Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Erythema multiforme (EM) is conventionally separated into EM minor and EM major. It is now separated from Stevens Johnson syndrome (SJS) and toxic epidermal necrolysis (T.E.N.).
EM is more common in men than women and 50% are under 20 years of age. It is an eruption of classic target lesions on the extremities associated with mild fever and malaise. It persists for one to three weeks.
EM minor is mostly preceded by infection. Common causes are:
Drugs are an uncommon cause. Recurrent EM is nearly always due to recurrent herpes simplex.
Erythema multiforme minor Erythema multiforme minor Erythema multiforme minor 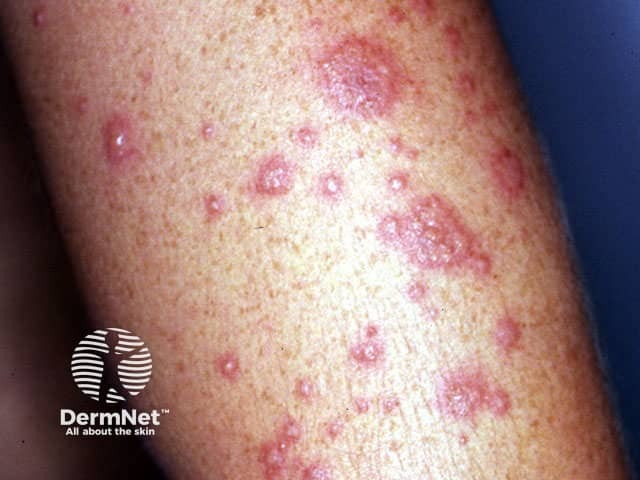
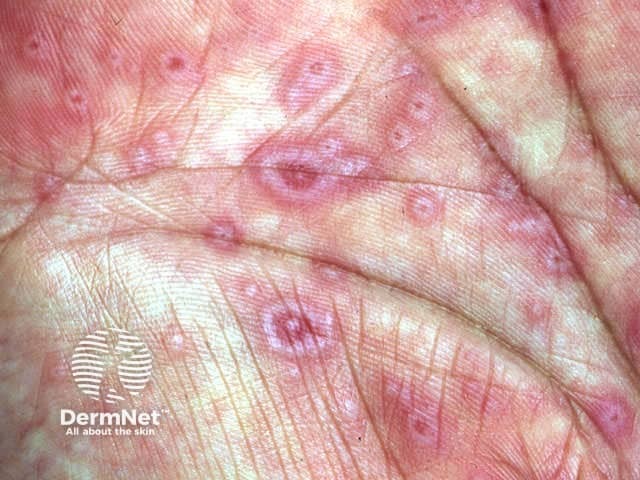
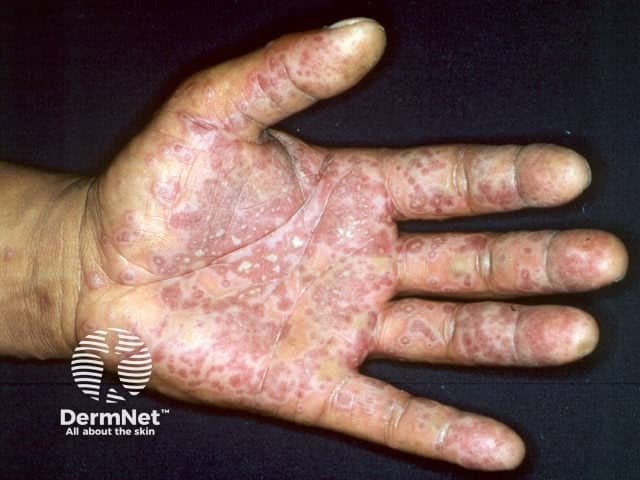
EM major is rare, except in patients suffering from human immunodeficiency virus infection. It is predominantly a mucosal eruption of erosions and blisters in the oropharynx, on the lips, conjunctivae and genitalia accompanied by fever and prostration. Target lesions or acral bullae may also be present.
Like toxic epidermal necrolysis, EM major is usually a drug eruption.
The most common drugs causing EM major:
| The most common drugs causing EM major |
|---|
|
Infections are less common causes, but EM major may occur in epidemics associated with Mycoplasma pneumoniae. There is usually lymphopaenia.
Erythema multiforme major Erythema multiforme major 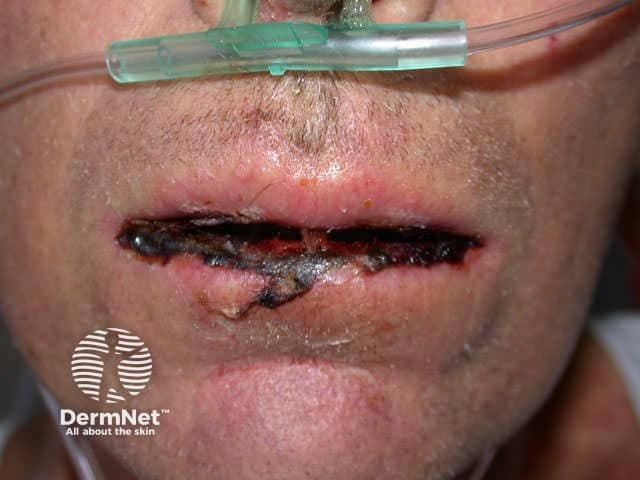
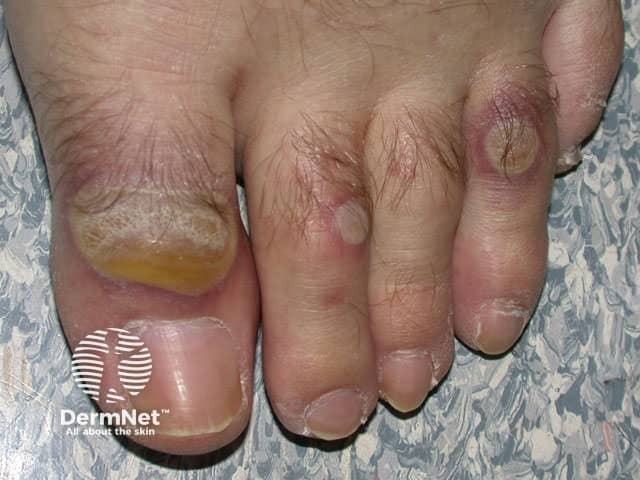

Look for underlying causes and complications of the disease.
Skin biopsy findings are often diagnostic:
EM minor resolves in 10 days or so. Symptomatic treatment may include:
Recurrent EM minor can be minimised or prevented by prophylactic oral acyclovir.
Most cases of EM major require hospitalisation for supportive care. This may include:
Oral corticosteroids should be avoided. In severe cases, EM major should be managed in an Intensive Care facility as for toxic epidermal necrolysis.
What other skin diseases may cause target lesions?
Information for patients
See the DermNet bookstore