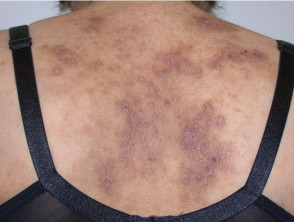
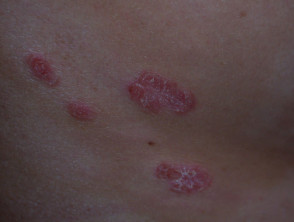
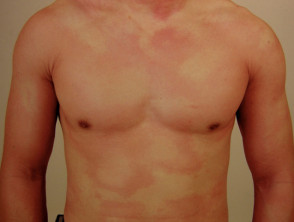
Submit your photo of COVID-19-related skin conditions
What is COVID-19?
COVID-19 (coronavirus disease 2019) is an infection caused by the virus SARS-CoV-2, that can lead to serious respiratory illness and can be fatal.
The World Health Organisation (WHO) declared on 11 March 2020 that the COVID-19 outbreak was officially a pandemic, as COVID-19 had spread rapidly worldwide [1].
Should my skin medications be stopped?
Commonly used systemic medications for severe skin conditions include immunomodulators or immunosuppressive drugs. These may include a biological agent, a disease-modifying anti-rheumatic drug (DMARD), or a systemic steroid. Dermatological medications are not known to increase the risk of acquiring COVID-19.
Biological agents (biologics)
- In a study conducted between February 2020 and April 2020 examining 5206 patients in northern Italy on biological agents for psoriasis, there were no COVID-19 related deaths and only four required hospital admission [2].
- It is recommended a patient should continue a biological agent if they are well [3,4].
- Biological agents may be less effective if stopped for a period and then restarted due to production of anti-drug antibodies.
- Starting the use of a new biological agent should be considered on a case-by-case basis. It may be appropriate to delay treatment, particularly if there are risk factors for severe COVID-19 disease.
If you have tested positive (or are a presumed case) for COVID-19, the biologic medication should be STOPPED for at least four weeks or until you have fully recovered from COVID-19 [3,4]. You should inform any doctor involved in your care that you are on this medication.
Other immunomodulators and immunosuppressants
If you are currently well, and do not have any other chronic medical conditions [3,4]:
- Continue taking your medications as prescribed
- Remember that these medications were started to treat a severe, long-term medical condition
- The skin condition is very likely to deteriorate if the systemic medication is stopped suddenly
- The COVID-19 pandemic may continue on for years
- Those with risk factors for severe disease with COVID-19 should be reviewed on a case-by-case basis [3].
If you have tested positive (or are a presumed case) for COVID-19:
- Inform your doctor about your skin condition and the medications you are currently taking
- Immunomodulator or immunosuppressant medication should be STOPPED for at least four weeks or until you have fully recovered from COVID-19 [4]
- EXCEPT systemic corticosteroids used long term should not be abruptly stopped. Dose adjustments may be required and should be done on consultation with your doctor [4].
If you have cold or flu-like symptoms [4]:
- Local guidelines may apply; ask your doctor
- A dose reduction or treatment interruption for two weeks may be considered [4]
- Systemic steroids used long term should be continued; ask your doctor if you should stay on the same dose, increase it, or reduce the dose.
The influenza vaccine by intramuscular injection is highly recommended for all patients without contraindications. See immunisation in immunosuppressed dermatology patients.