Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Lesions (cancerous) Diagnosis and testing
Author(s): A/Prof Amanda Oakley, Dermatologist, New Zealand (1997). Updated Nov 2017; further update Dr Ian Coulson, Dermatologist, United Kingdom (2023)
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Treatment
Prevention
Outlook
Intraepidermal squamous cell carcinoma (SCC) is a common superficial form of keratinocyte cancer. It is also known as Bowen disease, intraepidermal carcinoma (IEC) and carcinoma in situ (SCC in situ).
Intraepidermal SCC is derived from squamous cells, the flat epidermal cells that make keratin, the horny protein that makes up skin, hair and nails. ‘Intraepidermal’ and ‘in situ’ mean the malignant cells are confined to the tissue of origin, in this case, the epidermis.
Risk factors for intraepidermal SCC include:
Up to 50% of patients with intraepidermal SCC have other keratinocytic skin cancers, mainly basal cell carcinoma.
Ultraviolet radiation (UV) is the main cause of intraepidermal SCC. It damages the skin cell nucleic acids (DNA), resulting in a mutant clone of the gene p53, setting off uncontrolled growth of the skin cells. UV also suppresses the immune response, preventing recovery from damage.
Human papillomavirus (HPV) is another major cause of intraepidermal SCC. Oncogenic strains of HPV are the main cause of squamous intraepithelial lesions (SIL), that is, squamous cell carcinoma in situ in mucosal tissue.
Intraepidermal SCC presents as one or more irregular scaly plaques of up to several centimetres in diameter. They are often an orange-red colour but may also be brown.
Although intraepidermal SCC may arise on any area of skin, it is most often diagnosed on sun-exposed sites of the ears, face, hands and lower legs. When there are many plaques, distribution is not symmetrical (unlike psoriasis).
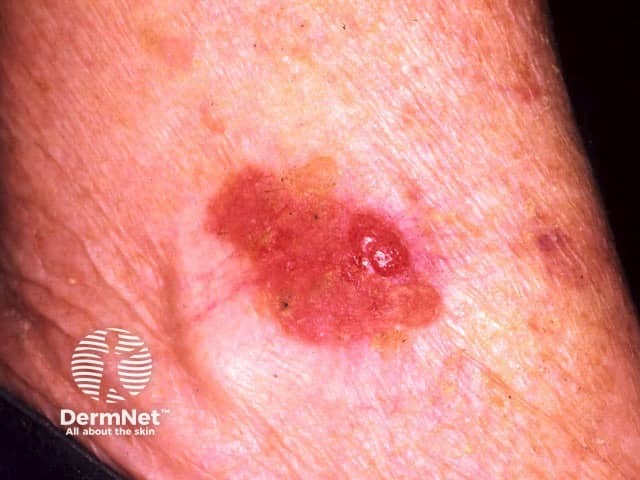
Squamous cell carcinoma
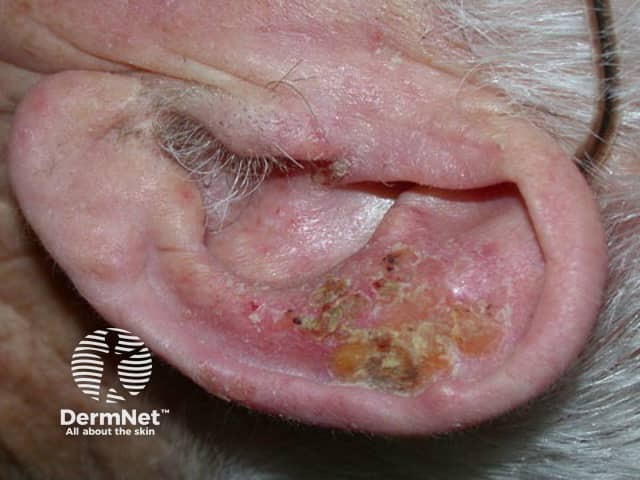
Squamous cell carcinoma
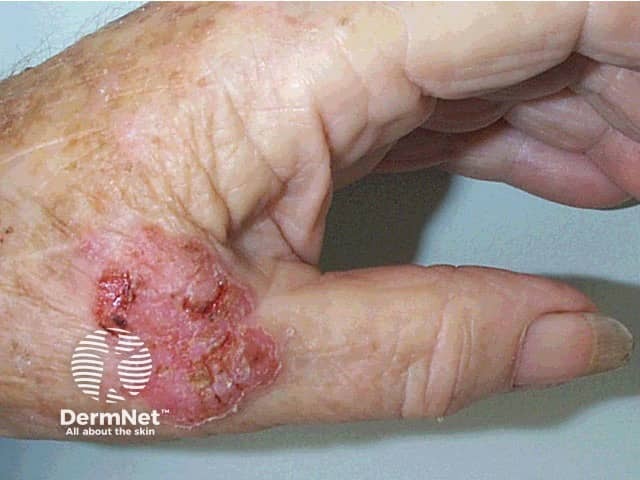
Squamous cell carcinoma
See more images of intraepidermal SCC ...
Intraepidermal SCC may start to grow under a nail when it results in a red streak (erythronychia) that later may destroy the nail plate.

Bowen disease of nail
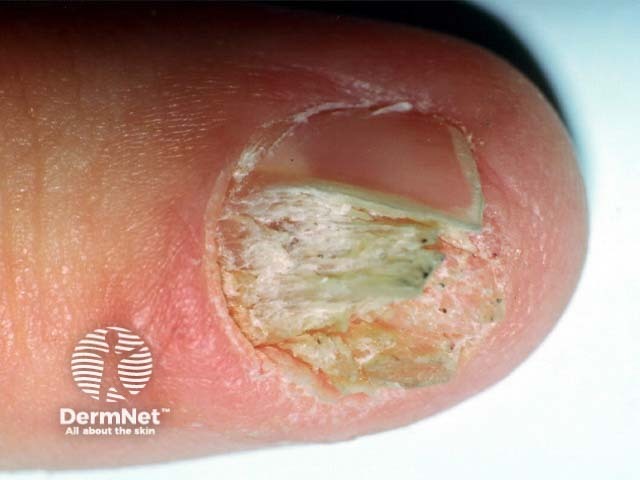
Bowen disease of nail
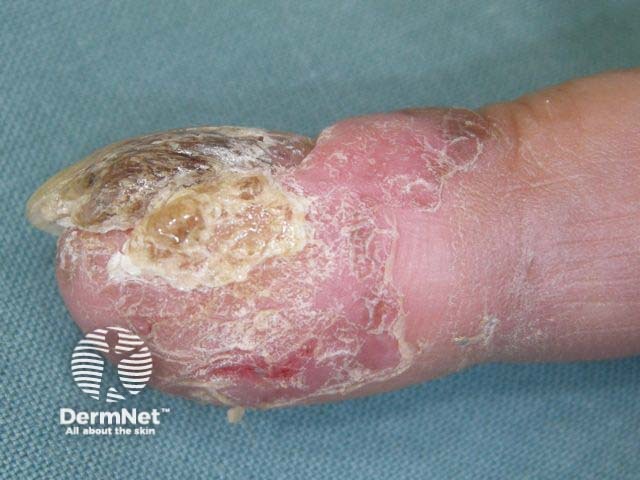
Squamous cell carcinoma in situ
Invasive SCC arises in about 5% of intraepidermal SCC lesions.
Intraepidermal SCC is often recognised clinically. Dermatoscopy of a red scaly irregular plaque is supportive if it reveals crops of rounded and coiled blood vessels.
Diagnosis may be confirmed by biopsy; histology reveals full thickness dysplasia of the epidermis.
As intraepidermal SCC is confined to the surface of the skin, there are various ways to remove it. Recurrence rates are high, whatever method is used, particularly in immune suppressed patients.
As the risk of invasive SCC is low, it may not be necessary to remove all lesions, particularly in elderly patients. Keratolytic emollients containing urea or salicylic acid may be sufficient to improve symptoms.
Solitary lesions can be cut out, and the defect repaired by stitching it up. Excision is often recommended if there is suspicion of invasive SCC.
Superficial skin surgery refers to shave, curettage and electrosurgery, and is an excellent choice for solitary or few hyperkeratotic lesions. The lesion is sliced off or scraped out; then the base is cauterised. Dressings are applied to the open wound to encourage moist wound healing over the next few weeks.
Cryotherapy means removing a lesion by freezing it, usually with liquid nitrogen. Moderately aggressive cryotherapy is suitable for multiple, small, flat patches of intraepidermal SCC. It leaves a permanent white mark at the site of treatment.
5-fluorouracil cream contains a cytotoxic agent and can be applied to multiple lesions. The cream may be used for intraepidermal SCC for four weeks and repeated if necessary. It causes a vigorous skin reaction that may ulcerate. A combination product of 5-fluorouracil with calcipotriol, used twice daily for 5-10 days, had favourable response rates over monotherapy.
Imiquimod cream is an immune response modifier used off-licence to treat intraepidermal SCC. It is applied 3–5 times weekly for 4–16 weeks and causes an inflammatory reaction.
Photodynamic therapy (PDT) refers to treatment with a photosensitiser (a porphyrin chemical) that is applied to the affected area before exposing it to a strong source of visible light. The treated area develops an inflammatory reaction and then heals over a couple of weeks or so. The best studied, methyl levulinate cream PDT used off licence, provides high cure rates for intraepidermal SCC on the face or lower legs, with excellent cosmetic results. The main disadvantage is the pain experienced by many patients during treatment.
Other treatments occasionally used in the treatment of intraepidermal SCC include:
Meticulous sun protection at any time of life can reduce the number of intraepidermal SCCs and is particularly important for ageing, sun-damaged white skin; and in patients that are immune suppressed by disease, for example with human immunodeficiency virus (HIV) infection, or by medications.
Intraepidermal SCC may recur months or years after treatment. The same procedure can be repeated or another method used.
Patients that have been treated for intraepidermal SCC are at risk of developing new lesions of intraepidermal SCC. They are also at increased risk of other skin cancers, especially squamous cell carcinoma, basal cell carcinoma and melanoma.