What is Turner syndrome?
Turner syndrome is a common genetic condition that almost exclusively presents in females. Infertility, failure to develop secondary sexual characteristics in adolescence and short stature develop in the majority of patients. Lymphoedema causes many of the other features. There are a number of skin conditions commonly seen in patients with Turner syndrome.
The approved gene symbol for Turner syndrome is TNR1.
Turner syndrome
Who gets Turner syndrome and why?
Turner syndrome affects approximately 1 in 2500 live female births and is a common cause of miscarriage (up to 10%). It affects 3% of females conceived but only 1% survive to birth.
Turner syndrome develops when there is only one entire functional X chromosome. In approximately 50% of patients there is a single X chromosome ie 45,X. The other 50% may have one of a number of structural defects in the second sex chromosome. The commonest structural abnormality is called isochromosome Xq. Up to 10% have a marker (ring) X chromosome. There are some correlations between the genetic defect and the clinical presentation. 45,X is associated with the most severe clinical presentation.
Mosaicism occurs when the second sex chromosome is lost or damaged after the embryo has started to develop. This results in two different cell populations in the body, some of which are normal and the others showing the Turner karyotype. Mosaicism, particularly 45,X/46,XX, is generally associated with a better prognosis than 45,X. Usually the second sex chromosome is an X, but rarely in some mosaics there is a normal or abnormal Y chromosome in some cells, ie 46,XY, but others are 45,X.
The X chromosome from the mother is found in the majority of girls with Turner syndrome. Whereas the X chromosome from the father is more commonly associated with spontaneous miscarriages.
Turner syndrome is not associated with advanced parental age.
Clinical features of Turner syndrome
The classic clinical triad of Turner syndrome is infertility (95%), failure to progress through puberty and short height (98%). Although growth may initially be normal, short stature tends to appear early and results in an average adult height of 143-147cm, approximately 20cm less than the general population.
Patients with Turner syndrome often have a typical facial appearance due to bone abnormalities. The eyes are sloped with the outer corners lower than the inner and a skin fold at the inner corners of the eyes. There may be other eye problems, most commonly squint (strabismus) and droopy eyelids (ptosis). The lower jaw is small (micrognathia). The ears are lowset on the head and may be an unusual shape.
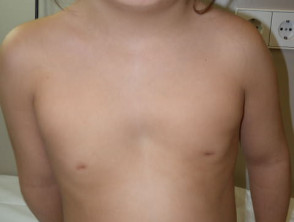
A short neck can be due to scoliosis or small vertebrae. The chest is usually square in shape like a shield with widely spaced nipples and minimal or absent breast development after puberty.
Many organ systems are involved in Turner syndrome including the reproductive system (womb, ovaries), cardiovascular system (heart and major blood vessels), gastrointestinal system (bowel), kidneys and bones.
Dermatological features
Lymphoedema is the accumulation of lymph in the tissues and is present in 80% of babies born with Turner syndrome. Swelling of hands, feet and/or neck in infancy is due to lymphoedema. The lymphoedema usually disappears by 2 years of age but may recur later affecting one or both legs in late childhood or adulthood.
Neck webbing (pterygium coli) follows resolution of a cystic hygroma which commonly forms on the back of neck during fetal development but resolves before birth. It is present in up to 50%.
The characteristic nail changes seen in up to 70% of infants and young children with Turner syndrome are probably due to lymphoedema. Fingernails are often small. Nails show over-curvature, either concave (bowl-shaped) with the free edge turned up or deep set and overcurved side to side (convex overcurvature). Toenails tend to be more affected than fingernails. This can result in paronychia or pain when wearing shoes. Nail pitting may also occur. The nail changes tend to improve with age.
Multiple melanocytic naevi (moles) appear in up to 70% in late childhood mainly over the face, back and limbs. The average number of moles is much higher in Turner syndrome than the general population, particularly in fair skin. The moles are usually small (1-5mm) and typical in appearance. Sun exposure does not appear to be a trigger for this but the number of moles increases with age. Despite the large number of moles, there does not appear to be an increased risk of melanoma.
Halo naevi, moles surrounded by a white rim, are more commonly seen in patients with Turner syndrome than the general population.
Although keloid and hypertrophic scarring is commonly reported in Turner syndrome, it usually occurs following surgery at sites that are known to be at increased risk of becoming keloid such as the chest (heart surgery) and back of neck (surgical correction of the neck webbing). Therefore the true relevance of such scarring in Turner syndrome has not yet been determined.
The posterior hairline is low in up to 80%. Armpit and pubic hair is often reduced. Hirsutism can occur and increased hair on limbs has been reported.
A high arched palate, which is often also narrow, and the small lower jaw contribute to overcrowding of teeth. The teeth are often small.
Vitiligo and alopecia areata may be more common in Turner syndrome. Studies have suggested alopecia areata is three times more common in Turner syndrome than in the general population. There is an increased incidence of other autoimmune conditions, particularly antithyroid autoantibodies (50-60%) and hypothyroidism (20-30%), insulin resistance and type 2 diabetes mellitus (5%), coeliac disease and inflammatory bowel disease. Skin changes may complicate these conditions or be the presenting sign.
Psoriasis may be twice as common in patients with Turner syndrome than in the general population, often developing at a very early age.
On the fingers and toes, the increased surface area produced by this swelling may be the cause of unusual dermatoglyphics (fingerprint patterns) with increased numbers of large finger ridges found in 40%.
Neonatal cutis verticis gyrata has been reported, always in association with lymphoedema, however may be due to a connective tissue naevus or mucinous naevus.
Patients with Turner syndrome develop little or no acne.
How is Turner syndrome diagnosed and investigated?
The diagnosis of Turner syndrome may be delayed as the clinical features can be subtle before puberty. The diagnosis is made in adulthood in approximately 10% of affected women during an investigation for infertility or failure to have periods (amenorrhoea).
The definitive diagnosis of Turner syndrome is made on karyotyping (examination of the chromosomes under the microscope), either during pregnancy by chorionic villus sampling or amniocentesis, or when the diagnosis is considered clinically at some time after birth. Karyotyping is performed on peripheral lymphocytes (white blood cells). If normal, mosaicism may be diagnosed after examining other cells such as skin fibroblasts.
Ultrasound during pregnancy may detect cystic hygroma, coarctation of the aorta, abnormalities of the kidneys or other findings, suggesting the need for investigation for Turner syndrome.
A protocol for investigations and follow up has been suggested by Elsheikh et al (2002):
Baseline:
- Karyotype
- Ultrasound of kidneys and pelvis (for womb and ovaries)
- Echocardiogram (ultrasound of the heart)
- Thyroid autoantibodies
- Sex hormone levels
Annual:
- Physical examination
- Thyroid function
- Cholesterol/triglycerides (fasting)
- Blood sugar (fasting)
- Kidney function
- Liver function
Every 3-5 years:
- Echocardiogram
- Bone density
- Hearing test
Treatment of Turner syndrome
Turner syndrome is best managed in a multi-disciplinary dedicated clinic throughout life.
Treatment of each clinical problem should be managed as appropriate.
Life expectancy is reduced in adults mainly due to cardiovascular disease.