What is paronychia?
Paronychia is inflammation of the skin around a finger or toenail. It can be acute (< 6 weeks) or chronic (persisting > 6 weeks).
Paronychia is also called whitlow. It may be associated with felon.
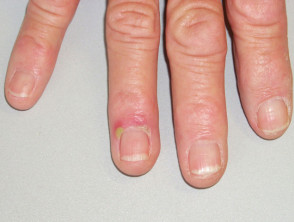
Paronychia
Who gets paronychia?
Acute paronychia can affect anyone. However, it is more likely to follow a break in the skin, especially between the proximal nail fold/cuticle and the nail plate. For example:
- If the nail is bitten (onychophagia) or the nail-fold is habitually picked (eg, habit-tic nail deformity)
- In infants that suck their fingers or thumbs
- Following manicuring
- Ingrown toenails (onychocryptosis)
- On the application of sculptured or artificial fingernails
- Treatment with oral retinoid that dries the skin (acitretin, isotretinoin)
- Other drugs, including epidermal growth factor receptor and BRAF inhibitors (vemurafenib, dabrafenib)
Chronic paronychia mainly occurs in people with hand dermatitis, or who have constantly cold and wet hands, such as:
- Dairy farmers
- Fishermen
- Bartenders
- Cleaners
- Housewives
- People with poor circulation
Acute and chronic skin infections tend to be more frequent and aggressive in patients with diabetes or chronic debility, or that are immune suppressed by drugs or disease.
What causes paronychia?
Acute paronychia is usually due to bacterial infection with Staphylococcus aureus (which may be multiresistant), Streptococcus pyogenes, Pseudomonas, or other bacterial pathogens. It can also be due to the cold sore virus, Herpes simplex (herpetic whitlow), and the yeast, Candida albicans.
The cause or causes of chronic paronychia are not fully understood. In many cases, it is due to dermatitis of the nail fold. Often several different micro-organisms can be cultured, particularly Candida albicans and the Gram-negative bacilli, pseudomonas.
What are the clinical features of paronychia?
Acute paronychia
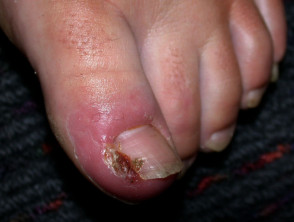
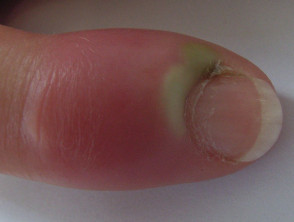
Acute paronychia develops rapidly over a few hours, and usually affects a single nail fold. Symptoms are pain, redness and swelling.
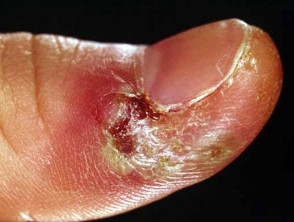
If herpes simplex is the cause (herpetic whitlow), multiple tender vesicles may be observed. Sometimes yellow pus appears under the cuticle and can evolve to abscess. The nail plate may lift up (onycholysis). Acute paronychia due to S. pyogenes may be accompanied by fever, lymphangitis and tender lymphadenopathy.
Acute candida more commonly infects the proximal nail fold.
Acute paronychia
Chronic paronychia
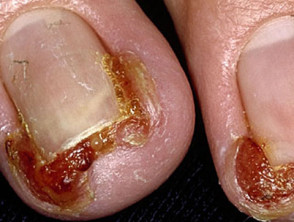
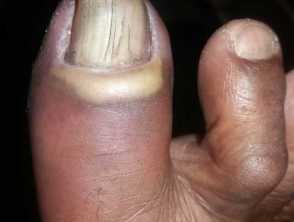
Chronic paronychia is a gradual process. It may start in one nail fold, particularly the proximal nail fold, but often spreads laterally and to several other fingers. Each affected nail fold is swollen and lifted off the nail plate. This allows the entry of organisms and irritants. The affected skin may be red and tender from time to time, and sometimes a little pus (white, yellow or green) can be expressed from under the cuticle.
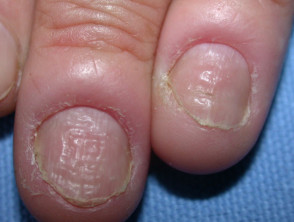
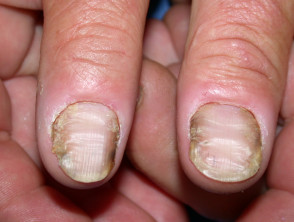
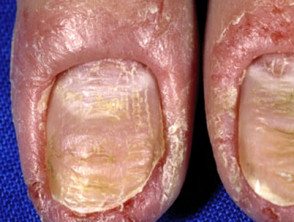
The nail plate thickens and is distorted, often with transverse ridges.
Chronic paronychia and nail changes
See more images of paronychia ...
What are the complications of paronychia?
Acute paronychia can spread to cause a serious hand infection (cellulitis) and may involve underlying tendons (infectious tendonitis).
The main complication of chronic paronychia is nail dystrophy. It is often associated with distorted, ridged nail plates. They may become yellow or green/black and brittle. After recovery, it takes up to a year for the nails to grow back to normal.
How is paronychia diagnosed?
Paronychia is a clinical diagnosis, often supported by laboratory evidence of infection.
- Gram stain microscopy may reveal bacteria
- Potassium hydroxide microscopy may reveal fungi
- Bacterial culture
- Viral swabs
- Tzanck smears
- Nail clippings for culture (mycology).
What is the treatment for paronychia?
Acute paronychia
- Soak affected digit in warm water, several times daily.
- Topical antiseptic may be prescribed for a localised, minor infection.
- Oral antibiotics may be necessary for severe or prolonged bacterial infection; often a tetracycline, such as doxycycline, is prescribed.
- Consider early treatment with aciclovir in case of severe herpes simplex infection (herpetic whitlow).
- Surgical incision and drainage may be required for abscess followed by irrigation and packing with gauze.
- Rarely, the nail must be removed to allow pus to drain.
Chronic paronychia
Attend to predisposing factors.
- Keep the hands dry and warm.
- Avoid wet work, or use totally waterproof gloves that are lined with cotton.
- Keep fingernails scrupulously clean.
- Wash after dirty work with soap and water, rinse off and dry carefully.
- Apply emollient hand cream frequently – dimethicone barrier creams may help.
Treatment should focus on dermatitis and any microbes grown on culture [1].
- Topical corticosteroid ointment is applied for 2–4 weeks and repeated for flares.
- Tacrolimus ointment is an alternative when dermatitis is not responding to routine management [2].
- Intralesional steroid injections are sometimes used in resistant cases.
- Antiseptics or antifungal lotions or solutions may be applied for several months.
- Oral antifungal agent (itraconazole or fluconazole), if C. albicans is confirmed.
Other management
- Patients with diabetes and vascular disease with toenail paronychia infections should be examined for signs of cellulitis.
- Surgical excision of the proximal nail fold may be necessary.
- Eponychial marsupialisation involves surgical removal of a narrow strip of skin next to the nail, to reduce the risk of infection [3].
- Swiss roll technique has the advantage of retaining the nail plate and quicker recovery [4].
What is the outlook for paronychia?
Acute paronychia usually clears completely in a few days, and rarely recurs in healthy individuals.
Chronic paronychia may persist for months or longer and can recur in predisposed individuals.