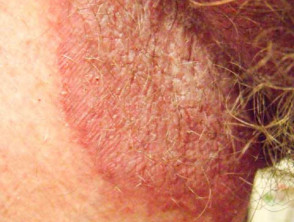
What is tinea cruris?
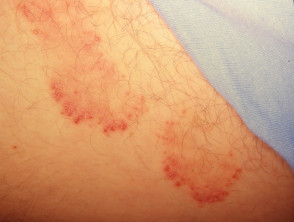
Tinea cruris, also known as ‘jock itch’, is a specific form of tinea due to a dermatophyte fungus affecting the groin, pubic region, and adjacent thigh. It presents as an acute or chronic asymmetrical rash.
Tinea cruris
Who gets tinea cruris?
Tinea cruris affects both sexes, with a male predominance (3:1). All ages can develop tinea cruris, adolescents and adults more commonly than children and the elderly. Tinea cruris can affect all races, being particularly common in hot humid tropical climates.
Predisposing factors for tinea cruris include:
- Longstanding tinea pedis
- Previous episodes of tinea cruris
- Occlusive clothing
- Obesity
- Excessive sweating (hyperhidrosis)
- Diabetes mellitus
- Topical steroid use.
What causes tinea cruris?
Tinea cruris is caused by a dermatophyte fungus, most commonly Trichophyton rubrum and Epidermophyton floccosum.
Spread of the infection to the groin is commonly from the feet (tinea pedis) or nails (tinea unguium) by scratching or use of contaminated towels or bed sheets.
What are the clinical features of tinea cruris?
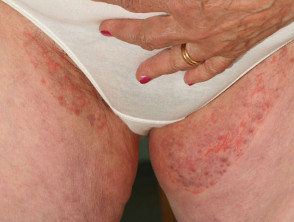
- Tinea cruris usually begins in the inguinal (groin) skin fold on one side which can evolve to become a bilateral but characteristically asymmetrical rash.
- The rash can extend down the inner aspect of the thigh or to the lower abdomen and pubic area.
- Involvement of the buttocks and perineum may be seen but there is typically sparing of the penis, scrotum, and vulva.
- Acute tinea cruris may present as a moist and exudative rash.
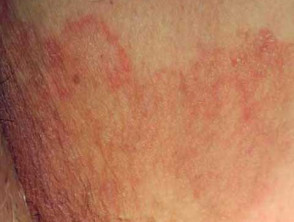
- Chronic tinea cruris presents as a large well-demarcated scaly plaque with a raised border and central clearing.
- Scale is most prominent at the leading edge of the plaque.
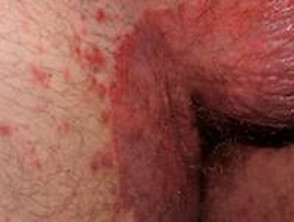
- Dermatophytic folliculitis may present as papules and pustules along the border.
- Tinea cruris is usually itchy.
- Wood lamp examination does not demonstrate fluorescence.
Tinea cruris
How do clinical features vary in differing types of skin?
Tinea cruris often causes marked hyperpigmentation in skin of colour.
Dermoscopy of tinea cruris
- Diffuse erythema
- Brown spots with white/yellow halo
- Follicular micropustules
- Morse code hairs — indicate invasion of vellus hairs
What are the complications of tinea cruris?
- Maceration and secondary infection with bacteria or candida
- Secondary excoriation, lichenification, and pigmentation
- Tinea incognito due to use of topical steroids
How is tinea cruris diagnosed?
Tinea cruris should be considered in the clinical setting of an asymmetrical scaly rash in the groin and confirmed on a skin scraping for mycology [see Laboratory tests for fungal infections].
Skin biopsy may be performed, usually to exclude other flexural skin conditions [see Skin diseases and conditions affecting body folds]. Histology demonstrates branching septate hyphae on special stains [see Tinea corporis pathology].
What is the differential diagnosis for tinea cruris?
- Flexural infections eg, candidal intertrigo, erythrasma
- Flexural dermatose eg, flexural psoriasis, seborrhoeic dermatitis, benign familial pemphigus
- Langerhans cell histiocytosis — a rare cause of a flexural rash in a very young child
Differential diagnosis of tinea cruris
What is the treatment for tinea cruris?
General and preventative measures
- Careful towelling after washing to avoid transfer of fungi from the feet
- Loose fitting clothing
- Treatment of triggers such as hyperhidrosis or obesity
- Topical antifungal powder after bathing
Specific measures
- Topical antifungal medication such as imidazoles or terbinafine
- Oral antifungal medication for extensive or recalcitrant infection, particularly in immunosuppressed patients eg, griseofulvin, terbinafine, itraconazole
- Treatment of tinea at other sites such as tinea pedis or tinea unguium
- Mild topical steroid can be used short-term to reduce itch, but is not appropriate as a monotherapy or long-term
What is the outcome for tinea cruris?
Tinea cruris clears with appropriate treatment in 80–90% of cases. However, recurrence is common, especially if predisposing factors are not addressed or antifungal treatment is stopped before mycological cure. Residual hyperpigmentation may persist in skin of colour.