Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Autoimmune/autoinflammatory Blood vessel problems
Author: Dr Vania Sinovich MBChB FRACP, Registrar, Dept of Dermatology Waikato Hospital, Hamilton, New Zealand, 2005. Updated by A/Prof Amanda Oakley, January 2016.
Introduction Demographics Causes Clinical features Diagnosis Treatment Outlook
Granulomatosis with polyangiitis is an uncommon but potentially fatal form of vasculitis. There is an immune reaction in which antibodies damage small blood vessel walls and surrounding tissues.
Multiple organs are often involved. The most commonly affected sites are the ear, nose, throat, lungs, eyes and kidneys. Mild forms without kidney involvement may occur.
Granulomatosis with polyangiitis was previously known as Wegener granulomatosis.
Granulomatosis with polyangiitis affects both sexes equally. It occurs in patients of all ages with a mean age of 41 years. It occurs more commonly in white patients than in blacks or Asians.
The cause of granulomatosis with polyangiitis is unknown. It is classified as an autoimmune disease and the cytoplasmic antineutrophil cytoplasmic antibody (c-ANCA) directed against serine proteinase three antigen (PR3-ANCA) is thought to be pathogenic. It may be triggered by a bacterial infection.
Genetic mutations may be involved, but granulomatosis with polyangiitis is not inherited.
Patients with granulomatosis with polyangiitis may complain of various non-specific symptoms especially:
Symptoms affecting the ear, nose and throat are common, affecting 70% of patients at onset and in 92% of patients during granulomatosis with polyangiitis.
Ear, nose and throat manifestations of granulomatosis with polyangiitis include:
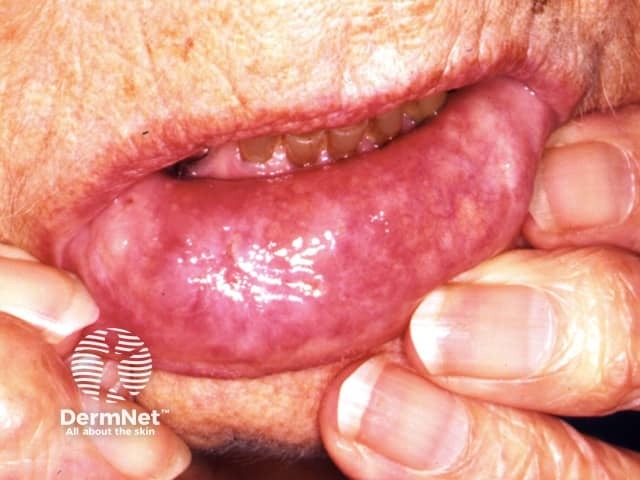
Lip ulceration due to granulomatosis with polyangiitis
Lung involvement occurs in 45% of patients with granulomatosis with polyangiitis at presentation and 87% during the disease, most often resulting in:
Chest x-rays may be abnormal, either showing diffuse disease (67%) or isolated areas (58%).
Renal involvement occurs in 20% of patients at presentation and in 85% during granulomatosis with polyangiitis. It may manifest as oliguria (decreased urine production) and haematuria (blood in urine).
Close monitoring of renal function is required for all patients (blood and urine tests).
Eye symptoms occur in 28–58% of patients with granulomatosis with polyangiitis and are part of the initial presentation in 8 to 16% of patients. The most common problems are:
The skin may be affected in 40–50% of patients with granulomatosis with polyangiitis. Skin problems include:
Musculoskeletal problems occur in 30–50% of patients at presentation and in 65–75% of patients during the disease. These include:
Neurological symptoms are rarely a presenting feature but may occur in 22-50% of patients during granulomatosis with polyangiitis. Peripheral nerves are mostly affected leading to loss of or abnormal sensations or weakness of some muscles. Involvement of the central nervous system (i.e. the brain and spinal cord) occurs in < 10% of cases.
The exact frequency of gastrointestinal symptoms in granulomatosis with polyangiitis is unknown. Symptoms are most often:
Cardiac problems occur in 12–30% of patients with granulomatosis with polyangiitis. These include:
The diagnosis of granulomatosis with polyangiitis is not always straightforward.
Blood count abnormalities in granulomatosis with polyangiitis may include:
Antineutrophil cytoplasmic antibody (ANCA) is the most useful blood test. A particular type, c-ANCA is highly specific for granulomatosis with polyangiitis and affects 70% of patients with the disease. It is recognised by cytoplasmic staining pattern and is directed against an enzyme, proteinase-3. Protoplasmic-staining perinuclear antineutrophil cytoplasmic antibodies, called p-ANCA, occur in 70% of people with granulomatosis with polyangiitis.
A positive test result for rheumatoid factor occurs in 50-60% of patients with granulomatosis with polyangiitis and can be misleading because this normally indicates rheumatoid arthritis.
A skin biopsy may be helpful if it demonstrates granulomatous vasculitis (inflamed blood vessels with a certain pattern of inflammation). Necrotising vasculitis, extravascular palisading granulomas, and leukocytoclastic vasculitis may also occur.
Granulomatosis with polyangiitis is usually treated with glucocorticoids and cyclophosphamide. Other drugs used include:
Skin lesions may be treated symptomatically with topical steroids.
Surgery may be necessary to repair tissue after fibrosis or necrosis.
Granulomatosis with polyangiitis may be slowly or rapidly progressive. There is often no way to predict which patients will continue to have limited, milder forms of the disease and which will go on to more severe progressive, generalised forms of the disease. Untreated, severe disease has a high mortality rate due to infection, lung or heart disease, renal failure or malignancy.
Disease activity should be monitored regularly. It is especially important to closely check kidney function. Many different specialists may need to be involved in the patient’s care. Careful and long-term follow-up is required.