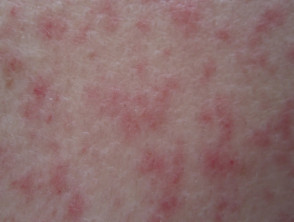
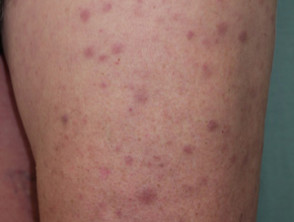
What is leukaemia cutis?
Leukaemia cutis refers to the infiltration of the skin with leukaemia cells.
Leukaemia is the name given to a group of blood disorders in which there is a malignant proliferation of white cells (leukocytes). The leukaemia may be acute or chronic, due to proliferation of lymphocytes or more commonly, myeloid cells (the neutrophils). Clonal expansion or proliferation of identical abnormal cells mainly occurs in the bone marrow.
The most common types of leukaemia are:
- Acute lymphoblastic leukaemia (ALL)
- Chronic lymphoblastic leukaemia (CLL)
- Acute myeloid leukaemia (AML)
- Chronic myeloid leukaemia (CML)
- Hairy cell leukaemia
- Acute T-cell leukaemia (ATLL).
Who gets leukaemia cutis?
Leukaemia cutis is rare, affecting about 3% of people diagnosed with leukaemia. It occurs in males and females of any age, and with almost any kind of leukaemia. In most cases, leukaemia occurs out of the blue. However, some kinds of leukaemia are associated with abnormalities of chromosomes, such as the Philadelphia chromosome.
Proliferation of the abnormal leukocytes is due to activation of oncogenes (cancer-promoting genes) or inactivation of tumour suppressor genes. Thus leukaemia is more common in syndromes that have mutations in these genes. These syndromes may be inherited and include Bloom syndrome.
Other known risks for the development of leukaemia include:
- Exposure to benzene
- Ionizing radiation
- Alkylating agents used in chemotherapy
- Viral infection e.g., HTLV-1, Epstein-Barr virus
- Other blood diseases such as myelodysplastic syndrome
It is not known why the leukaemia cells sometimes choose to grow in the skin.
What are the clinical features of leukaemia cutis?
In most cases presenting with leukaemia cutis, the patient is already known to have leukaemia because of abnormal blood count or bone marrow findings.
The skin lesion is the very first sign of the haematological malignancy in 7% of patients with leukaemia cutis. This is sometimes called aleukaemic leukaemia. Bone marrow infiltration and systemic symptoms occur later.
Sometimes myeloid leukaemia relapses in the skin after apparently successful treatment of bone marrow. It is then called ‘extramedullary’ leukaemia.
Skin changes
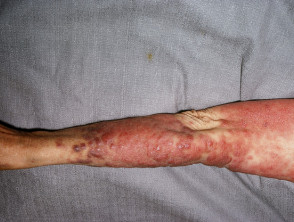
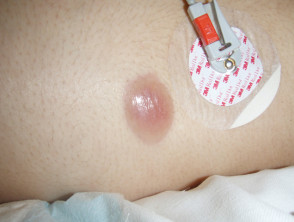
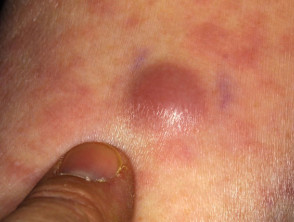
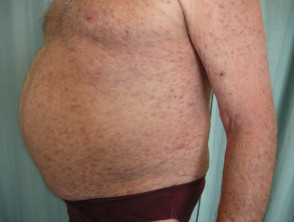
Leukaemia cutis can present with various types of skin lesion. They are usually asymptomatic; that is, they are not itchy or sore.
- Firm papules (small bumps), nodules (larger lumps), and plaques (thickened flat patches), which may be skin-coloured, red, brown or purple
- Diffuse eczema-like red dry thickened skin (erythroderma)
- Figurate or annular erythema
- Purpura and petechiae (purple patches and spots due to bleeding into the skin)
- Blisters, erosions and ulcers
- Swollen gums (gingival hyperplasia or gingivitis) in acute leukaemia.
- The skin lesions most often arise on the head, neck and trunk.
- They favour sites of injury.
- In babies, leukaemia cutis is one of the causes of blueberry muffin syndrome.
Chloroma
‘Chloromas’ sometimes arise in myeloid leukaemia or granulocytic sarcoma. These may present as solitary or numerous nodules. They appear blue-green when cut into at the time of biopsy, hence the name. The colour is due to myeloperoxidase granules in the malignant leukocytes. This type of leukaemia cutis may precede the development of systemic leukaemia by several months.
Leukaemia cutis
Blood abnormalities
Pancytopaenia occurs; that is, a reduction in red cells, white cells and platelets — all normally formed in the bone marrow.
- Anaemia: pallor, tiredness, breathlessness.
- Reduced neutrophil count: bacterial, viral, fungal infections often with unusual or opportunistic organisms.
- Reduced platelet count (thrombocytopenia): easy bruising, bleeding.
Other organs
Symptoms depend on which organs have been infiltrated by the leukaemic cells.
- Fever, chills, lethargy
- Enlarged liver and spleen: nausea, abdominal fullness, constipation.
- Swollen lymph glands.
- Central nervous system: cranial nerve palsies, stroke, seizures, headache, loss of sensation.
- Musculoskeletal system: painful or swollen bones and joints, fractures, gout.
How is the diagnosis made?
Leukaemia is suspected from an abnormal blood count and confirmed by sampling the bone marrow by aspiration or trephine.
Although leukaaemia cutis may be suspected from the patient's history and the appearance of the skin, skin biopsy is necessary to confirm the diagnosis. This reveals a diffuse infiltration of malignant leukocytes in the dermis.
- The cells can cluster around blood vessels and sweat glands.
- They may spread as single cells through the collagen bundles.
- Immature or precursor myeloid cells in AML often have cytoplasmic granules.
- Immature lymphoid cells in ALL are large and do not have granules.
- Promyelocytes, metamyelocytes, bands and mature neutrophils are typical in CML.
- Dense uniform-looking small round lymphocytes are seen in CLL.
- Kidney-shaped cells are seen in monocytic leukaemia.
- Flower cells are seen in ATLL.
- There may be considerable bleeding, especially in AML.
Further histochemistry (immunostaining and immunotyping) may reveal the specific cell type involved. It is sometimes very difficult to diagnose leukaemia cutis.
- ALL and CLL may be confused with lymphoma.
- AML and CML may be confused with extramedullary haematopoeisis.
- Similar features may be seen in vasculitis, drug eruptions and infectious emboli.
- If the cells are uniform, the lymphocytic or neutrophilic infiltrate may appear reactive rather than malignant.
Blood tests may include:
- Complete blood count
- Peripheral blood smear
- Cytogenetic studies
- Coagulation tests
- Liver and kidney function tests
- Lactate dehydrogenase
- Uric acid levels
- Calcium, magnesium, sodium, potassium levels
- Blood culture in case of fever.
It is likely that imaging will be done to find out the extent of organ involvement and may include chest X-ray, abdominal ultrasound, CT scan, and MRI scan.
What is the treatment?
Treatment is directed towards the underlying leukaemia, so the patient should be under the care of an experienced clinical haematologist and/or medical oncologist. Systemic chemotherapy is the usual choice depending on the overall condition of the patient.
Other treatments include electron beam therapy, localised radiation, and phototherapy.
Fever usually indicates infection and requires investigation and treatment with systemic antibiotics, antifungal and antiviral treatment.
The prognosis is poor.
Other skin disorders associated with leukaemia
Patients with leukaemia are prone to a variety of skin conditions.
- Neutrophilic dermatoses: Sweet disease, pyoderma gangrenosum, neutrophilic eccrine hidradenitis
- Vasculitis: polyarteritis nodosa, erythema elevatum diutinum
- Panniculitis: erythema nodosum, lobular panniculitis
- Urticaria
- Nonspecific dermatitis
- Eosinophilic dermatosis of haematological malignancy
- Erythema multiforme
- Paraneoplastic pemphigus
- Infections due to immune suppression: cellulitis, thrush, herpes zoster, herpes simplex and opportunistic infections with unusual organisms such as systemic mycoses
- Skin cancer, due to immunosupression from disease or its treatment
- Drug eruptions
- Graft versus host disease after bone marrow transplantation