Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Lesions (cancerous) Lesions (benign)
Last Reviewed: November, 2025
Authors: Dr Samuel Morriss, Resident; A/Prof Susan Robertson, Director of Dermatology, The Royal Children’s Hospital, Victoria, Australia (2024)
Peer reviewed by: Dr James A. Ida, Dermatologist, Veterans Administration, USA (2025)
Previous contributors: Vanessa Ngan, Staff Writer; Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand (2003)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department.
Introduction
Clinical significance
Demographics
Causes
Clinical features
Naevus differences
Diagnosis
Differential diagnoses
Treatment
Outcome
An atypical melanocytic naevus (or simply, atypical naevus) is a benign, acquired melanocytic naevus with unusual features.
Atypical naevi are commonly referred to as dysplastic naevi. However, the two terms are not technically interchangeable (see below).
Atypical naevi are a marker for increased risk of developing cutaneous melanoma. This risk rises proportionally with the number of atypical naevi present.
Compared to those without atypical naevi, individuals with:
The risk of a solitary atypical naevus transforming into melanoma is low, though progression can rarely occur.
Atypical naevi typically develop in childhood and early adolescence, but they can arise at any age. The prevalence of atypical naevi in White communities ranges from 5.2% to 12.0%.
Data on the prevalence in communities of skin of colour are not available.
Atypical naevi can be sporadic or familial (inherited).
Risk factors include:
The unregulated use of melanotropic peptides (eg, melanotan I and II) has also been associated with changes in existing naevi and the development of new sporadic naevi, both of which may display clinically atypical features.
Sporadic atypical naevi tend to accumulate more somatic mutations than common naevi, but fewer mutations than melanoma. Additionally, the mutational profiles found in melanoma (eg, mutations in CDKN2A, PTEN and CDK4) are not found in sporadic atypical naevi.
Some authors propose that the relatively large size of most atypical naevi may be due to longer telomeres, leading to decreased cellular senescence.
Familial atypical mole melanoma (FAMM) syndrome is an autosomal dominant genodermatosis characterised by:
FAMM syndrome associations:
About 5-10% of melanomas are hereditary, with 45% of those familial melanomas occurring in association with a germline CDKN2A mutation, or more rarely (1%) with a CDK4 mutation. Mutations in either of these genes result in the loss of tumour suppressor function, promoting uncontrolled proliferation and decreased apoptosis.
Other terms for FAMM syndrome include:
Atypical naevi, like common melanocytic naevi, are composed of naevus cells (specialised melanocytes). However, atypical naevi are distinguished by any combination of the following features:
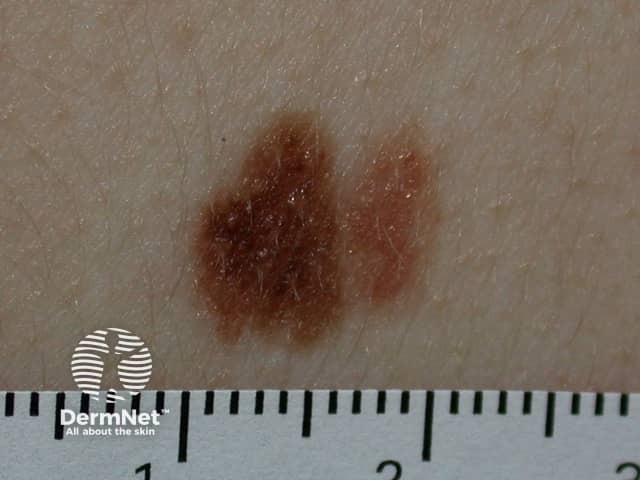
Atypical naevus
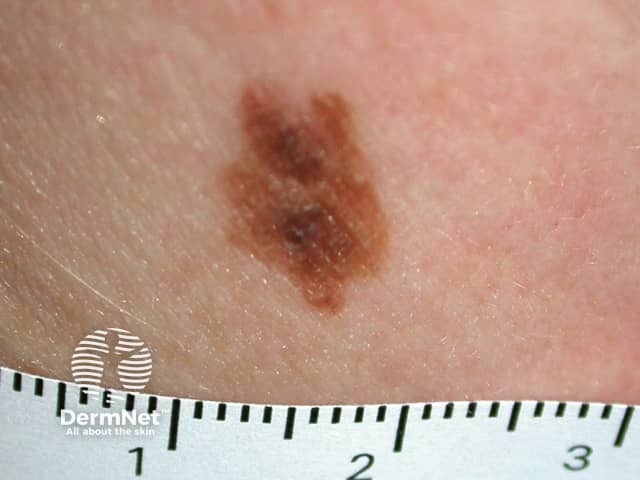
Atypical naevus
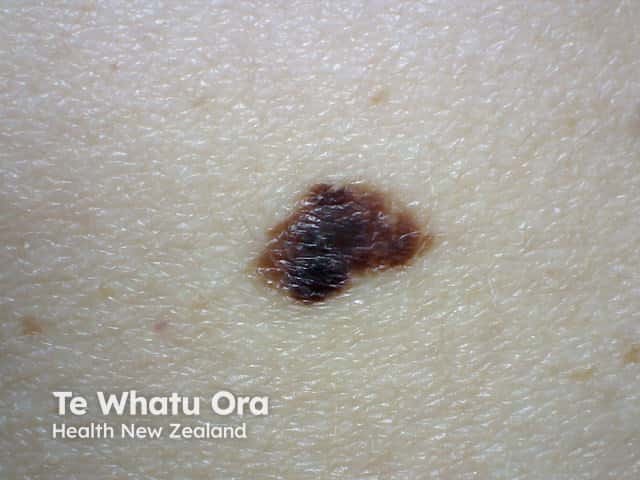
Atypical naevus
The term dysplastic naevus refers to a naevus with a specific microscopic appearance. That is, a dysplastic naevus is a histologic, not a clinical, diagnosis.
Only a minority of clinically atypical naevi fulfil microscopic criteria for dysplastic naevus. Conversely, many histologically dysplastic naevi appear clinically banal (eg, small and uniform in colour and structure).
While the name ‘dysplastic naevus’ might suggest these moles are premalignant or direct precursors to melanoma, evidence does not support this.
Rare reports exist of dysplastic naevi progressing to melanoma, but routine removal of dysplastic naevi does not prevent melanoma. Most melanomas arise de novo, rather than from pre-existing naevi.
Key histopathological features of a dysplastic naevus are listed below.
See: Melanocytic naevus pathology
Atypical naevi are typically diagnosed clinically during a skin examination, aided by dermoscopy.
For patients with numerous naevi, there is often a ‘signature naevus’ — a predominant pattern of naevi with shared clinical and dermoscopic features. Identification of an outlier naevus that does not fit this signature appearance, known as the ‘ugly duckling’ sign, should prompt consideration for biopsy/excision and histopathologic examination to rule out melanoma.
The dermoscopic characteristics listed below are used to classify atypical naevi.
*Note: eccentric peripheral hypo/hyperpigmentation can be seen in both atypical naevi and melanoma. This finding should be regarded as suspicious and warrants consideration for biopsy/excision to rule out melanoma.
There are currently no reliable clinical or histologic features that can predict whether an individual atypical naevus will transform into melanoma. Therefore, routine prophylactic excision of all atypical naevi is not recommended.
Excision considerations:
Because individuals with atypical naevi have a higher lifetime risk of melanoma, they should:
Atypical melanocytic naevi are benign and rarely undergo malignant transformation. However, their presence indicates an increased risk of developing melanoma.