Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2009.
Skin generally heals rapidly to restore barrier function after injuries such as cuts, abrasions, thermal burns, puncture wounds and blisters.
The severity of a wound depends on its surface area and depth. Partial thickness wounds can recruit new keratinocytes from adjacent adnexal tissue and can regenerate much more rapidly than full thickness wounds of the same surface area where regeneration of epithelium arises only from keratinocytes on the wound edges. Damage to the dermis can be repaired but results in altered tissue i.e. a scar. However, fetal wounds heal by regeneration without fibrosis so do not result in scars.
Injury results in epidermal and dermal repair:
Haemostasis creates a protective wound scab beneath which cell migration and movement of the wound edges can occur.
Inflammation brings nutrients to the area of the wound, removes debris and bacteria, and provides chemical stimuli for wound repair.
Repair begins immediately after wounding and proceeds rapidly through the processes of epithelialisation, fibroplasia, and capillary proliferation into the healing area.
Wounds can be classified as either acute or chronic. Acute wounds are sometimes defined as those that follow the normal phases of healing; they are expected to show signs of healing in less than 4 weeks and include postoperative wounds. Chronic wounds are those that persist for longer than 4 weeks and are often of complex poorly understood origin.
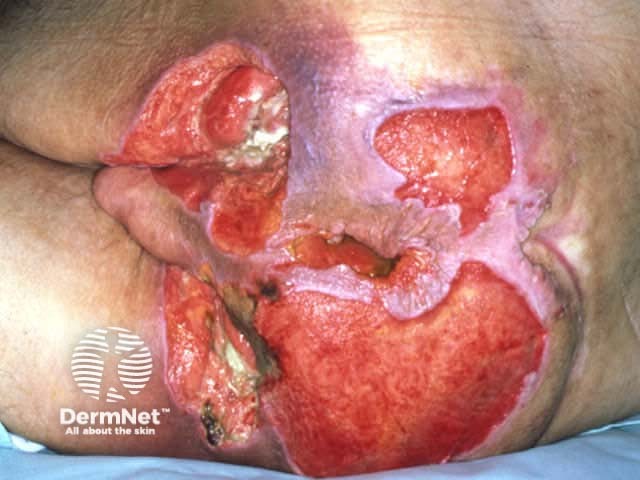
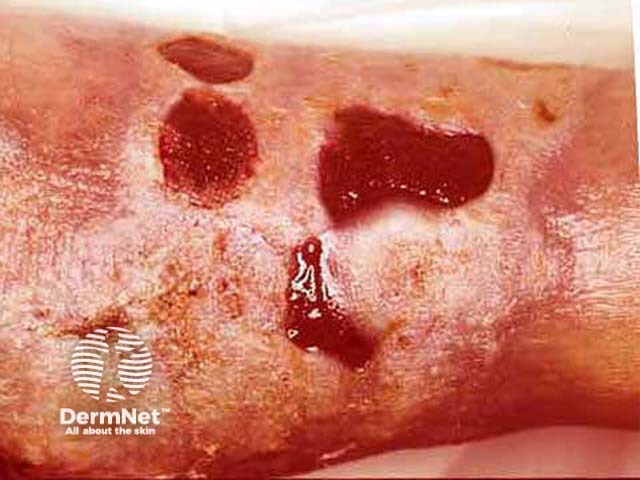
Acute surgical wound Chronic pressure ulcer Healing venous ulcer 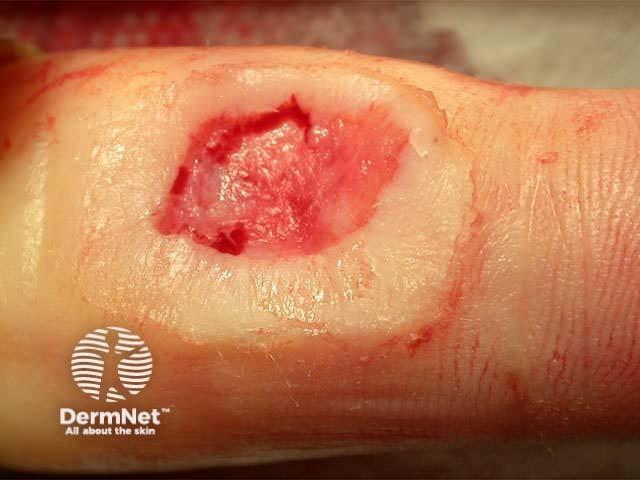
A moist environment is beneficial compared with a dry wound. Moist wounds:
Describe typical acute and chronic wounds seen in your clinic recently.
Information for patients
See the DermNet bookstore