Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Cowpox is a viral skin infection caused by the cowpox or catpox virus. This is a member of the Orthopoxvirus family, which includes the variola virus that causes smallpox. Cowpox is similar to but much milder than the highly contagious and sometimes deadly smallpox disease. Cowpox should also not be confused with cowpock, which is an alternative name for a condition called milker’s nodules, which is caused by a parapox virus.
The cowpox virus got its name hundreds of years ago, from a rash that developed in dairymaids that touched the udders of infected cows. Back in 1770, an English farmer discovered that dairymaids that had contracted and recovered from cowpox not only became immune to further cases of cowpox, but also to the more serious viral disease, smallpox. In 1796 English physician, Dr Edward Jenner used the cowpox virus to inoculate a patient to prevent them from contracting smallpox. Hence this was the first successful vaccination performed.
Nowadays, cowpox is a rare disease. It mostly occurs in Great Britain and some European countries. Cows are no longer the main carrier of the virus; instead woodland rodents are the natural hosts of the virus, who then pass it on to domestic cats. Human cases are very rare and are most often contracted from the scratch or bite of domestic cats, hence the alternative name catpox. Although human-to-human transmission has not been reported, patients should be made aware that their lesions are potentially contagious.
It appears that most cases of human cowpox occur in young people (50% of patients are less than 18 years). This is possibly due to the fact that younger people may have closer contact with animals such as cats, or they have not been vaccinated against smallpox, which may confer some protection against cowpox.
Most human cases of cowpox appear as one or a small number of pus-like lesions on the hands and face, which then ulcerate and form a black scab before healing on their own. This process can take up to 12 weeks, with the following skin findings over that period:
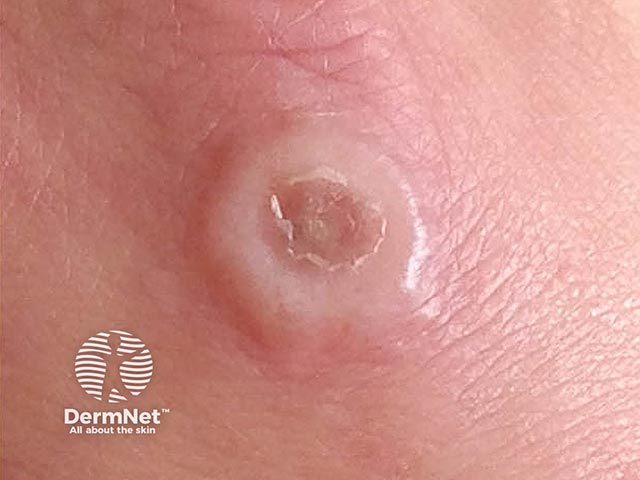
An early cowpox lesion (CP-patient1)
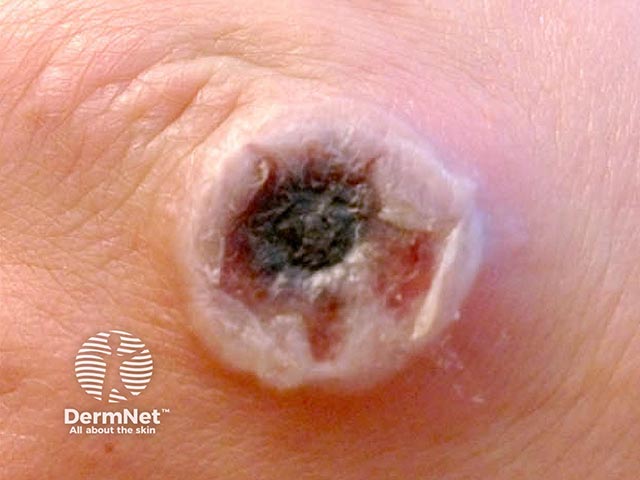
Central necrosis is developing in the blister as the cowpox lesion matures (CP-patient1)
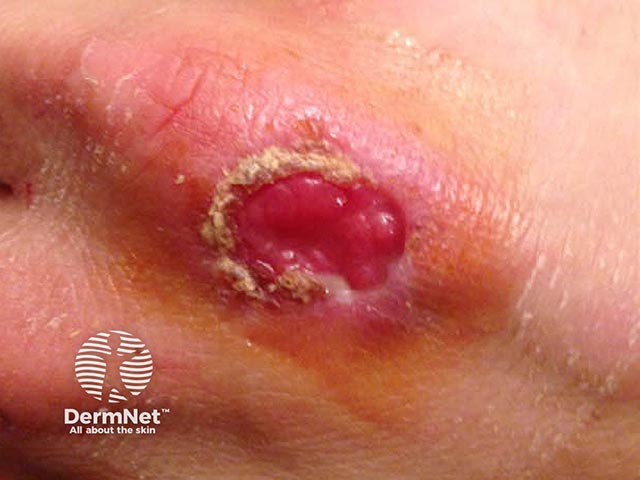
The healing cowpox ulcer (CP-patient1)
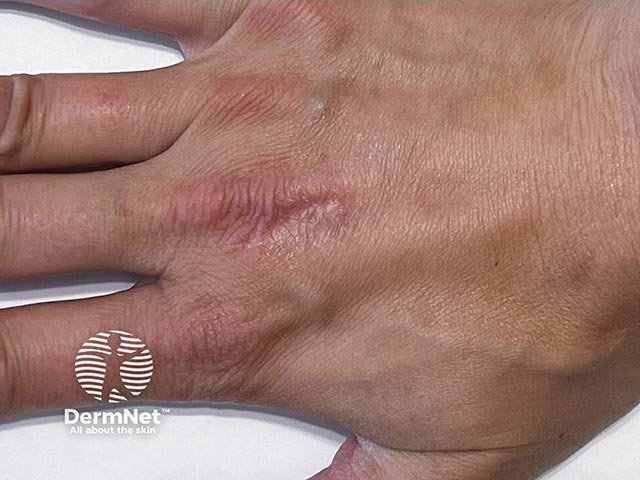
A faint atrophic scar remains after the cowpox lesion has healed (CP-patient1)
View more images of cowpox infection
Other generalised symptoms from cowpox are fever, tiredness, vomiting, and sore throat. Eye complaints such as conjunctivitis, periorbital swelling and corneal involvement have been reported. Enlarged painful local lymph nodes may also develop.
There is no cure for cowpox, but the disease is self-limiting. The human immune response is sufficient to control the infections on its own. The lesions heal by themselves within 6–12 weeks. Often patients are left with scars at the site of the healed pox lesions.
Patients may feel unwell and require bed rest and supportive therapy. Wound dressings or bandages may be applied to lesions to prevent spread to other sites and potentially to other people.
Patients with underlying skin conditions, such as atopic dermatitis, may be at greater risk of generalised cowpox.