DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Principles of dermatological practice Structure of the dermis and subcutis CME
Principles of dermatological practice
Structure of the dermis and subcutis
Created 2008.
Learning objectives
- Name specific structural components of the basement membrane zone, dermis and subcutis
Introduction
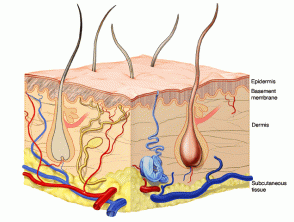
The basement membrane zone is the communication channel between epidermis and dermis. The dermis supports the epidermis, providing nutrients and protecting it.
The dermis supports the epidermis by providing it with nutrients and toughness. It is made up of fibres and ground substance, with nerves, blood vessels and cellular infiltrations. The papillary dermis is the upper portion beneath the epidermis, characterised by thin haphazardly arranged collagen fibres, thin elastic fibres and ground substance. The lower portion is the reticular dermis, composed of coarse elastic fibres and thick collagen bundles parallel to the skin surface.
The dermis is full of double rows of peg-like formations called papillae under the basement membrane zone. Each double row underlies an epidermal ridge.
The papillary dermis is the portion of the dermis just below the epidermis. The reticular dermis extends from the papillary dermis to the fat.
Below this is subcutaneous tissue, the shock absorbing, and insulating and energy storage layer.
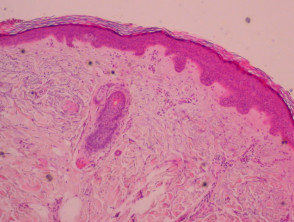
Normal skin
Basement membrane zone
| Structure | Description |
|---|---|
| Basal cell membrane |
|
| Lamina lucida |
|
| Lamina densa |
|
| Sublamina densa |
|
Dermis
| Structure | Description |
|---|---|
| Collagen |
|
| Elastic fibres |
|
| Ground substance |
|
| Fibroblasts |
|
| Blood vessels |
|
| Lymphatics |
|
| Nerves |
|
| Arrector pili muscles |
|
| Immune cells |
|
Subcutaneous tissue (subcutis, hypodermis)
| Structure | Description |
|---|---|
| Adipose cells |
|
Activity
List collagen subtypes, their differences, location and function.
Related information
References:
Other websites:
- Loyola University: Anatomy and Histology of Normal Skin
- Electronic Textbook of Dermatology: Anatomy of the skin
- University of British Columbia: The integumentary system
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.