Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand. 2009/2015. Updated: Dr Amy Stanway, Dermatologist, Tauranga, New Zealand. Copy edited by Gus Mitchell. July 2021
Normal skin changes in pregnancy Skin conditions specific to pregnancy Skin conditions that worsen during pregnancy Skin condition that improve during pregnancy Skin conditions associated with complications of pregnancy Outcome
During pregnancy there are marked changes in sex hormones, the immune system, and the cardiovascular system, and this can lead to changes in the skin. Many changes in the skin, hair, and nails of pregnant women are common and considered normal (physiological).

Linea nigra
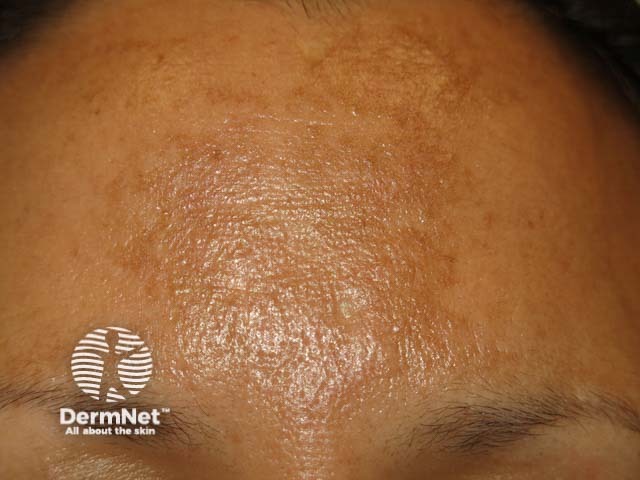
Melasma
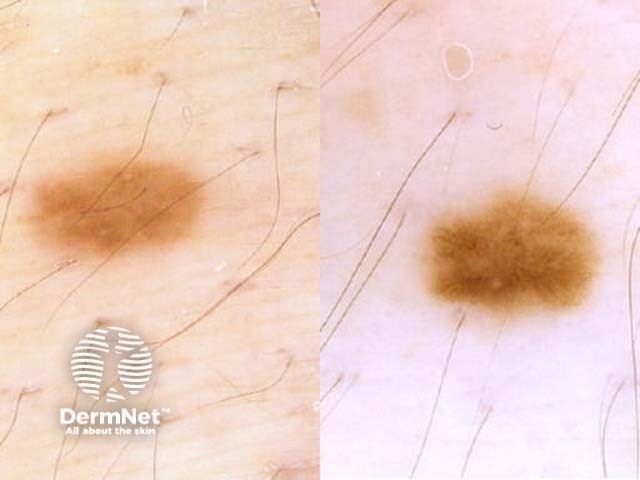
Dermoscopic change in a melanocytic naevus in pregnancy
Stretch marks (striae) are extremely common in pregnancy, affecting up to 90% of women in the second and third trimesters. They are linear, pink or purple, atrophic bands that develop at right angles to the skin tension lines on the abdomen, breasts, thighs, and buttocks.
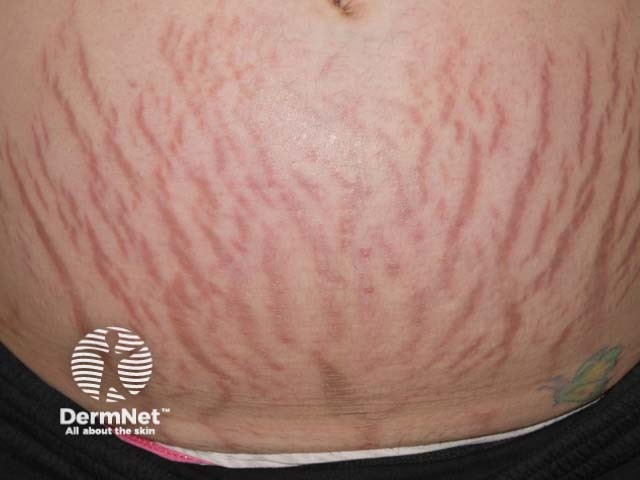
Striae gravidarum

Shed hair due to telogen effluvium
Nail changes commonly occur during pregnancy. Increased brittleness, leukonychia, onychoschizia, and ingrown toenails are most common. Increased nail growth, onycholysis, melanonychia, grooving of nails, and subungual hyperkeratosis are also described. [see Nail terminology]. Benign, uniform, symmetrical hyperpigmentation of multiple nails is reported during pregnancy with fading postpartum; however, irregular pigmentation with cuticle involvement should prompt investigation of possible melanoma.
The vascular changes of pregnancy are probably brought about by the general increase in vascularity associated with high oestrogen levels and increased blood volume.
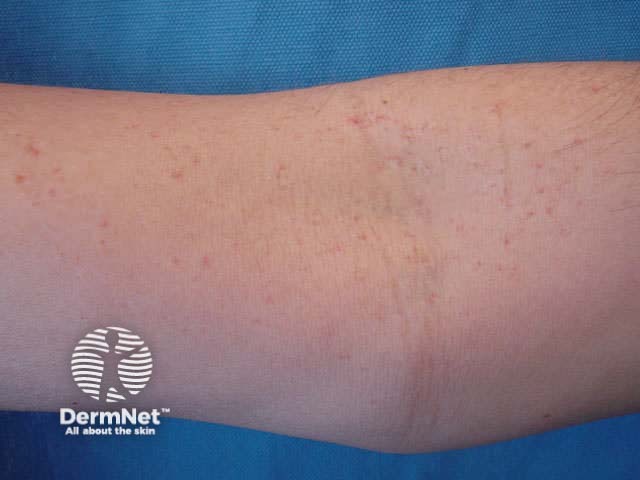
Spider telangiectases

Palmar erythema
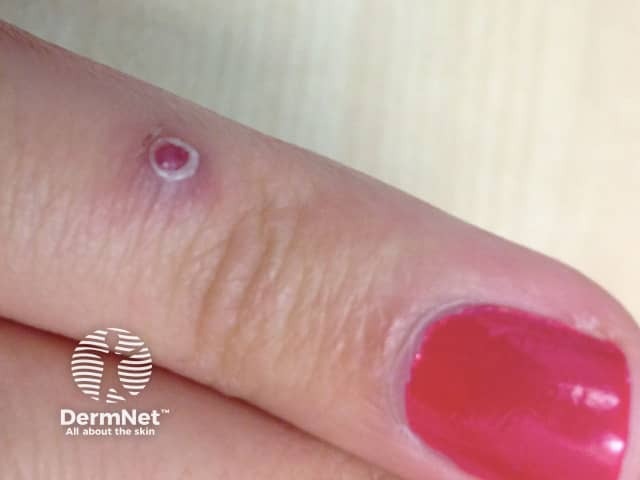
Pyogenic granuloma
A switch from cell-mediated to humoral immunity (TH1 to TH2 shift) during pregnancy is important to make sure the mother’s body does not reject the developing fetus. This influences a woman’s susceptibility to skin disease, increasing the tendency towards autoimmune disease and reducing her cell-mediated immunity.
Diseases that are TH1-driven, such as psoriasis, tend to improve while TH2-driven diseases, such as atopic dermatitis and systemic lupus erythematosus, are exacerbated. Reduced cell-mediated immunity during normal pregnancy probably accounts for the increased frequency of and severity of certain infections such as candida, herpes simplex, and varicella/zoster.
There are four main conditions that occur specifically during pregnancy. These are called pregnancy-specific dermatoses.
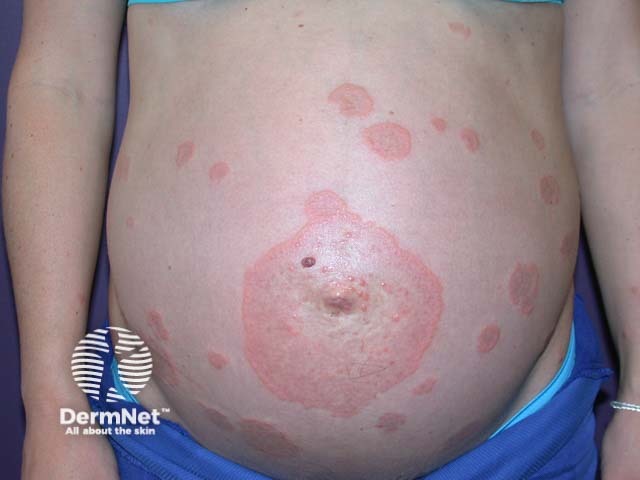
Pemphigoid gestationis
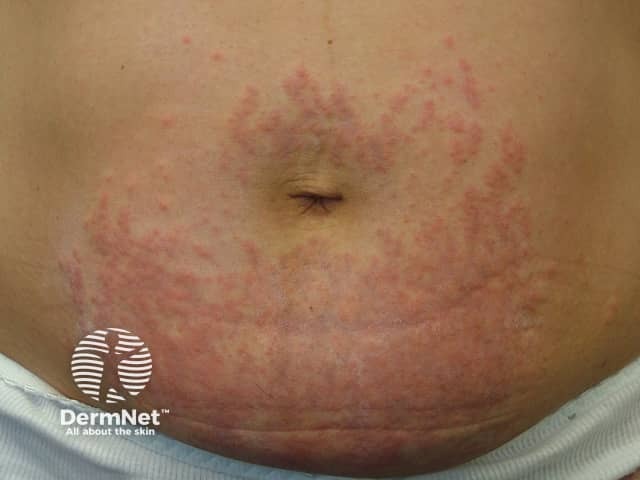
Polymorphic eruption of pregnancy

Prurigo of pregnancy
Other conditions have a variant specific to pregnancy:

Acne in pregnancy
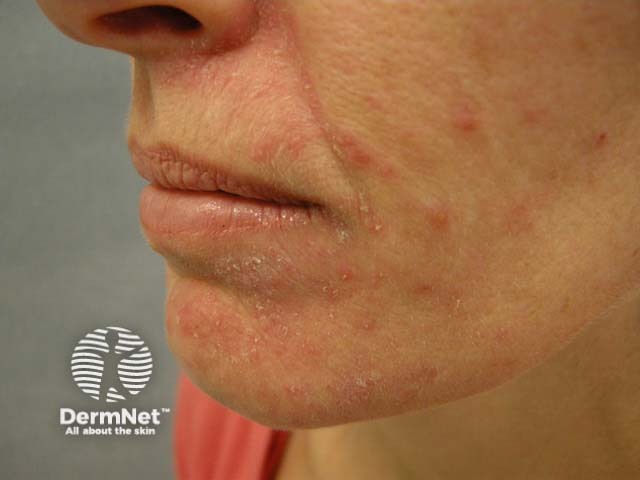
Perioral dermatitis

Pyoderma faciale
Most pregnancy-associated physiological changes in the skin improve after delivery but may not completely clear. Hair, nail, vascular, immune, and glandular changes usually resolve in the months following delivery.
Pre-existing skin conditions that worsen or improve during pregnancy usually return to the pre-pregnancy state post-partum.
Skin conditions that are associated with complications during pregnancy can cause temporary or permanent complications for the mother, fetus, or neonate. These conditions need to be diagnosed early and managed to minimise the risk or treat the complications as they arise. When possible, mothers with pre-existing conditions should plan their pregnancy in consultation with their doctor to ensure the best outcome for mother and baby.