Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Melasma — extra information
Melasma
Authors: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. 1997/2014. Updated: Dr Brent J Doolan, Dermatology Research Fellow, The Skin Hospital, Sydney NSW, Australia. Dr Monisha Gupta, Dermatologist, The Skin Hospital, Sydney NSW, Australia. Copy edited by Gus Mitchell. October 2020.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
What is melasma?
Melasma is a common acquired skin disorder that presents as a bilateral, blotchy, brownish facial pigmentation.
This form of facial pigmentation was previously called chloasma, but as this derives from the Greek meaning ‘to become green’, the term melasma (brown skin) is preferred. It was also known as the ‘mask of pregnancy’.
Who gets melasma?
Melasma is more common in women than in men, with an onset typically between the ages of 20 and 40 years. Melasma is most common in people who tan easily or have naturally brown skin (Fitzpatrick skin phototypes III, IV). It is less common in people with fair skin (Fitzpatrick types I, II) or black skin (Fitzpatrick types V, VI).
What causes melasma?
The cause of melasma is complex; it has been proposed to be a photoageing disorder in genetically predisposed individuals. The pigmentation ultimately results from the overproduction of melanin by melanocytes (pigment cells); either taken up by keratinocytes (epidermal melanosis) and/or deposited in the dermis (dermal melanosis, melanophages).
Factors implicated in the development of melasma include:
- Family history — 60% report affected family members
- Sun exposure — ultraviolet and visible light promote melanin production
- Hormones — pregnancy and the use of oestrogen/progesterone-containing oral contraceptives, intrauterine devices, implants, and hormone replacement therapy, are implicated in one-quarter of affected women; thyroid disorders can be associated with melasma
- Medications and scented products — new targeted therapies for cancer and perfumed soaps, toiletries, and cosmetics may cause a phototoxic reaction to trigger melasma
- Researchers are examining the roles of stem cell, neural, vascular, and local hormonal factors in promoting melanocyte activation.
What are the clinical features of melasma?
Melasma presents as bilateral, asymptomatic, light-to-dark brown macules or patches with irregular borders.
Distinct patterns include:
- Centrofacial — forehead, cheeks, nose, upper lip (sparing the philtrum); 50-80% of presentations
- Malar — cheeks, nose
- Mandibular — jawline, chin
- Erythosis pigmentosa faciei — reddened or inflamed
- Extrafacial — forearms, upper arms, shoulders in a sun-exposed distribution.
Melasma can be separated into epidermal, dermal, and mixed types, depending on the level of increased melanin in the skin.
Epidermal melasma
Epidermal melasma is defined by:
- Border: well-defined
- Colour: dark brown
- Wood lamp: appears more obvious
- Dermoscopy: Scattered islands of brown reticular network with dark fine granules
- Treatment: usually has a good response.
Dermal melasma
Dermal melasma is defined by:
- Border: ill-defined
- Colour: Light brown to blue-grey
- Wood lamp: no accentuation
- Dermoscopy: reticuloglobular pattern, telangiectasia, arciform structures
- Treatment: usually has a poor response.
Mixed melasma
Mixed melasma is the most common type, and is defined by:
- Combination of blue-grey, light and dark brown colours
- Mixed patterns seen with Wood lamp and dermatoscope
- Treatment usually shows a partial improvement.

Melasma
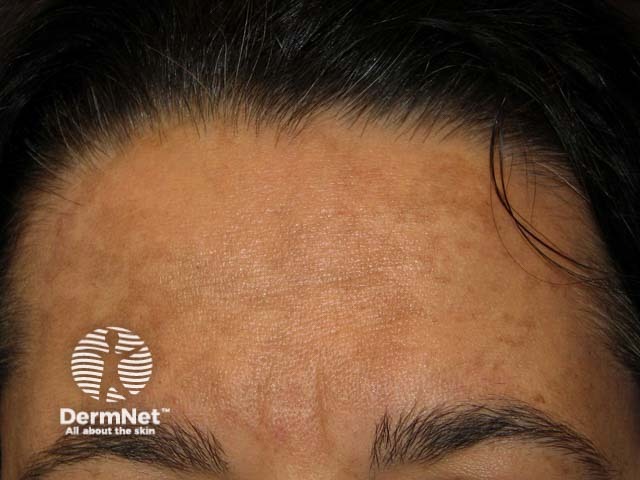
Melasma
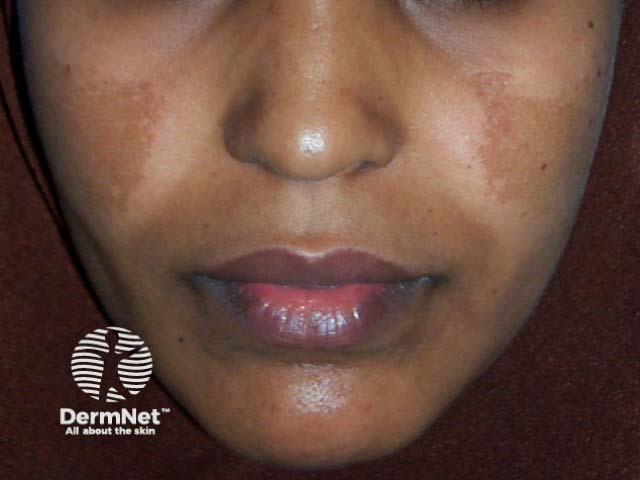
Melasma
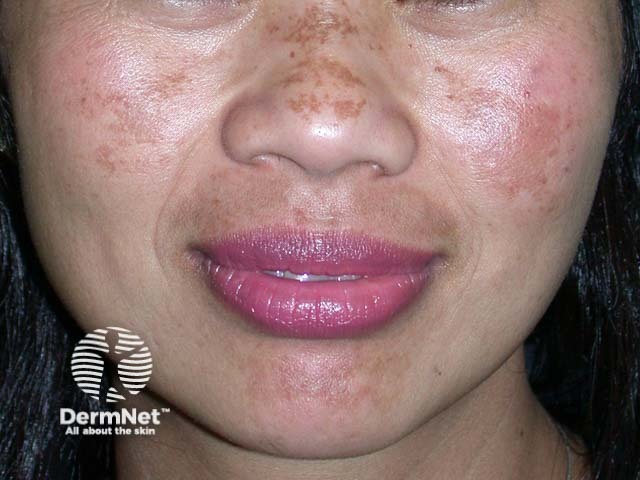
Melasma
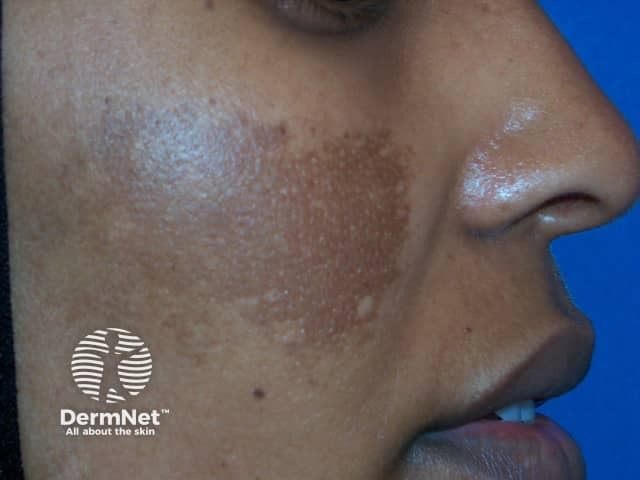
Melasma
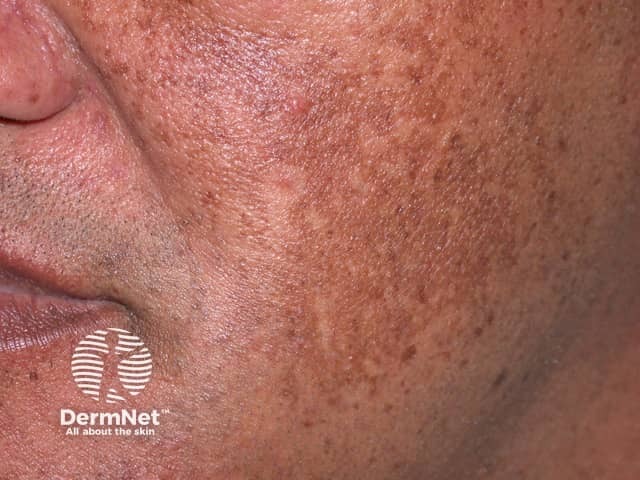
Melasma
See more melasma images.
What are the complications of melasma?
Melasma can have a severe impact on quality of life due to its visibility.
How is melasma diagnosed?
Melasma is usually a clinical diagnosis based on the clinical appearance, and examination with a Wood lamp and dermatoscope.
Occasionally a skin biopsy may be taken. Histology varies with the type of melasma, but typically the following features are seen:
- Melanin deposited in basal and suprabasal keratinocytes
- Highly dendritic (branched) intensely pigmented melanocytes
- Melanin within dermal melanophages
- Solar elastosis and elastic fibre fragmentation
- An increase in blood vessels.
Serial photography and severity indices such as the Melasma Area and Severity Index (MASI) or modified MASI can be used to monitor response to treatment.
What is the differential diagnosis for melasma?
Other disorders that may resemble melasma clinically include:
- Post-inflammatory hyperpigmentation
- Solar lentigo and other forms of lentigines and freckles
- Acquired dermal macular hyperpigmentation
- Drug-induced hyperpigmentation
- Naevus of Ota and naevus of Hori.
What is the treatment for melasma?
A combination of measures is generally required.
General measures
- Year-round, life-long sun protection — broad-brimmed hat, broad-spectrum very high protection factor (SPF50+) sunscreen containing iron oxides, and sunsmart behaviour
- Discontinue hormonal contraception if possible
- Cosmetic camouflage.
Topical therapy
The most successful formulation has been a combination of hydroquinone, tretinoin, and moderate potency topical steroid (skin lightening cream) reported to clear or improve 60–80%.
Other topical agents used alone or, more commonly, in combination have included:
- Thiamidol
- Azelaic acid
- Kojic acid
- Cysteamine cream
- Ascorbic acid
- Methimazole
- Tranexamic acid
- Glutathione
- Soybean extract.
Many other agents are under investigation.
Oral treatment
Tranexamic acid blocks conversion of plasminogen to plasmin, with downstream effects inhibiting synthesis of prostaglandin and other factors involved in melasma.
More new oral treatments are being trialled.
Procedural techniques
Chemical peels and lasers can be used with caution, but carry a risk of worsening melasma or causing post-inflammatory hyperpigmentation. Patients should be pretreated with a tyrosinase-inhibitor, such as hydroquinone.
Superficial epidermal pigment can be peeled off using alpha-hydroxy acids (AHA), such as glycolic acid, or beta-hydroxy acids (BHA), such as salicylic acid.
Microneedling, intense pulsed light (IPL), and lasers including Q-switched Nd:YAG, ablative and non-ablative fractionated and picosecond lasers carry a high risk for relapse and the disease becoming more resistant to treatment, so require expert use.
What is the outcome for melasma?
Melasma can be frustrating to treat, both for the patient and the medical practitioner. It is slow to respond to treatment, especially if it has been present for a long time.
Even in those who get a good result from treatment, pigmentation may reappear on exposure to summer sun.
The chronicity and risk for relapse with the need for lifelong sun protection should be emphasised to set realistic goals and outcomes.
Bibliography
- Bala HR, Lee S, Wong C, Pandya AG, Rodrigues M. Oral tranexamic acid for the treatment of melasma: a review. Dermatol Surg. 2018;44(6):814–25. doi:10.1097/DSS.0000000000001518. PubMed
- Boukari F, Jourdan E, Fontas E, et al. Prevention of melasma relapses with sunscreen combining protection against UV and short wavelengths of visible light: a prospective randomized comparative trial. J Am Acad Dermatol. 2015;72(1):189–90.e1. doi:10.1016/j.jaad.2014.08.023. PubMed
- Handel AC, Miot LD, Miot HA. Melasma: a clinical and epidemiological review. An Bras Dermatol. 2014;89(5):771–82. doi:10.1590/abd1806-4841.20143063. PubMed
- Kheradmand M, Afshari M, Damiani G, Abediankenari S, Moosazadeh M. Melasma and thyroid disorders: a systematic review and meta-analysis. Int J Dermatol. 2019;58(11):1231–8. doi:10.1111/ijd.14497. PubMed
- Ogbechie-Godec OA, Elbuluk N. Melasma: an up-to-date comprehensive review. Dermatol Ther (Heidelb). 2017;7(3):305–18. doi:10.1007/s13555-017-0194-1. PubMed
- Passeron T, Picardo M. Melasma, a photoaging disorder. Pigment Cell Melanoma Res. 2018;31(4):461–5. doi:10.1111/pcmr.12684. PubMed
- Rodrigues M, Pandya AG. Melasma: clinical diagnosis and management options. Australas J Dermatol. 2015;56(3):151–63. doi:10.1111/ajd.12290. PubMed
- Sarma N, Chakraborty S, Poojary SA, et al. Evidence-based review, grade of recommendation, and suggested treatment recommendations for melasma. Indian Dermatol Online J. 2017;8(6):406–42. doi:10.4103/idoj.IDOJ_187_17. PubMed
- Sonthalia S, Jha AK, Langar S. Dermoscopy of melasma. Indian Dermatol Online J. 2017;8(6):525–6. doi:10.4103/idoj.IDOJ_6_17. PubMed Central
- Trivedi MK, Yang FC, Cho BK. A review of laser and light therapy in melasma. Int J Womens Dermatol. 2017;3(1):11–20. doi:10.1016/j.ijwd.2017.01.004. PubMed Central
On DermNet
Other websites
- Melasma — Medscape Reference
- Melasma — British Association of Dermatologists
- Melasma: Tips for managing — American Academy of Dermatology
- Melasma — American Academy of Dermatology
