Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated 4 January 2016.
Introduction
How it works
Different potencies
Formulations
New Zealand preparations
Side effects
How to use
Bans in cosmetic products
A topical steroid is an anti-inflammatory preparation used to control eczema/dermatitis and many other skin conditions. Topical steroids are available in creams, ointments, solutions and other vehicles.
Topical steroids are also called topical corticosteroids, glucocorticosteroids, and cortisone.
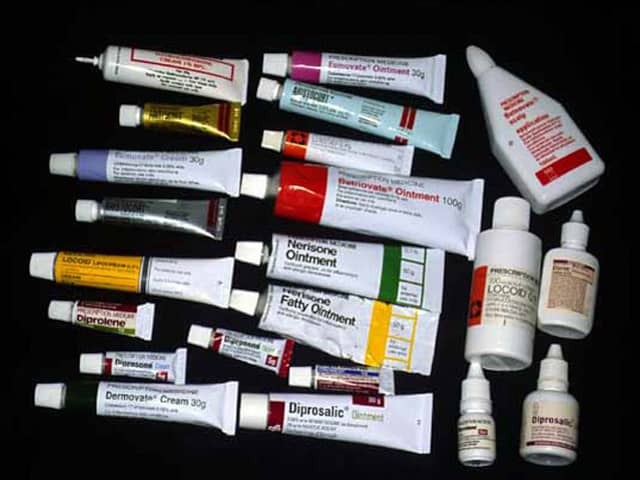
Topical steroids in differing vehicles
The effects of topical steroid on various cells in the skin are:
The potency of a topical steroid depends on:
There is little point in diluting a topical steroid, as their potency does not depend much on concentration and diluting the product does not reduce the risk of adverse effects. After the first 2 or 3 applications, there is no additional benefit from applying a topical steroid more than once daily.
A topical steroid is absorbed in different rates depending on skin thickness.
Absorption also depends on the vehicle in which the topical steroid is delivered and is greatly enhanced by occlusion.
Several formulations are available for topical steroids, intended to suit the type of skin lesion and its location. Creams and lotions are general purpose and are the most popular formulations.
Ointment
Gel or solution
As a general rule, use the weakest possible steroid that will do the job. It is often appropriate to use a potent preparation for a short time to ensure the skin condition clears completely.
Topical steroid is sometimes combined with another active ingredient, including antibacterial, antifungal agent or calcipotriol. Topical corticosteroid/antibiotic preparations should be used rarely, and short-term (eg, three times daily for one week for a small area of infected dermatitis), to reduce the risk of antimicrobial resistance.
Topical steroids are medicines regulated by Health Authorities. They are classified according to their strength. Their strength may be displayed on the packaging in some countries (eg, UK).
Side effects are uncommon or rare when topical steroids are used appropriately under medical supervision. Topical steroid may be falsely blamed for a sign when underlying disease or another condition is responsible (for example, postinflammatory hypopigmentation or undertreated atopic eczema).
Internal side effects similar to those due to systemic steroid (Cushing syndrome) are rarely reported from topical steroids, and only after long-term use of large quantities of topical steroid (eg > 50 g of clobetasol propionate or > 500 g of hydrocortisone per week).
Cases of Cushing syndrome due to topical corticosteroids most often occur because of inappropriate prescribing or over the counter sales of corticosteroids in countries where that is permitted.
Local side effects may arise when a potent topical steroid is applied daily for long periods of time (months). Most reports of side effects describe prolonged use of an unnecessarily potent topical steroid for inappropriate indications.
A topical steroid can cause, aggravate or mask skin infections such as impetigo, tinea, herpes simplex, malassezia folliculitis and molluscum contagiosum. Note: topical steroid remains the first-line treatment for infected eczema.
A potent topical steroid applied for weeks to months or longer can lead to:
Stinging frequently occurs when a topical steroid is first applied, due to underlying inflammation and broken skin. Contact allergy to steroid molecule, preservative or vehicle is uncommon but may occur after the first application of the product or after many years of its use.
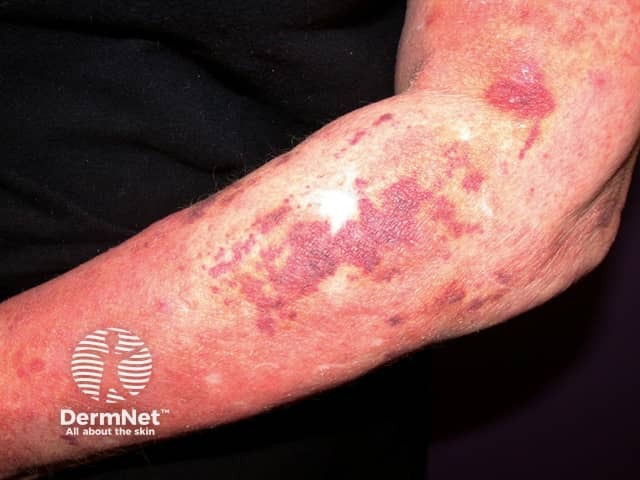
Bruising
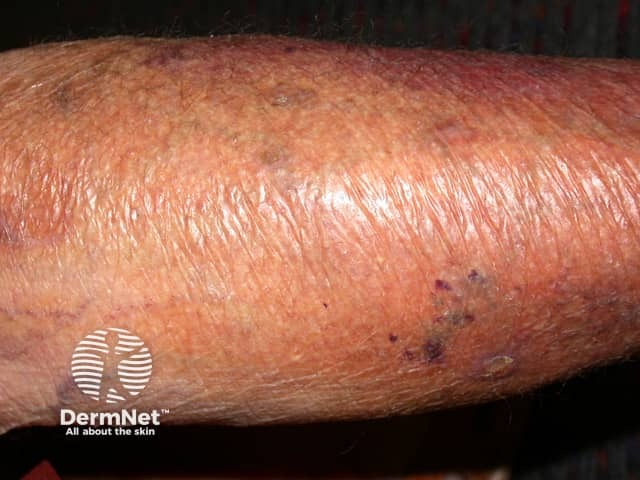
Skin thinning
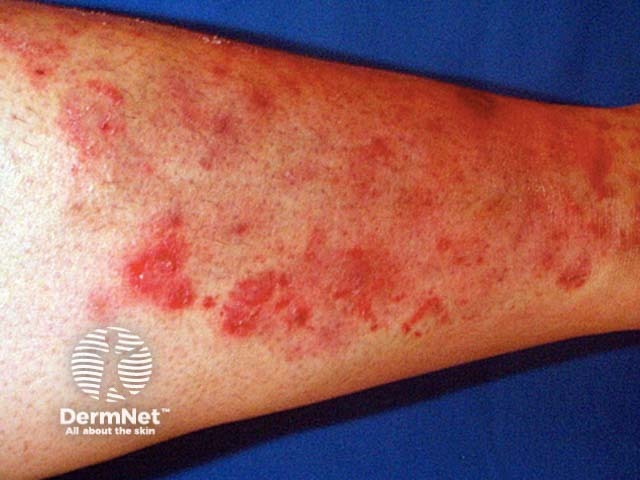
Tinea incognita
Prominent capillaries

Stretch marks
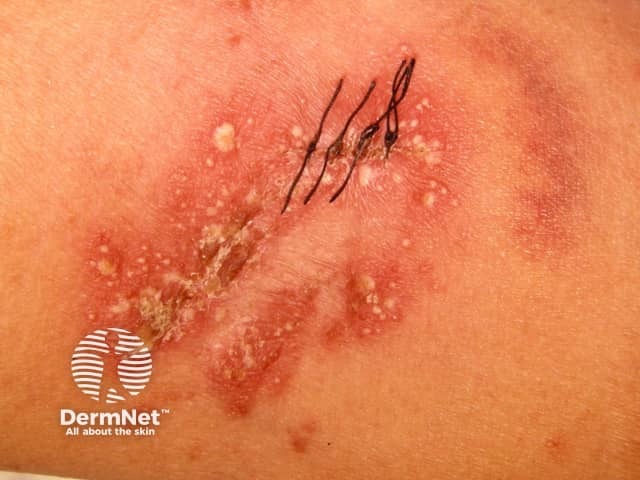
Localised pustular psoriasis
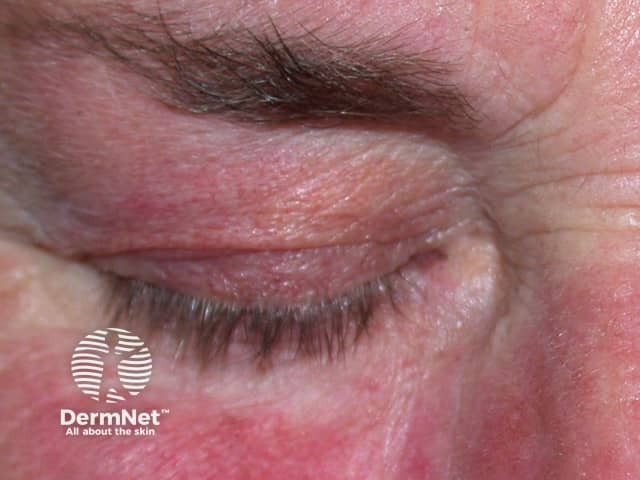
A topical steroid should be used cautiously on eyelid skin, where it commonly results in periocular dermatitis. Potentially, excessive use over weeks to months might lead to glaucoma or cataracts.
Mild and moderate-potency topical steroids can be safely used in pregnancy. Caution should be used for potent and ultrapotent topical steroids used over large areas or under occlusion, of which a proportion will be absorbed systemically.
Reports of low birth-weight infants exposed to high-dose topical steroid are not thought to be due to the medication.
Topical steroid is applied once daily (usually at night) to inflamed skin for a course of 5 days to several weeks. After that, it is usually stopped, or the strength or frequency of application is reduced.
Emollients can be applied before or after the application of topical steroid, to relieve irritation and dryness or as a barrier preparation. Infection may need additional treatment.
The fingertip unit guides the amount of topical steroid to be applied to a body site. One unit describes the amount of cream squeezed out of its tube onto the volar aspect of the terminal phalanx of the index finger.
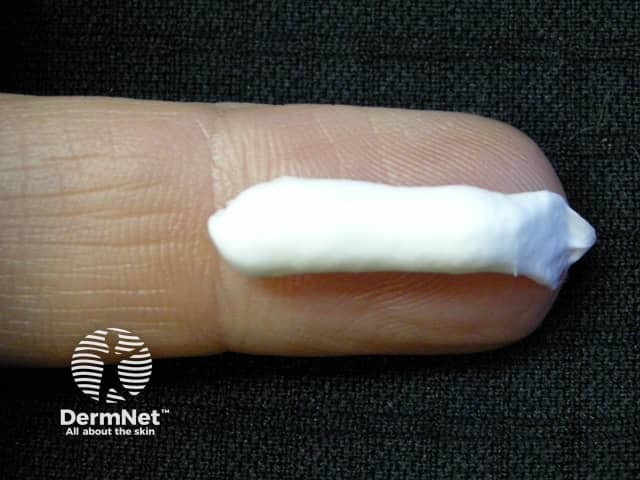
Fingertip unit
The quantity of cream in a fingertip unit varies with sex, age and body part.
Topical corticosteroids are regulated. However, a potent steroid is illegally present in some cosmetic products purchased over the counter or via the Internet, according to reports from China and several developing countries. This has resulted in many reports of steroid-dependent periorificial dermatitis, rosacea and other adverse effects.
Approved datasheets are the official source of information for medicines, including approved uses, doses, and safety information. Check the individual datasheet in your country for information about medicines.
We suggest you refer to your national drug approval agency such as the Australian Therapeutic Goods Administration (TGA), US Food and Drug Administration (FDA), UK Medicines and Healthcare products regulatory agency (MHRA) / emc, and NZ Medsafe, or a national or state-approved formulary eg, the New Zealand Formulary (NZF) and New Zealand Formulary for Children (NZFC) and the British National Formulary (BNF) and British National Formulary for Children (BNFC).