Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: February, 2025
Authors: Dr Nageswary Nadarajah, Acute Medical Registrar, Hull Royal NHS Foundation Trust; Dr Faraz Imran, Consultant Dermatologist, Castlehill Hospital, United Kingdom (2025).
Previous contributors: Dr Amanda Oakley, Dermatologist, NZ (1998; 2015)
Peer reviewed by: Dr Sally-Anne Ting, Sir Charles Gairdner Hospital, Australia (2025)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Complications
Acute febrile neutrophilic dermatosis is a rare skin condition characterised by a sudden onset of painful, inflamed skin lesions associated with fever.
Acute febrile neutrophilic dermatosis also has the eponymous name, Sweet syndrome, named after Dr Robert Douglas Sweet from Plymouth, England, who first described it in 1964.
Acute febrile neutrophilic dermatosis typically occurs in women aged between 30-60 years old. It can also develop in men, children (rarely), and the elderly. There is also no identifiable racial preference.
Most affected individuals have underlying associated conditions.
The exact cause of this condition remains unknown, but possible causes are:
The syndrome can manifest in three clinical settings:
Acute febrile neutrophilic dermatosis may occur once or repeatedly. It is characterised by some or all of the following symptoms:
Skin lesions may be few or numerous. They are characteristically tender and may persist from days to weeks. Lesions commonly affect the face, neck, and upper extremities. In some patients, they arise only in sun-exposed areas.
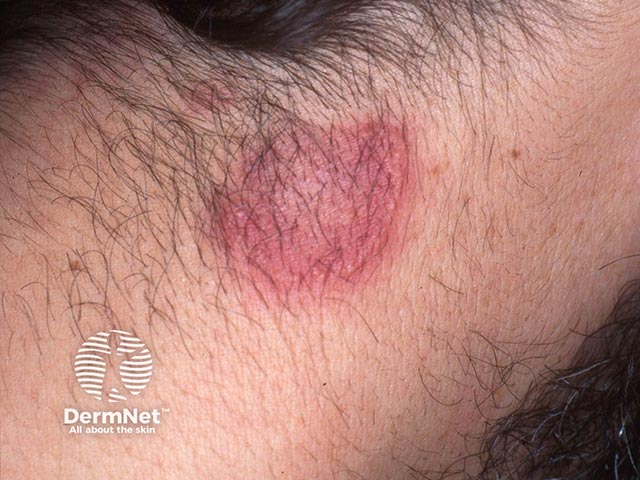
Annular plaque on the neck due to acute febrile neutrophilic dermatosis - there is a pseudovesicular edge
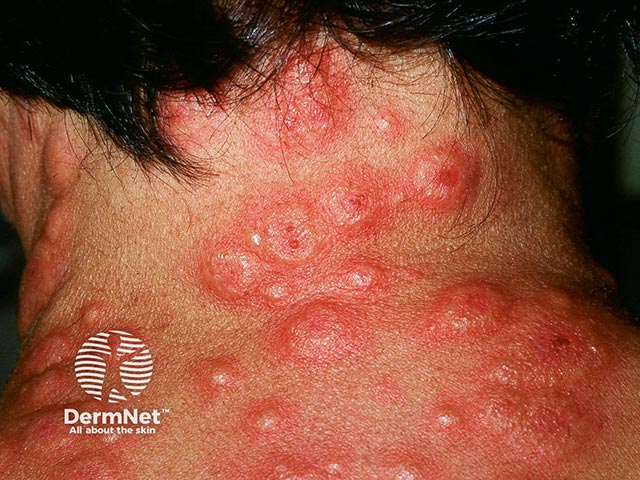
Acute febrile neutrophilic dermatosis on the neck (AFND-patient4)
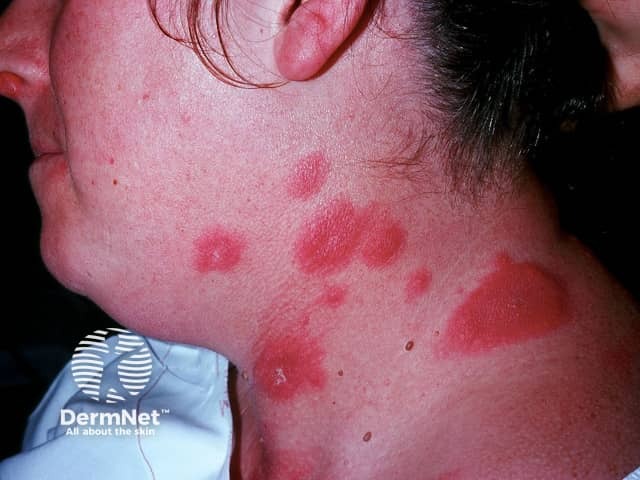
Plaques of tender acute febrile neutrophilic dermatosis on the neck
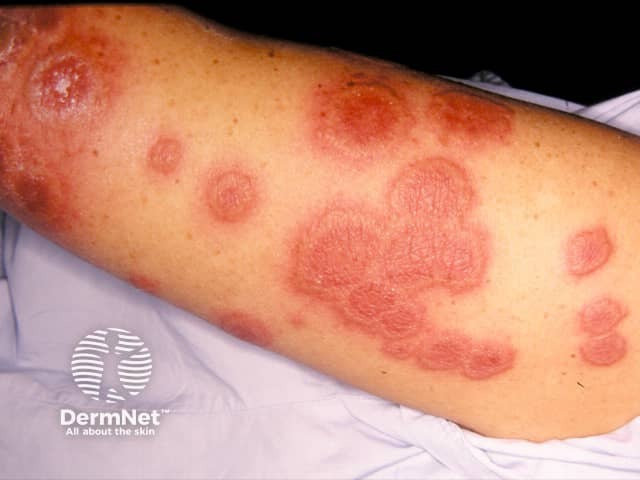
Annular lesions of acute febrile neutrophilic dermatosis
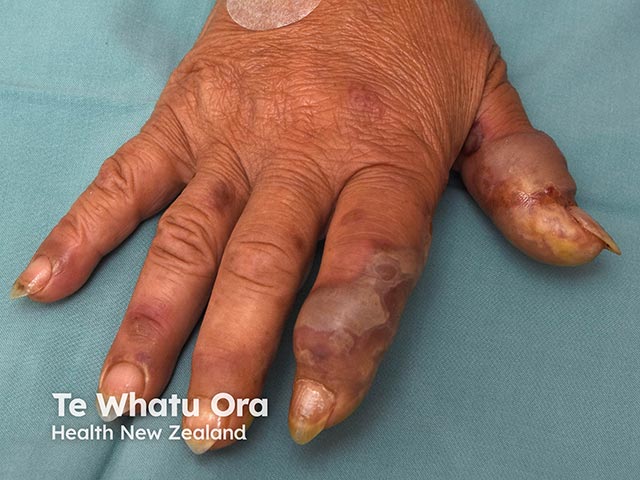
Oedematous lesions on the fingers due to acute febrile neutrophilic dermatosis of the dorsal hands (AFND-patient2)
Sweet syndrome may have a range of appearances:
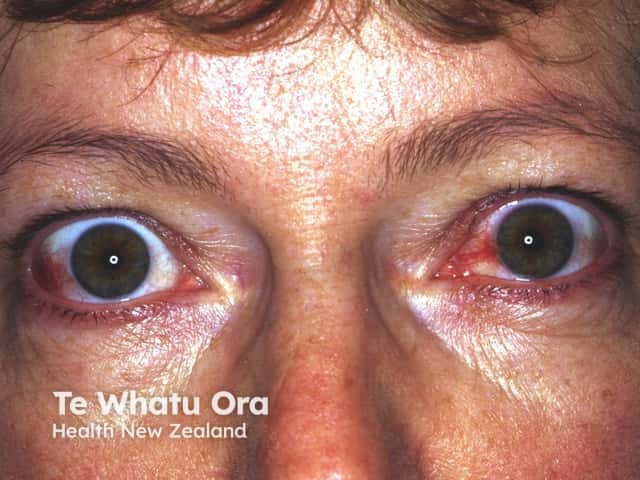
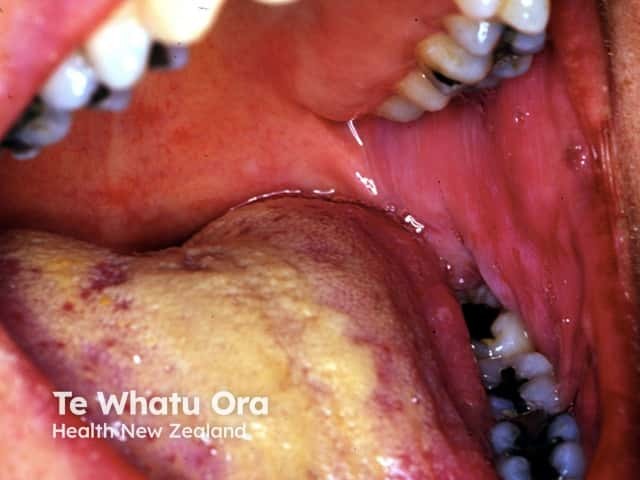
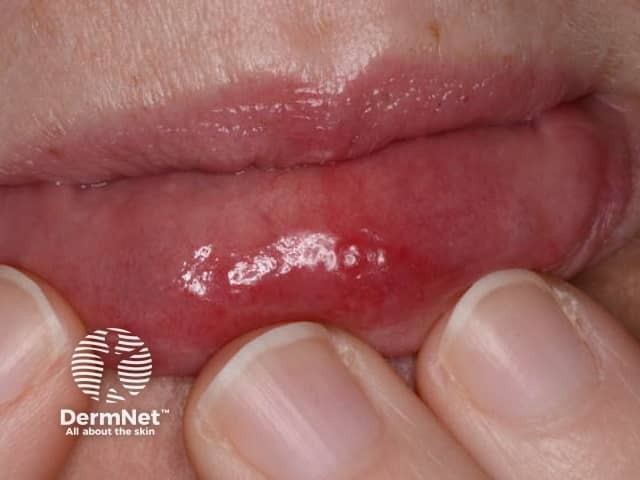
In some patients, acute febrile neutrophilic dermatosis can affect the eyes and the inner lining of the mouth, including the tongue and lips, causing erosions or ulcerations.
Sweet syndrome can present with dusky or a more violaceous colouration in darker skin. Post-inflammatory hyperpigmentation (area of darker skin after wound healing) is also more prominent and lasts longer in darker skin.
There is no specific testing for acute febrile neutrophilic dermatosis but, there is a diagnostic criterion developed to help identify it. To diagnose Sweet syndrome, two major criteria combined with two of the four minor criteria must be met.
The following tests can be performed to determine if an underlying cause of Sweet syndrome is present, especially occult malignancies:
It is also worth noting that there are several clinical and histopathological (tissue changes related to a disease) variants of Sweet syndrome which may alter management.
Treatment of acute febrile neutrophilic dermatosis usually results in rapid improvement in symptoms. Usually, systemic corticosteroids such as predniso(lo)ne, are prescribed in a dose of 30–60 mg daily. The fever, skin lesions and other symptoms clear up within a few days. However, lower doses of corticosteroids are often required for several weeks to months to prevent reoccurrence.
Several other medications may be tried when systemic corticosteroids are ineffective or contraindicated. Those reported to be useful include:
In some cases, acute febrile neutrophilic dermatosis is resistant to treatment.
Prior knowledge and high index of suspicion in high-risk patients (with associated disease such as IBD, AML or taking commonly associated medications), and early management may help prevent the symptoms or complications associated with Sweet syndrome.
Acute febrile neutrophilic dermatosis usually resolves eventually, without leaving a mark or scar, with or without treatment though the lesions may persist for weeks to months.
Generally, there is a single episode of Sweet syndrome, but approximately 50% of patients may develop repeated episodes. This is more likely in idiopathic or in patients with underlying cancer. Rarely, it may persist for years.