Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Shendy Engelina, Core Medical Trainee, Northampton General Hospital, UK. Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, April 2016.
Introduction
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Treatment
Outcome
Abnormal levels of circulating thyroid hormone (thyroxine) and underlying diseases may lead to alterations in the appearance of skin, hair and nails. The thyroid gland can be overactive, resulting in hyperthyroidism, discussed here, or underactive, resulting in hypothyroidism.
Hyperthyroidism is due to excessive thyroxine. It is also known as thyrotoxicosis. It can lead to a variety of signs and symptoms.
Hyperthyroidism:
There are several causes for hyperthyroidism.
Graves disease is the most common cause of hyperthyroidism (80%).
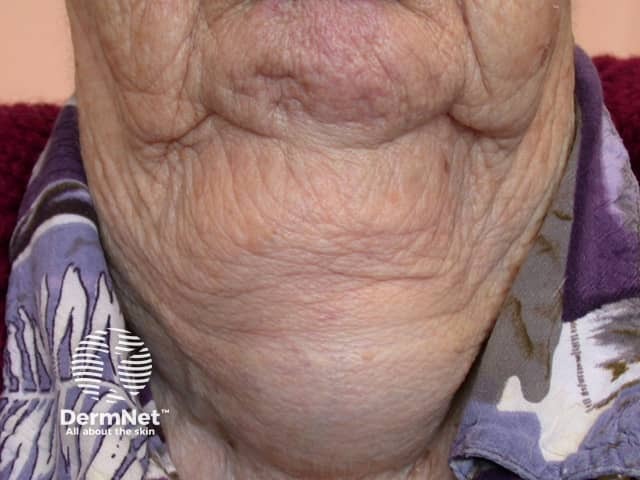
Goitre
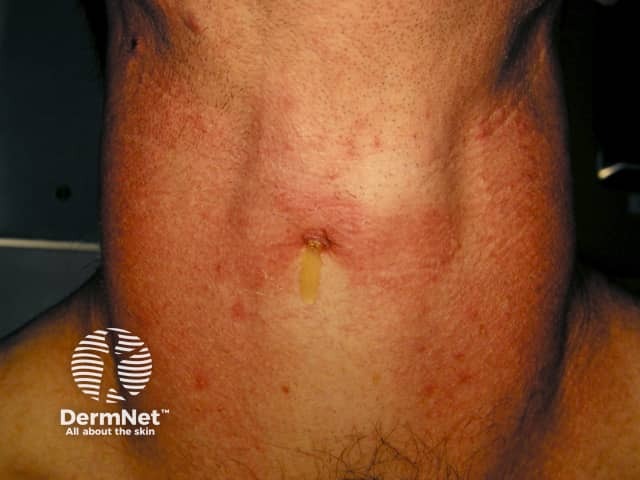
Goitre
A thyroid nodule is a benign growth within the thyroid gland.
Hyperthyroidism arises from:
Subacute thyroiditis is also known as De Quervain thyroiditis.
Rare causes of hyperthyroidism include:
Hyperthyroidism results in an increase in the body’s metabolic rate, which characterised by:
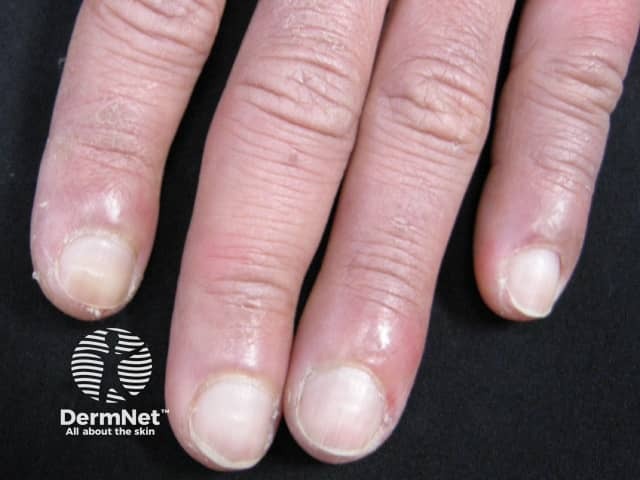
Thyroid acropachy
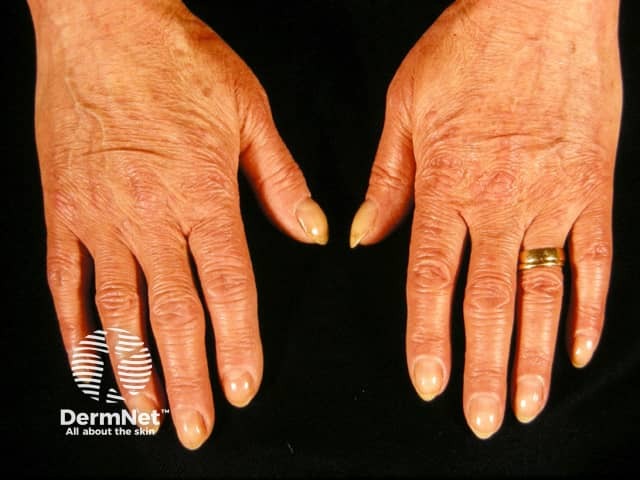
Thyroid acropachy
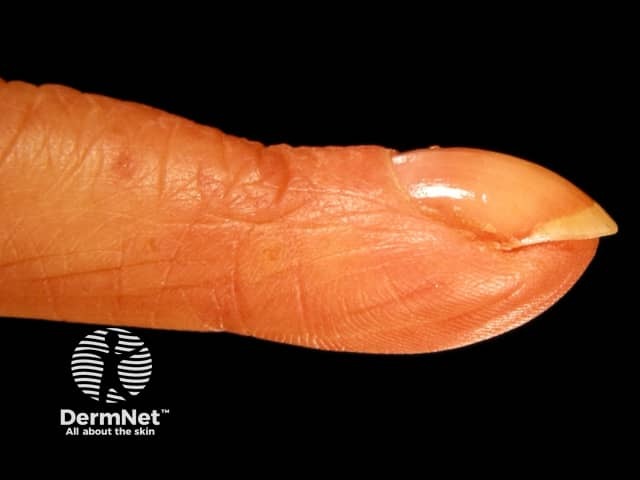
Thyroid acropachy
Other common systemic features include palpitations, tremor, weight loss, heat intolerance, anxiety and menstrual disturbance (irregular or light period).
Graves disease may also cause thyroid dermopathy resulting in pretibial myxoedema and exophthalmos, which are associated with the presence of thyroid antibodies.
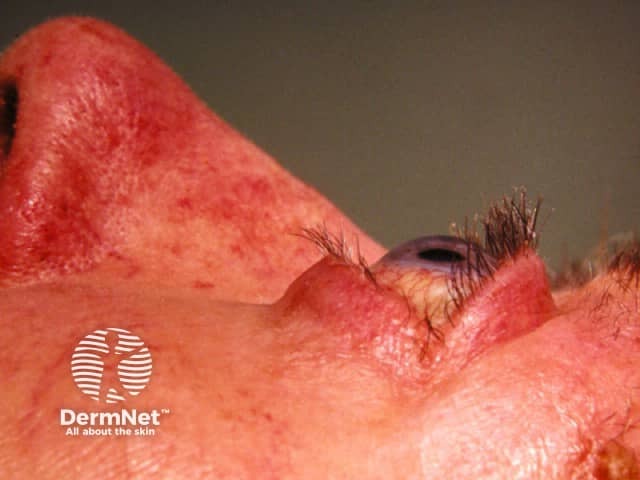
Thyroid ophthalmopathy
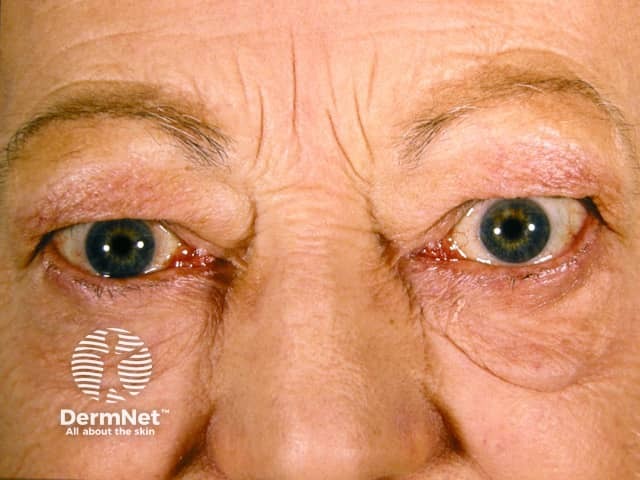
Thyroid ophthalmopathy
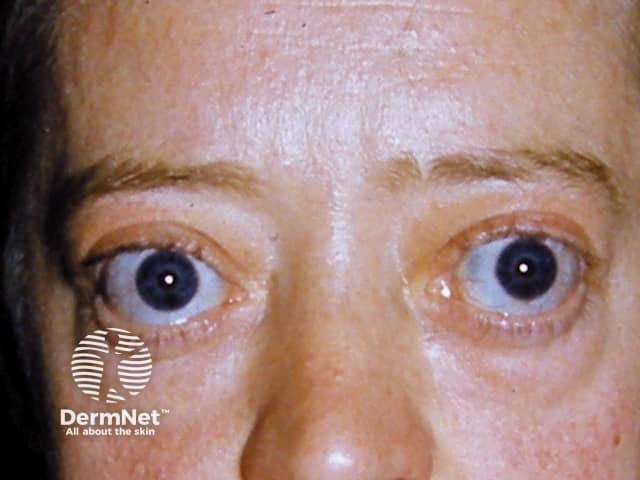
Thyroid ophthalmopathy
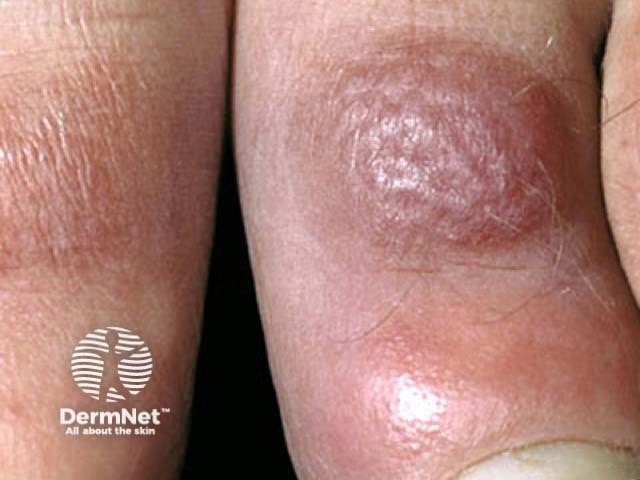
Pretibial myxoedema
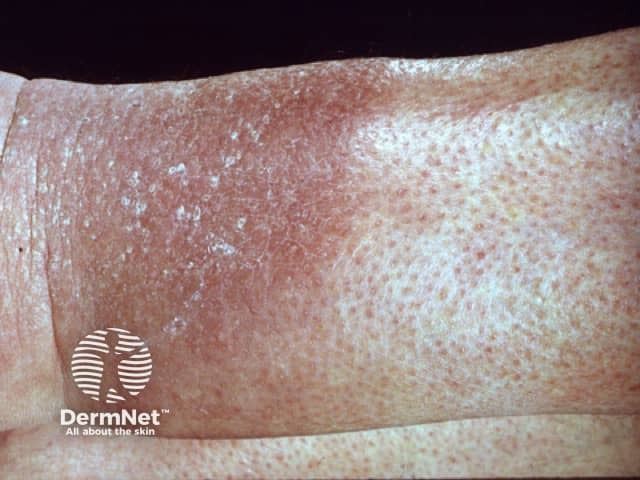
Pretibial myxoedema
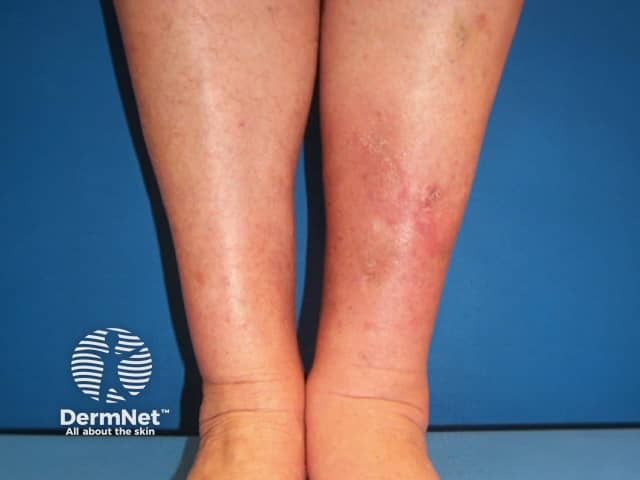
Pretibial myxoedema
Untreated hyperthyroidism can cause serious systemic complications including:
Medical emergencies associated with hyperthyroidism include thyroid storm and thyrotoxic periodic paralysis.
Thyroid storm is also called thyroid crisis.
Thyrotoxic periodic paralysis is characterised by acute onset of hypokalaemia.
Hyperthyroidism is diagnosed with thyroid function tests (TFTs).
Interpretation of thyroid function tests |
|||
|---|---|---|---|
TSH |
Free T4 (thyroxine) |
Free T3 (triiodothyronine) |
|
(Primary) hyperthyroidism |
Low |
High |
High |
Secondary hyperthyroidism |
High |
High |
High |
Subclinical hyperthyroidism |
Low |
Normal |
Normal |
Primary hypothyroidism |
High |
Low |
Low or normal |
Secondary hypothyroidism |
Low or normal |
Low |
Low or normal |
Subclinical hypothyroidism |
Borderline high |
Normal |
Normal |
Sick euthyroid syndrome |
Low |
Low |
Low |
Serum autoantibodies are markers of autoimmune disease. They should include:
Full blood count and inflammatory markers, such as C-reactive protein, are routinely included to screen for anaemia (commonly associated with hyperthyroidism) and systemic infection causing thyroiditis.
Imaging should include:
Hyperthyroidism is either treated with medication, by radioactive iodine, surgery or a combination of these.
Radioactive iodine is usually indicated for relapses of Graves disease and toxic nodular goitre. However, it has increasingly been used as first-line treatment for hyperthyroidism in teenagers.
Partial or total thyroidectomy is surgical removal of part or the whole of the thyroid gland respectively.
Treatment of hyperthyroidism is usually effective. Regular thyroid function tests are recommended following successful treatment, as some individuals develop further relapses, with annual blood tests long term.