DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Phototherapy Indications for phototherapy CME
Phototherapy
Indications for phototherapy
Created 2007.
Learning objectives
- List common skin diseases that may be treated with phototherapy and photodynamic therapy
- Describe patient factors that impact on phototherapy
Specific skin diseases
In general, the same skin diseases may be treated with phototherapy using UVB or photochemotherapy (PUVA). The most common conditions treated include:
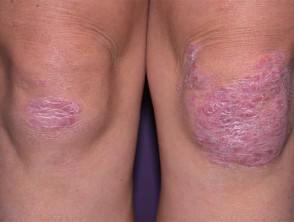
- Psoriasis
- Atopic dermatitis
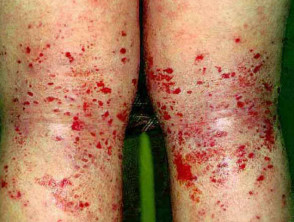
- Other forms of dermatitis
- Vitiligo
Skin diseases suitable for phototherapy
Other less common indications include:
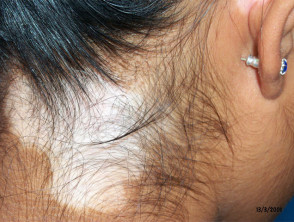
- Alopecia areata
- Pityriasis rosea
- Parapsoriasis
- Cutaneous T-cell lymphoma (CTCL)
- Polymorphous light eruption and other photodermatoses
- Lichen planus
- Generalised pruritus
- Pityriasis lichenoides
Many other skin diseases may also respond to treatment.
Photodynamic therapy (PDT) has recently been introduced to New Zealand. The main indications are actinic keratoses, in-situ squamous cell carcinoma and superficial basal cell carcinoma. PDT may prove useful for other skin diseases as experience is gained.
UVA1 phototherapy is not available in New Zealand. It is mainly used for atopic dermatitis, systemic sclerosis, morphoea, urticaria pigmentosa, disseminated granuloma annulare, lichen sclerosus, CTCL and graft-versus-host disease.
Extracorporeal photopheresis is not available in New Zealand. It is mainly used for erythrodermic CTCL (Sézary syndrome) and chronic graft-versus-host disease but has also been successfully applied to autoimmune diseases such as systemic sclerosis, pemphigus and connective tissue disease.
Assessment prior to UVB and PUVA
The initial assessment of the patient should include evaluation of:
- Age, sex, social and economic factors
- The skin disease
- Current and prior treatment
- Current medical problems
- Medications
Age
UVB phototherapy is contraindicated in infants but may be recommended for severe disease in children. PUVA is contraindicated in young children and rarely recommended prior to adulthood because it is known to cause skin cancer.
Either form of phototherapy may be impractical in the very elderly.
Sex
Females of childbearing age should be assessed for the risk of pregnancy and need for contraception. UVB phototherapy is permitted in pregnancy. PUVA is relatively contraindicated in pregnancy and absolutely contraindicated in breastfeeding.
Social and economic factors
The patient must be in a position to attend regularly for the full course of treatment, which may require three scheduled visits each week in working hours for many weeks or months. Intelligence, distance from the treatment centre, occupation and cost of treatment may be barriers.
Assess the individual's perception of the disease and its psychosocial effect.
Skin disease
Phototherapy has risks and side effects and may be inconvenient and expensive. The severity of disease or disability arising from it must warrant the treatment.
Severity may relate to:
- Extent of the skin disorder
- Involvement of specific sites such as face, hands and feet
- Symptoms such as itch or soreness
- Psychosocial impact
The disease should be located on exposed and relatively hairless skin.
A history of photo-aggravated skin disease or another adverse reaction to sunlight or previous phototherapy should be considered carefully, and may or may not be a contraindication to cautious treatment.
Other possible topical or systemic treatments may be selected instead of or as well as phototherapy.
Current and prior treatment of skin disease
Consider whether the current or prior treatment increases the risk of phototherapy.
- Prolonged &/or frequent courses of UVB or PUVA. More than 120-200 treatments with PUVA are a relative contraindication to further treatment.
- Immunosuppressive agents. Azathioprine and ciclosporin in particular markedly increase the risk of photocarcinogenesis and are contraindications to phototherapy.
- Photosensitising oral medications eg acitretin, which is frequently combined with phototherapy and necessitates lower initial doses.
- Photosensitising topical medications eg tar, which can be used but must be removed prior to exposure and lower initial doses should be selected.
Current medical problems
A careful history should include assessment of the following conditions:
- Cardiovascular disease: the patient may need to stand unassisted in a hot environment for 10 minutes or longer. Consider whether this is practical or hazardous to the patient.
- Active or latent lupus erythematosus is a contraindication to phototherapy or PUVA.
- Severe renal or hepatic disease may be a contraindication to PUVA.
- Pregnancy: consider the effect of treatment on the fetus. Avoid PUVA where possible.
- Sun damage: prior skin cancers are a relative contraindication to phototherapy. It should be used only in exceptional circumstances if a patient has a history of multiple skin cancers or melanoma. Facial skin should be protected from exposure. Additional acitretin may reduce the risk.
- Eye disease: very careful eye protection is mandatory for all patients. Contact their ophthalmologist if a patient has significant eye disease (cataracts, keratitis etc).
Topical and oral photosensitisers
Prescribed and over-the-counter cosmetics, topical and systemic medications may be photosensitising, i.e. a relatively low dose of ultraviolet radiation may provoke erythema, an eczematous dermatitis or other rash. In most cases, phototherapy is still possible, but if a photosensitising medication has been identified, it should be avoided or lower initial doses should be used.
Topical photosensitising agents include:
- Coal tar and its derivatives
- Plants (especially umbelliferae) and derivatives such as essential oils and fragrances
- Sunscreens (rarely)
The most common oral photosensitising medications include:
- Thiazide diuretics
- Antibiotics especially tetracyclines, quinolones and sulphonamides
- Non-steroidal anti-inflammatory drugs
- Phenothiazines
- Retinoids
- Griseofulvin
- Sulphonylureas
- Quinine
- Nalidixic acid
- St John's Wort
There are others.
Absolute contraindications
Absolute contraindications to phototherapy or photochemotherapy are:
- Xeroderma pigmentosum
- Lupus erythematosus
- Breastfeeding (photochemotherapy only)
Activity
Create a proforma for patient assessment prior to phototherapy.
Take the Indications for phototherapy quiz
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Photosensitizing Medication List – Radiation Protection Services, Oregon.gov
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.