DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Viral skin infections Viral warts CME
Viral skin infections
Viral warts
Created 2009.
Learning objectives
- Identify and manage viral warts.
Clinical features
Viral warts are benign proliferations of the skin and mucosa caused by infection with human papillomavirus (HPV); more than 150 subtypes of the DNA virus are known. Viral warts are particularly common in childhood (affecting about 15% of school children) but may arise at any age. They are spread by direct contact or autoinoculation with a latency of weeks to years. They are frequently painful and they cause significant embarrassment.
Characteristically they are hyperkeratotic ‘verrucous’ papules. The keratinocyte proliferation by basal cells is driven by viral replication within the granular layer of the epidermis.
Subtypes favour particular sites, but any wart can appear at any site. They include:
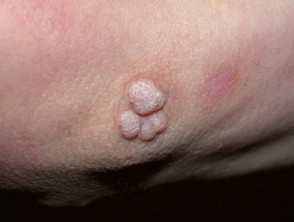
- Common warts (verruca vulgaris, HPV types 2 and 4): hard papule with dry surface most often on hands and knees.
- Butcher's warts (HPV 7): ‘cauliflower’-type, most common in meat handlers.
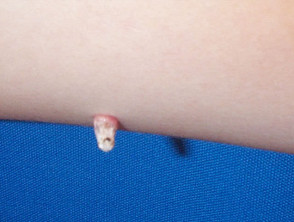
- Filiform warts: long thin lesion most often on the face
Viral warts
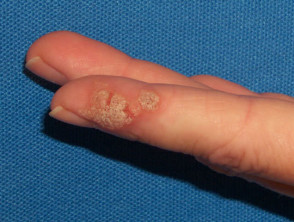
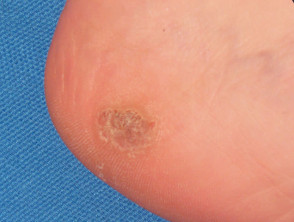
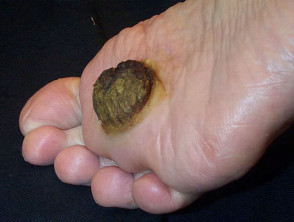
- Palmoplantar warts (myrmecia, HPV type 1): round horny deep painful nodules, most often on weight-bearing sites
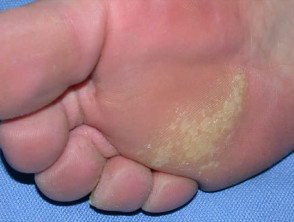
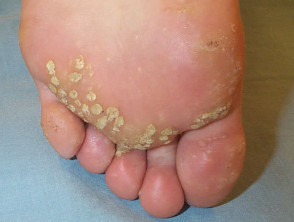
- Mosaic warts: closely grouped, generally presenting as relatively asymptomatic plantar warts
Plantar warts
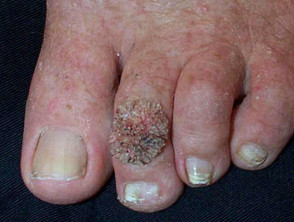
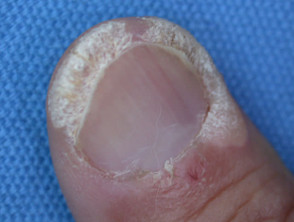
- Periungual warts: myrmecia arising around nails
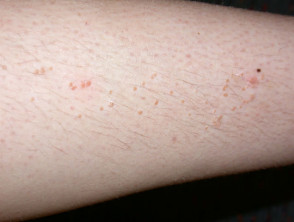
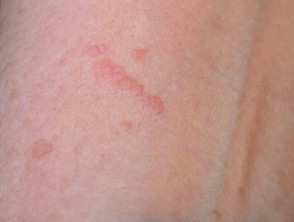
- Plane or flat warts (HPV types 3 and 10): smooth or dry small papules often numerous most often face, hands and shins. Frequently koebnerise, for example after excoriation or shaving.
Viral warts
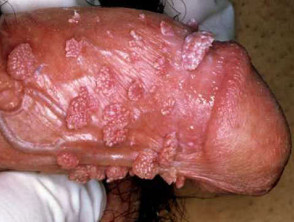
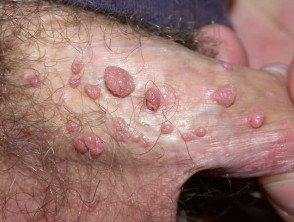
- Genital warts are often transmitted sexually. Types 6 and 8 are the most common to cause symptoms but types 16 and 18 are more likely to result in cervical, penile and vulval intraepithelial neoplasia and invasive cancer.
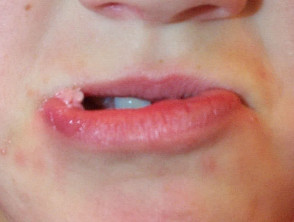
- Intraoral warts are usually misplaced genital types but those on the lips may also be common or filiform variants.
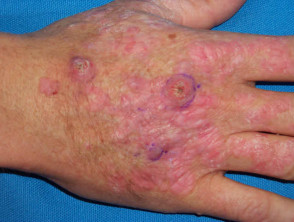
- Epidermodysplasia verruciformis (HPV types 5, 8, 20 and 47): rare genetic disorder prone to oncogenic transformation
Viral warts
Immunosuppression can result in malignant transformation of warts on non-genital sites, most commonly ten or more years after organ transplantation. Solar damage may be a cofactor.
Rarely, longstanding non-genital warts can cause verrucous carcinoma (large solitary well-differentiated squamous cell carcinoma usually found on the plantar surface).
Viral warts
Diagnosis
Warts are diagnosed clinically. It may be helpful to pare the surface to reveal small black dots, which are thrombosed capillaries. Dermoscopy can be helpful for those who have had training in its use.
Occasionally a biopsy is necessary to confirm the diagnosis. The histological features are:
- Hyperkeratosis and papillomatosis with elongated rete ridges that slope inwards
- Compact orthokeratosis
- Hypergranulosis with vacuolated cells (koilocytes)
- Dilated dermal papillary capillaries
- Columns of parakeratosis
There are variations for different clinical subtypes.
Viral typing is rarely necessary or available. It requires viral DNA amplification using polymerase chain reaction followed by Southern blot hybridisation.
Management
In children, even without treatment, 50% of warts disappear within 6 months; 90% are gone in 2 years. They are more persistent in adults but in most, they clear up eventually. Wart removal may stimulate an immune response; if not, recurrence is likely.
The most popular treatments include:
- Daily application of paints or gels containing keratolytics such as 15 to 60% salicylic acid.
- Occlusion with adhesive plaster or duct tape.
- Regular paring using a scalpel blade.
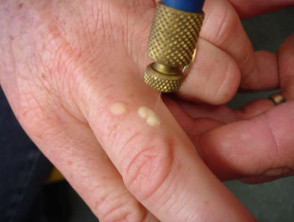
- Cryotherapy with liquid nitrogen (cotton bud or cryospray) to the wart and 1–2 mm rim of normal tissue. The depth of freeze should be sufficient to cause a little blistering and should be repeated every 2–4 weeks on 4–6 occasions. Start gently — some patients have more severe local reactions than others. Side effects include pain, injury to underlying tendons and superficial nerves (avoid the sides of digits), postinflammatory depigmentation, scarring and recurrent warts (often as a ring around the treated site).
- Electrosurgery (curettage and cautery), used for particularly large and annoying warts. Under local anaesthetic, the growth is pared away and the base burned by diathermy or cautery. The wound heals in about two weeks; even then 20% of warts can be expected to recur within a few months. However, the procedure is painful and often leaves a scar.
Wart treatment
How to use wart paint
Apply wart paint once daily. Persevere for twelve weeks or longer; up to 70% of warts will resolve with wart paints, and removing the keratinised surface relieves discomfort.
First, the skin should be softened in a bath or bowl of hot water. The hard skin should be rubbed away from the wart surface with a piece of pumice stone or emery board. The wart paint or gel should be applied accurately, allowing it to dry. It works better if covered with adhesive tape (particularly recommended when the wart is on the foot).
If the chemical makes the skin sore, stop treatment until the discomfort has settled, then recommence as above. Take care to keep the chemical off normal skin.
If simple treatments do not prove effective, there is little point in pursuing more elaborate and sometimes very expensive options as the success rates are little better. Most dermatologists in New Zealand advocate ‘benign neglect’ for extensive or longstanding warts that have failed wart paint and cryotherapy.
However, other preparations that may be applied by the patient include:
- Podophyllin (podophyllum resin), a cytotoxic agent present in a resin extracted from the May Apple plant and available as over-the-counter ointment or paint. It is a powerful irritant, contraindicated during pregnancy.
- Podophyllotoxin (refined podophyllin), applied to genital warts for 4-day courses each week for several weeks.
- Formalin 3% solution, applied to mosaic warts for 10 minutes daily. A convenient method is to pour the solution on a cotton ball and tape this to the warts. Protect interdigital spaces from irritation by first applying a barrier cream or petrolatum. Formalin is potentially toxic and it is a contact allergen.
- Imiquimod cream, most useful for genital warts. It is applied three times weekly for four to sixteen weeks.
- Tretinoin, as a cream or gel, most useful for plane warts. It is applied daily for several weeks or months.
- 5-fluorouracil cream, a cytotoxic applied for several weeks under occlusion. It may result in superficial necrosis and subsequent eradication of the wart. Specialist approval is required for PHARMAC subsidy.
Systemic retinoids (acitretin and isotretinoin) are sometimes used for extensive warts. These may require a prescription by a dermatologist and have mucocutaneous and systemic side effects.
Potential risky procedures by a health practitioner are not necessarily recommended:
- Bleomycin injected intralesionally, repeated monthly. Regulations require full staff protection. Can cause nail dystrophy if injected into periungual warts.
- Interferon alpha injected intralesionally, repeated weekly. Associated with flu-like symptoms.
- Trichloroacetic acid 80% applied weekly by the physician, resulting in immediate superficial (and sometimes deep) tissue necrosis.
- Cantharidin (extract of blister beetle), applied weekly by the physician, resulting in superficial blisters and necrosis.
- Contact allergens such as dinitrochlorobenzene (a mutagen) or dibutyl squaric acid, which cause local inflammation.
- Laser vaporisation using carbon dioxide laser, used for diffuse warts or deep plantar warts. This can be painful and leave scarring.
- Flashlamp or pulse dye laser treatments are thought to destroy the blood supply to the wart.
HPV vaccines in development have the potential to reduce the substantial morbidity and mortality associated with cervical cancer and other HPV-associated diseases. Large-scale efficacy studies that are planned or underway will provide additional information about vaccine tolerance and efficacy.
Activity
Determine the evidence that treatment of warts is effective.
Related information
On DermNet NZ
Information for patients
Other websites
- Medscape Reference:
- Cochrane review: Local treatments for cutaneous warts (use search term 'warts')
- Merck Manual Professional: Warts
Books about skin diseases
See the DermNet NZ bookstore.
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.