What is deucravacitinib?
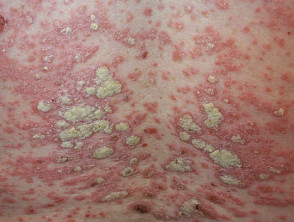
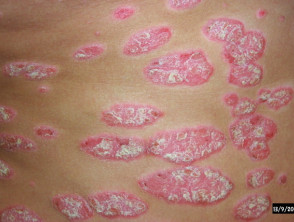
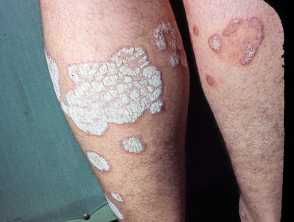
Deucravacitinib is a selective oral tyrosine kinase 2 (TYK2) inhibitor for the systemic treatment of moderate to severe plaque psoriasis and other immune-mediated diseases.
What is deucravacitinib used for?
Deucravacitinib (SOTYKTU™) was first approved in September 2022 by the US Food and Drug Administration (FDA) and subsequently in the European Union (EU) for the treatment of adults with moderate to severe plaque psoriasis who are candidates for systemic therapy or phototherapy.
Deucravacitinib was later approved in Japan for treatment of plaque psoriasis, generalised pustular psoriasis, and erythrodermic psoriasis.
Further clinical trials are underway to explore the efficacy of deucravacitinib for treatment of other immune-mediated diseases such as:
- Crohn disease and ulcerative colitis
- Cutaneous lupus erythematosus
- Discoid lupus erythematosus
- Systemic lupus erythematosus (SLE)
- Psoriatic arthritis.
How does deucravacitinib work?
Deucravacitinib is the first-in-class oral tyrosine kinase 2 (TYK2) inhibitor that acts via allosteric inhibition of the TYK2 regulatory pseudokinase (JH2) domain.
The precise mechanism of action explaining the link between TYK2 inhibition and therapeutic effectiveness of deucravacitinib is currently unknown. It is postulated that TYK2 pairs with other Janus kinase enzymes to stimulate cytokine-mediated inflammatory responses. Deucravacitinib targets this pathway to suppress the immune response; see: Janus kinase inhibitors.
What are the precautions and contraindications with deucravacitinib?
Precautions
- Pregnancy and breastfeeding — currently no safety information available; benefits of use during pregnancy or lactation should be balanced against potential risks.
- History of recurrent infections or underlying conditions that predispose to infection.
- History of serious infections or tuberculosis exposure.
- Liver disease.
- Known malignancy.
- Administration of live vaccines during treatment. See: Immunisation in immunosuppressed dermatology patients.
- Recommend to avoid concurrent treatment with other potent immunosuppressants.
Contraindications
- Hypersensitivity to deucravacitinib or its excipients.
- Clinically important active infections eg, tuberculosis (TB) or hepatitis B or C.
- Concurrent use with other potent immunosuppressants.
- Severe hepatic impairment (Child-Pugh C).
Deucravacitinib administration and monitoring
Deucravacitinib is a systemic therapy taken as a once-daily oral tablet.
Monitoring:
- Monitor for signs of infection before initiating and during treatment
- Pretreatment screening for hepatitis B and C, HIV +/- tuberculosis
- Baseline kidney function
- Lipids
- Liver function tests (LFTs)
- Creatine kinase (CK) may require monitoring if myopathy is suspected.
What are the benefits of deucravacitinib?
The POETYK PSO-2 phase III study found that 53% of patients with moderate to severe plaque psoriasis using deucravacitinib had a reduction of 75% or more in their Psoriasis Area and Severity Index (PASI) score after 16 weeks, compared to 9.4% of patients taking placebo, and 39.8% of patients on apremilast.
Deucravacitinib is conveniently administered, as it is an oral medication that can be taken at any time of day, with or without food. Ease of use is analogous to other plaque psoriasis therapies.
What are the disadvantages of deucravacitinib?
- Deucravacitinib is a potent immunosuppressant that may increase the risk of severe infections and malignancy.
- Risk of elevation of liver enzymes and triglycerides.
- Links have been made to increased risk of rhabdomyolysis.
- Deucravacitinib is relatively expensive.
- Benefits are not seen immediately but around 4 weeks after initiating treatment.
- Tolerance and efficacy largely depend on individual patient response to therapy.
- Limited information is available about the use of deucravacitinib outside of clinical trials.
- No evidence of efficacy for nail psoriasis.
What are the side effects and risks of deucravacitinib?
Clinical trials extending up to 52 weeks have shown that deucravacitinib is generally well tolerated.
Common side effects include:
- Nasopharyngitis
- Upper respiratory tract infections
- Headache.
Mucocutaneous side effects:
- Herpes simplex (HSV) infection
- Folliculitis
- Acne
- Aphthous ulcers.
Uncommon side effects:
- Hypertriglyceridemia
- Raised liver enzymes.
Serious adverse events:
- Hepatotoxicity
- Rhabdomyolysis
- Hypersensitivity reaction
- Malignancy
- Serious infections such as tuberculosis.
We suggest you refer to your national drug approval agency such as the Australian Therapeutic Goods Administration (TGA), US Food and Drug Administration (FDA), UK Medicines and Healthcare products regulatory agency (MHRA) / emc, and NZ Medsafe, or a national or state-approved formulary eg, the New Zealand Formulary (NZF) and New Zealand Formulary for Children (NZFC) and the British National Formulary (BNF) and British National Formulary for Children (BNFC).