Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Pigmentary disorders Terminology
Author: Ken Hiu-Kan Ip, Medical Student, University of Auckland, New Zealand; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand; Copy Editor: Clare Morrison, June 2014. Updated by Dr Ebtisam Elghblawi and Dr Oakley in October 2017.
Introduction Demographics Causes Complications Management Outlook
Melanonychia is brown or black discolouration of a nail. It may be diffuse or take the form of a longitudinal band.
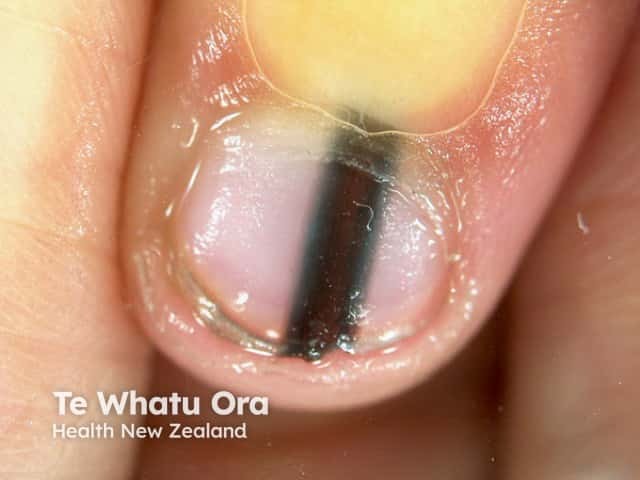
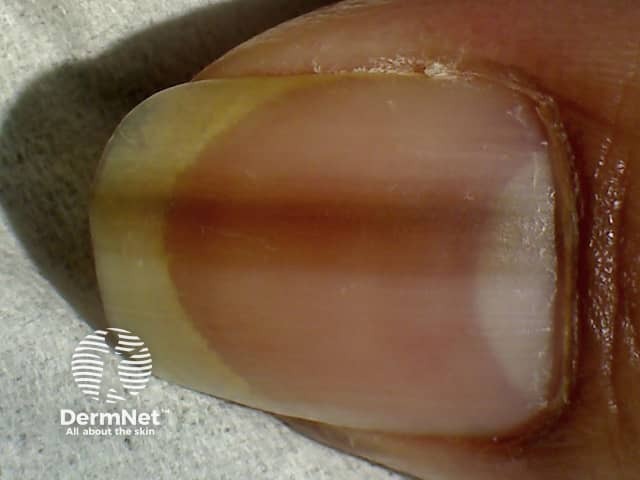
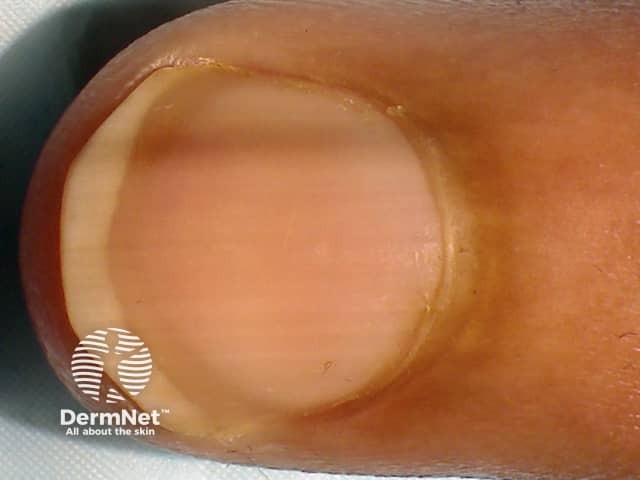
See more images of melanonychia.
Melanonychia can present in individuals of all ages, including children, and affects both sexes equally. It is more prevalent in people with skin of colour, especially Fitzpatrick skin type V and VI.
Melanonychia can also be associated with genetic disorders, injury, medications, nutritional deficiency, endocrine disease, connective tissue disease, inflammatory skin disease, a local tumour, or nail infection.
The nail plate is a hard, translucent structure made of keratin. It is not normally pigmented. Melanocytes typically lie dormant in the proximal nail matrix where the nail originates. Melanin is deposited into the growing nail when melanocytes are activated, resulting in a pigmented band — this is longitudinal melanonychia.
The deposition of melanin in the nail plate can result from 2 processes:
Melanocytic hyperplasia refers to an increased number of melanocytes within the nail matrix. This can represent a benign or malignant process.
Melanocytic naevi arise more commonly in children. Histologically there are nests of naevus cells.
Lentigines are seen more commonly in adults. Nests are absent.
Melanoma of the nail unit most commonly affects the thumbs, index fingers and big toes.
Melanocytic activation is an increase in the production and deposition of melanin into the nail cells (onychocytes), without an increase in the number of melanocytes. The causes of melanocytic activation are listed in the table below.
Melanonychia associated with melanocytic activation |
|
|---|---|
Physiological (functional) |
Racial variation |
Trauma |
Nail biting, chewing, breaking and picking |
Inflammatory skin disease |
Psoriasis |
Nonmelanocytic lesions |
|
Nutritional deficiency |
Vitamin B12 or folate deficiency |
Endocrine disorders |
|
Another systemic disease |
Haemosiderosis |
Syndromes |
Laugier-Hunziker syndrome |
Iatrogenic |
|
Medications |
Chemotherapy agents (especially hydroxyurea, busulfan, bleomycin, adriamycin, doxorubicin, cyclophosphamide, 5-fluorouracil |
Pathogens can cause an irregular melanonychia as they stimulate inflammation activating melanocytes. For example:
External agents can stain the nails.
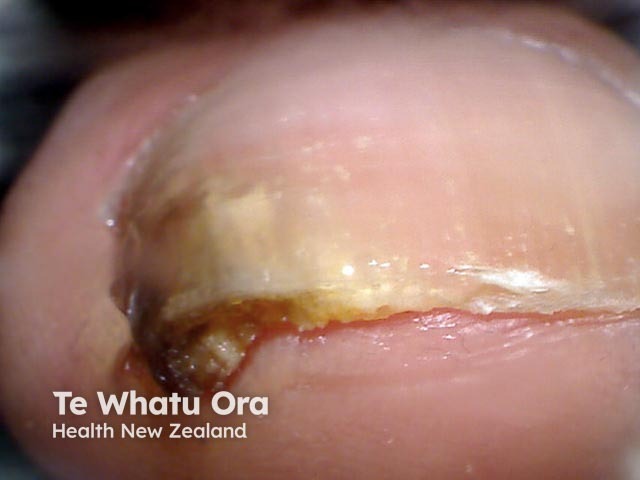
Pigmented onychomycosis
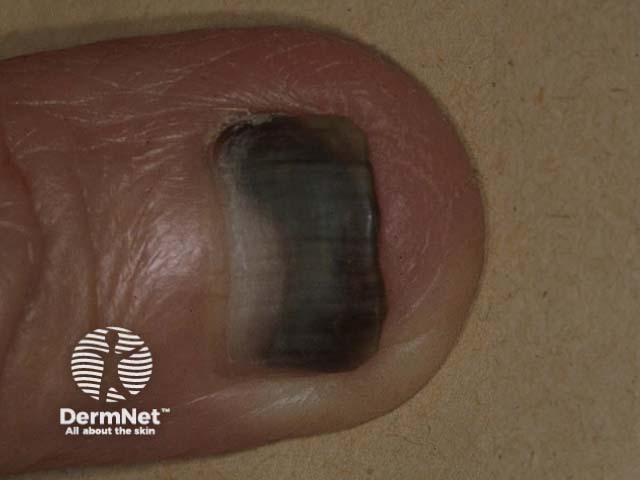
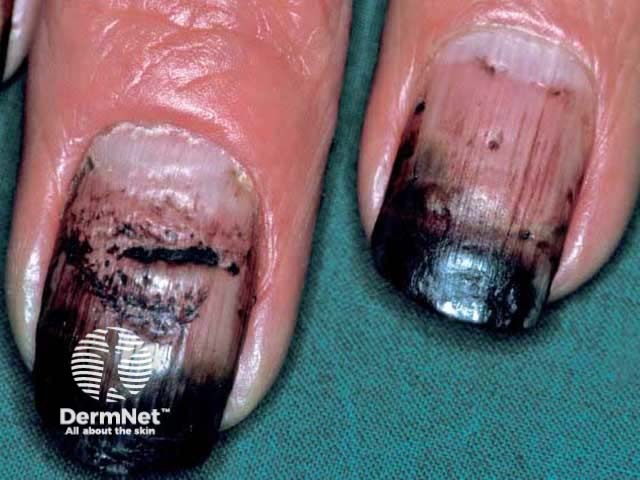
Complications depend on the cause of melanonychia.
Where melanonychia is attributed to a benign cause, no further treatment is necessary.
The management of melanoma of the nail unit requires complete excision of the tumour and may require amputation of the digit.
Melanonychia tends to persist, except when it is related to medication — in which case it fades following its withdrawal.