DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Quiz
Mixed diagnoses – 10 cases (2 of 11)
For each of the ten cases, study the image(s) and then answer the questions. You can click on the image to view a larger version if required.
Each case should take approximately 2 minutes to complete. There is a list of suggested further reading material at the end of the quiz.
When you finish the quiz, you can download a certificate.
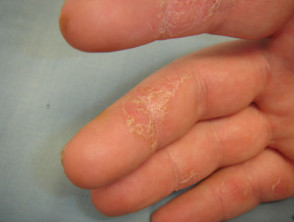
Case 2
The patient presented with persistent scaly plaques on several fingers. He complained of painful fissuring.
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.