What is bathwater PUVA?
Bathwater PUVA, also called bath-water or balneo-photochemotherapy, is a treatment for skin diseases. It is a type of phototherapy.
PUVA is an acronym: ‘P’ is for psoralen, a medication. It is used in combination with ‘UVA’, or the ultraviolet radiation of wavelength 320–360 nm.
The most commonly prescribed psoralen is methoxsalen (8-methoxypsoralen) but 5-methoxypsoralen and trisoralen are sometimes used. The psoralen may be taken by mouth (orally).
Bathwater PUVA refers to psoralen prescribed in a dilute solution of water, usually 3 mg/L. The part to be treated is soaked in this solution prior to exposure to UVA emitted from special fluorescent lamps.
What skin disorders are treated with bathwater PUVA?
Bathwater PUVA is used to treat inflammatory skin disorders, mainly:
Whole-body bathwater PUVA is prescribed to treat extensive skin disease but is not widely available because of its expense, inconvenience and risks.
Localised bathwater PUVA is more common. It is most often prescribed for psoriasis or eczema affecting the hands and feet.
How is bathwater PUVA carried out?
- The affected areas are covered with psoralen solution mixed in warm water and soaked for 15 to 30 minutes.
- The skin is gently dried off. Some centres recommend a waiting period of 15 to 30 minutes while the solution penetrates into the skin, whereas others treat immediately.
- The affected skin is exposed to UVA emitted from special fluorescent lamps.
- The treated skin should then be covered for the next 2–3 days, especially when outdoors, to protect it from inadvertent exposure to UVA.
Whole-body soaks
The patient soaks in a bathtub of psoralen solution then stands in a whole-body cabinet containing 6-foot fluorescent tubes emitting UVA.
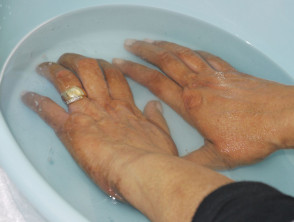
Hands and feet soaks
The hands or feet are soaked in a bowl or bucket of psoralen solution and are then exposed to UVA from 2-foot bulbs in a hand-foot box.
The actual duration of treatment will depend on the power of the lamps, the number of lamps, the patient’s skin type, and prior exposure. It may range from less than a minute to half an hour or longer.
The phototherapy staff will measure the output of the lamp and calculate the dose of UVA required. The dose may be increased each visit according to a protocol. The dose will be held the same or reduced if the condition clears, the maximum dose is reached, or side effects such as burning occur.
Hands and feet soaks
How many treatments are required?
Bathwater PUVA is most often carried out two or three times weekly. The number of treatments varies according to the severity of the skin condition and the response to the PUVA. It may range from 10–60 treatments in total.
Treatment is usually stopped when the skin condition has cleared, but maintenance treatments are used in some cases, for example, once weekly.
Bathwater PUVA may also be stopped if it proves ineffective or there are significant adverse effects.
What are the results of treatment?
About 60–80% of patients with psoriasis have good results from bathwater PUVA within 20–40 treatments. The success rates for eczema are somewhat lower.
What precautions are necessary?
Follow the directions of the phototherapy staff.
- Keep all scheduled appointments.
- Tell the staff about your health problems and the medications you take.
- Do not apply any creams to the area to be treated until afterwards.
- Avoid sun exposure on treatment and non-treatment days.
- Bathwater PUVA is not undertaken during pregnancy or breast-feeding.
What are the side effects?
The treated areas are expected to be mildly pink after each treatment. The pinkness may last several days and may be accompanied by a temporary prickling or itch. The skin is often dry; apply moisturisers frequently. Tanning usually occurs and is most prominent in darker skin types.
Burning
Burning may occur if exposure to UVA has been prolonged. The peak time for burning is 48–72 hours after exposure to UVA. Mildly burned areas may feel itchy and appear red. In severe cases, pain and blistering may occur.
Increased risk of burning occurs in the following circumstances:
- Fair skin: Fitzpatrick skin phototype 1 or 2
- If a higher concentration of psoralen solution is used
- If treated areas are exposed to the sun or another source of UVA after treatment
- If a phototoxic medication is taken prior to treatment
- If the course of treatment is interrupted; dosing should be reduced on recommencing.
In the event of a burn, apply cooling emollients frequently. Anti-inflammatory drugs such as aspirin or ibuprofen may reduce discomfort. It may take several days or longer to recover from PUVA burns as they are more prolonged than normal sunburn.
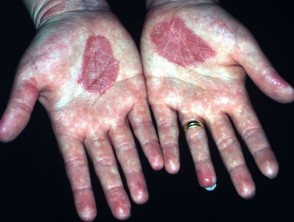
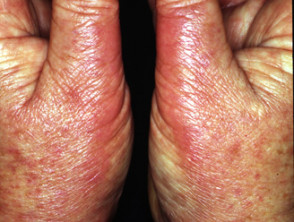
Hands burning after PUVA soaks
Skin cancer
Long term, 200 or more treatments with whole-body oral PUVA have been associated with skin cancer, cataracts and skin ageing such as freckles, wrinkles and increased dryness. The risks of bathwater PUVA are unknown.
Combination treatments
Bathwater PUVA may be carried out at the same time as other treatments are used for the skin condition. These include topical creams (e.g. corticosteroids for eczema) and oral medicines such as prednisone, acitretin and methotrexate.
Bathwater PUVA is best avoided in those on azathioprine and ciclosporin because these medicines are immunosuppressive and may increase the risk of skin cancer.
Certain topical preparations such as sunscreens and calcipotriol should not be applied to the skin to be treated as they may reduce its effect. Cosmetics and perfumes should also be avoided, as they are phototoxic and may induce severe burns.
What if the skin condition fails to clear up?
Other options may be available to treat your skin condition. Consult your dermatologist for advice.