Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Infections Follicular disorder
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Updated by Dr Oakley and Clare Morrison, Copy Editor. April 2014.
Introduction
Causes
Folliculitis due to infection
Folliculitis due to irritation from regrowing hairs
Folliculitis due to contact reactions
Folliculitis due to immunosuppression
Folliculitis due to drugs
Folliculitis due to inflammatory skin diseases
Buttock folliculitis
Folliculitis means an inflamed hair follicle due to any cause. The result is a tender red spot, often with a surface pustule.
Folliculitis may be superficial or deep. It can affect anywhere there are hairs, including chest, back, buttocks, arms, and legs. Acne and its variants are also types of folliculitis.
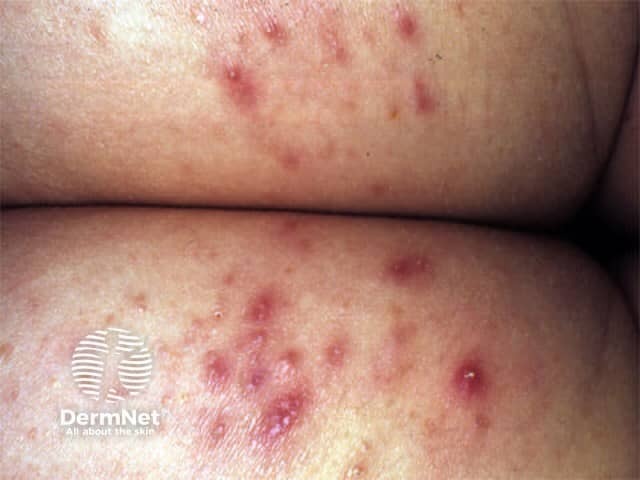
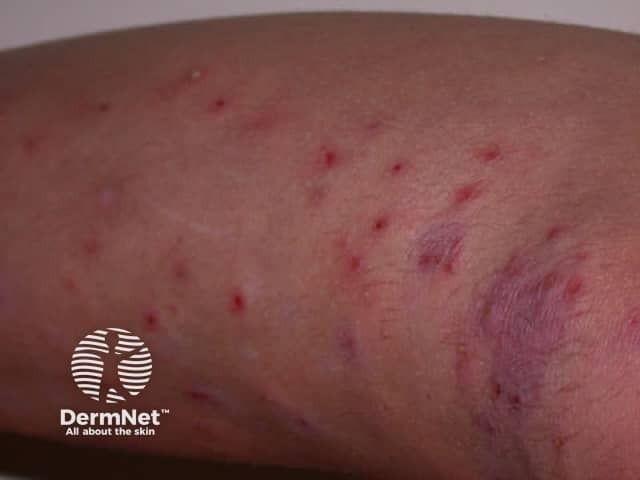
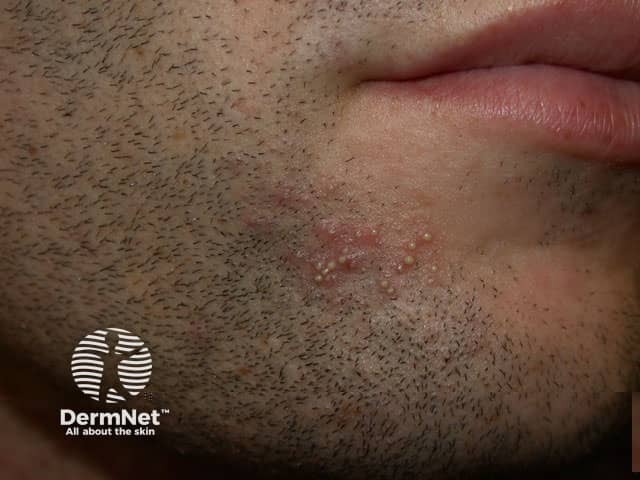

Superficial bacterial folliculitis
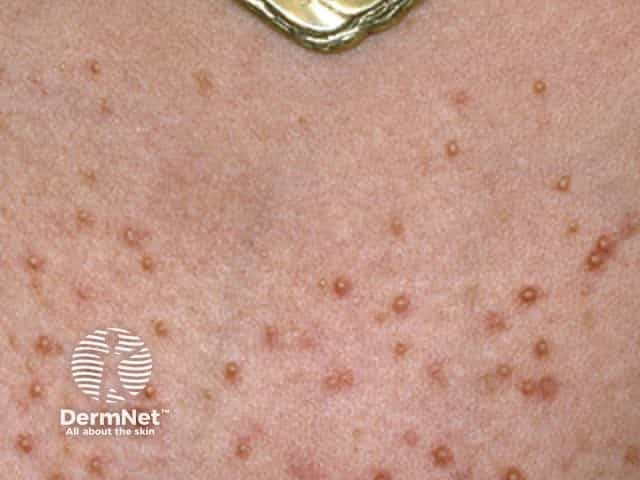
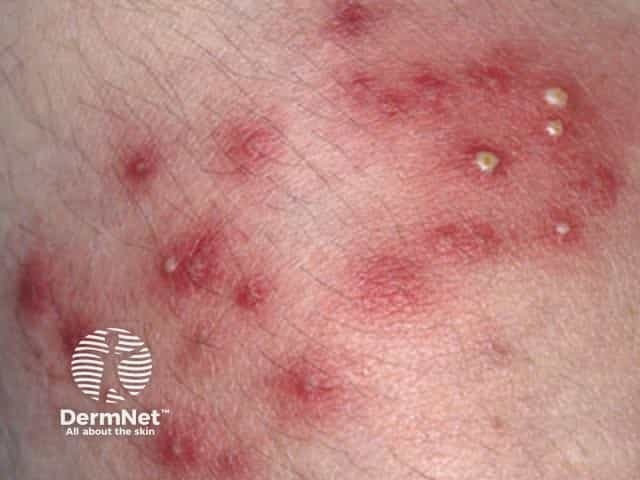
Superficial bacterial folliculitis
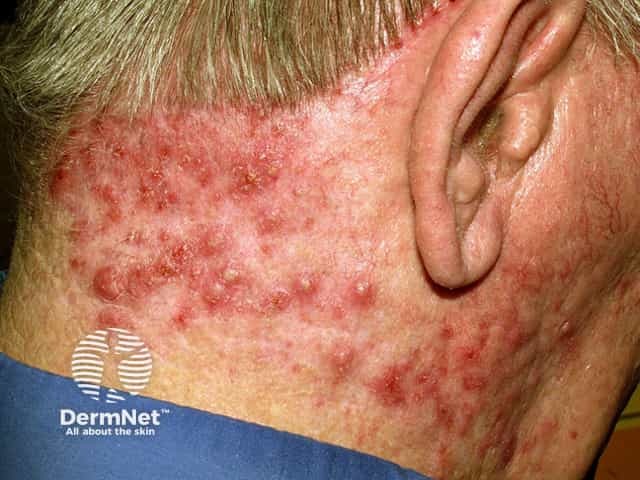
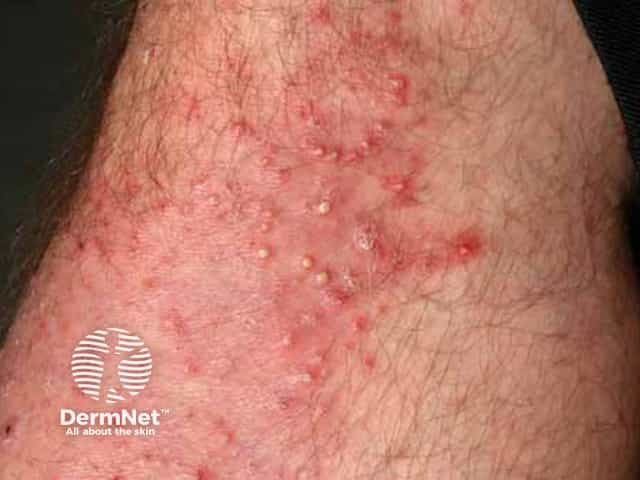
See more images of folliculitis.
Folliculitis can be due to infection, occlusion (blockage), irritation and various skin diseases.
Swabs should be taken from the pustules for cytology and culture in the laboratory to determine if folliculitis is due to an infection.
Bacterial folliculitis is commonly due to Staphylococcus aureus. If the infection involves the deep part of the follicle, it results in a painful boil. Recommended treatment includes careful hygiene, antiseptic cleanser or cream, antibiotic ointment, or oral antibiotics.
Spa pool folliculitis is due to infection with Pseudomonas aeruginosa, which thrives in warm water. Gram-negative folliculitis is a pustular facial eruption also due to infection with Pseudomonas aeruginosa or other similar organisms. When it appears, it usually follows tetracycline treatment of acne but is quite rare.
The most common yeast to cause a folliculitis is Pityrosporum ovale, also known as Malassezia. Malassezia folliculitis (pityrosporum folliculitis) is an itchy acne-like condition usually affecting the upper trunk of a young adult. Treatment includes avoiding moisturisers, stopping any antibiotics and using topical antifungal or oral antifungal medication for several weeks.
Candida albicans can also provoke a folliculitis in skin folds (intertrigo) or the beard area. It is treated with appropriate topical or oral antifungal agents.
Ringworm of the scalp (tinea capitis) usually results in scaling and hair loss, but sometimes results in folliculitis. In New Zealand, cat ringworm (Microsporum canis) is the commonest organism causing scalp fungal infection. Other fungi such as Trichophyton tonsurans are increasingly reported. Treatment is with an oral antifungal agent for several months.
Folliculitis may be caused by the herpes simplex virus. This tends to be tender and resolves without treatment in around ten days. Severe recurrent attacks may be treated with aciclovir and other antiviral agents.
Herpes zoster (the cause of shingles) may present as folliculitis with painful pustules and crusted spots within a dermatome (an area of skin supplied by a single nerve). It is treated with high-dose aciclovir.
Molluscum contagiosum, common in young children, can present with follicular umbilicated papules, usually clustered in and around a body fold. Molluscum may provoke dermatitis.
Folliculitis on the face or scalp of older or immunosuppressed adults may be due to colonisation by hair follicle mites (demodex). This is known as demodicosis.
The human infestation, scabies, often provokes folliculitis, as well as non-follicular papules, vesicles and pustules.
Folliculitis may arise as hairs regrow after shaving, waxing, electrolysis, or plucking. Swabs taken from the pustules are sterile — there is no growth of bacteria or other organisms. In the beard area irritant folliculitis is known as pseudofolliculitis barbae (or folliculitis barbae if associated with an infection).
Irritant folliculitis is also common on the lower legs of women (shaving rash). It is frequently very itchy. Treatment is to stop hair removal, and not begin again for about three months after the folliculitis has settled. To prevent reoccurring irritant folliculitis, use a gentle hair removal method, such as a lady's electric razor. Avoid soap and apply plenty of shaving gel, if using a blade shaver.
Paraffin-based ointments, moisturisers, and adhesive plasters may all result in a sterile folliculitis. If a moisturiser is needed, choose an oil-free product, as it is less likely to cause occlusion.
Coal tar, cutting oils and other chemicals may cause an irritant folliculitis. Avoid contact with the causative product.
Overuse of topical steroids may produce a folliculitis. Perioral dermatitis is a facial folliculitis provoked by moisturisers and topical steroids. Perioral dermatitis is treated with tetracycline antibiotics for six weeks or so.
Eosinophilic folliculitis is a specific type of folliculitis that may arise in some immune-suppressed individuals such as those infected by human immunodeficiency virus (HIV) or those who have cancer.
Folliculitis may be due to drugs, particularly corticosteroids (steroid acne), androgens (male hormones), adrenocorticotrophic hormone (ACTH), lithium, isoniazid (INH), phenytoin and B-complex vitamins. Treatment with protein kinase inhibitors (epidermal growth factor receptor inhibitors) and targeted therapy for metastatic melanoma (vemurafenib, dabrafenib) nearly always results in folliculitis.
Certain uncommon inflammatory skin diseases may cause permanent hair loss and scarring because of deep-seated sterile folliculitis. These include:
Treatment depends on the underlying condition and its severity. A skin biopsy is often necessary to establish the diagnosis.
Acne variants
Acne and acne-like (acneform) disorders are also forms of folliculitis. These include:
The follicular occlusion syndrome refers to:
Treatment of the acne variants may include topical therapy as well as long courses of tetracycline antibiotics, isotretinoin (vitamin-A derivative) and, in women, antiandrogenic therapy.
Folliculitis affecting the buttocks is quite common in males and females.