Introduction
Pseudomonas species are Gram-negative rod-shaped bacteria widespread in water and soil. Infections of the skin or soft tissues by Pseudomonas aeruginosa and other Pseudomonas spp. range from superficial discolourations to serious and life-threatening because these bacteria are invasive and toxigenic.
What causes pseudomonas skin infections?
Pseudomonas aeruginosa is commonly found transiently on the skin, especially in the axillary and anogenital regions, and readily colonises ulcers and moist skin. However, healthy people do not normally develop pseudomonas infection. Pseudomonas is considered to be an opportunistic infection causing serious disease in immunocompromised patients, damaged tissue, or following accidental intravenous access.
Pseudomonas species can be transmitted in hospitals due to contaminated surfaces and via hands of staff, and is responsible for approximately 10% of all nosocomial infections.
Who is at risk for pseudomonas skin infections?
Patients at highest risk for these infections include those with:
- Malignancies
- HIV/AIDs
- Burns
- Diabetes
- Intravenous catheter
- Indwelling urinary catheter
- Surgery
- Trauma.
What are the clinical features of a pseudomonas skin infection?
Signs of pseudomonas infection vary depending upon the site of the infection, but can include:
- Erythematous (red) lesions that can become haemorrhagic or necrotic
- Acneform rash
- Deep abscess
- Subcutaneous nodules
- Cellulitis
- Necrotising fasciitis
- Black or purple discolouration or eschar.
Pseudomonas skin infection
What are the different types of pseudomonas skin infections?
- External otitis is the most common infection due to Pseudomonas spp. particularly in the tropics and in swimmers: patients present with pain, swelling, and redness of the external portions of the ear as well as a purulent discharge. Malignant (necrotising) external otitis is more serious affecting diabetic patients presenting as severe pain and discharge. Damage to cranial nerves, particularly the facial nerve, is common.
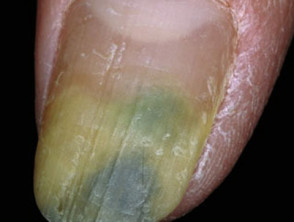
- Chronic paronychia and onycholysis involving Pseudomonas spp. presents as a greenish discolouration of the nail.
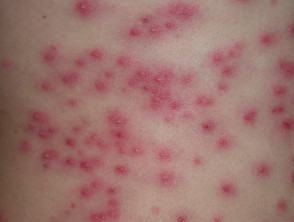
- Spa pool folliculitis is a pseudomonas infection acquired in inadequately chlorinated hot tubs. Patients present with itchy follicular papules and pustules on any part of the body submerged in the tub.
- Puncture wounds of the foot can frequently become infected with Pseudomonas species and the patient will present with a sweet, fruity-smelling discharge. Cellulitis and osteomyelitis are common complications.
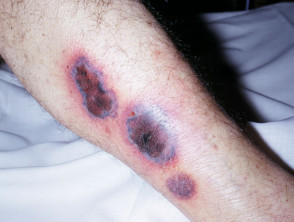
- Ecthyma gangrenosum typically develops in neutropenic patients as erythematous, ulcerated, purple or black skin lesions in the axillary, inguinal, or anogenital areas.
- Thermal burn wounds with an eschar can be populated by Pseudomonas spp. resulting in bacteraemia (bacteria in the blood stream), a complication with a high mortality rate.
- Chronic leg ulcer colonisation with Pseudomonas spp is recognised by a malodorous greenish superficial crust.
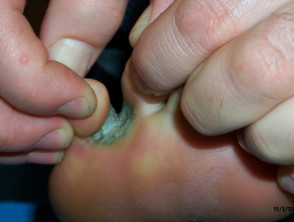
- Tropical immersion foot develops in the toeweb spaces as areas of maceration with a greenish tinge.
- Pseudomonas infection of the umbilical stump in the neonate present as a spreading erythema associated with the typical green fruity-smelling discharge.
- Pseudochromhidrosis due to Pseudomonas aeruginosa presents as green-black sweat.
Pseudomonas nail infection
What are the complications from pseudomonas skin infections?
The most serious complication of a pseudomonas skin or soft tissue infection is bacteraemia following contaminated intravenous fluids, drugs, or antiseptics used during placement of an intravenous line. This can be fatal.
How are pseudomonas skin infections diagnosed?
Pseudomonas infections are suspected on physical examination when there is a a greenish or blackish, fruity-smelling discharge. They are confirmed by laboratory studies of cultures taken from the affected area.
What are the treatments for pseudomonas skin infections?
Treatment is determined by the site of the pseudomonas infection and its severity. It may include:
- Antibiotics
- Irrigation with a 1% acetic acid solution for otitis externa together with topical polymyxin B, or fluoroquinolones in cases of a more severe infection
- Debridement of necrotic tissue and/or drainage of abscesses as an adjuvant to antibiotic therapy
- Amputation of affected limb (in rare cases).