Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Treatments Blood vessel problems
Authors: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Revised and updated by Dr Arun Gangakhedkar, Paediatrician, Waitemata DHB, Auckland, New Zealand, 2012. Copy edited by Gus Mitchell. January 2021.
Introduction
Associations and complications
Treatment
Outcome
Infantile haemangioma, also known as a strawberry naevus, is the most common benign vascular skin tumour in children.
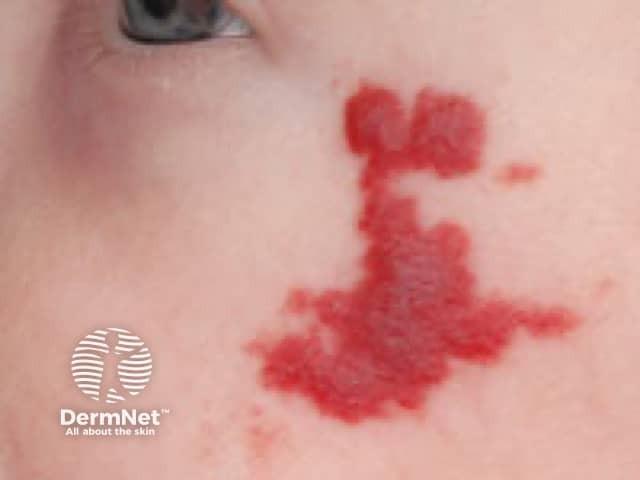
Infantile haemangioma, face
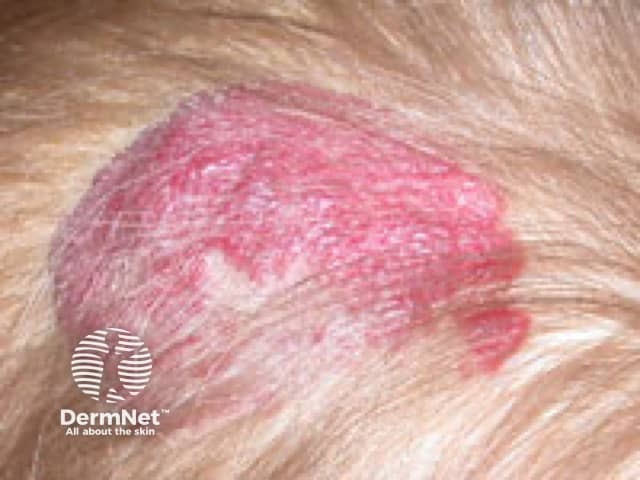
Regressing infantile haemangioma, scalp
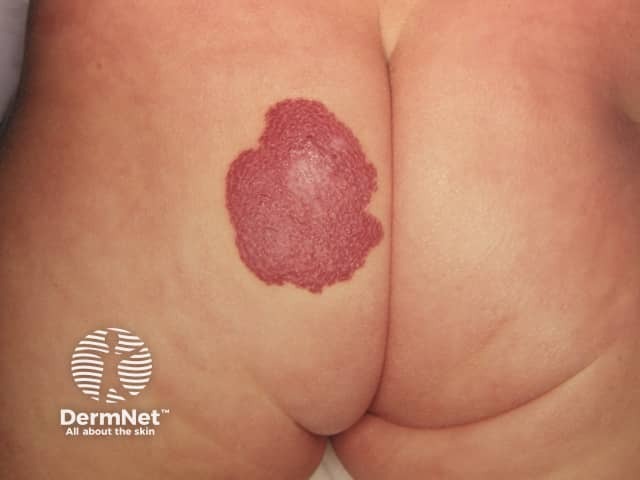
Infantile haemangioma, buttock
Potentially life altering skin changes are reported in 50–65% of untreated infantile haemangiomas. Kasabach-Merritt syndrome, a rare complication of a rapidly growing vascular lesion, is no longer thought to arise from infantile haemangioma.
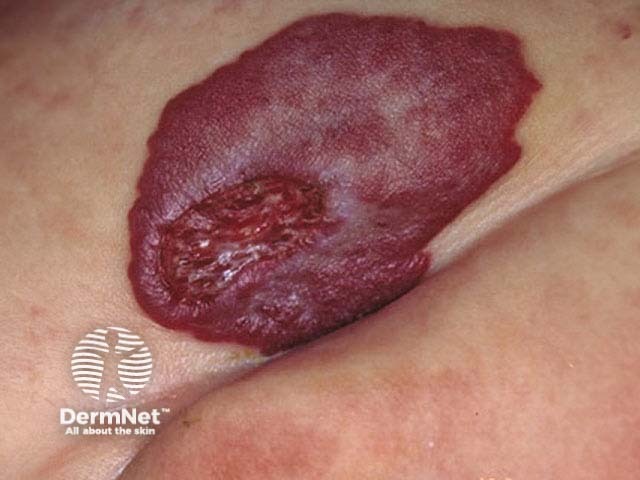
Painful ulceration is the most common complication occurring in 15% of infantile haemangiomas around 4 months of age. A white change may herald the onset of ulceration while the lesion is still solid. Large segmental, superficial, or mixed lesions in the proliferation phase, and those located on the tip of nose, neck, perineum, or flexural areas are prone to ulceration and scarring. Large ulcerated infantile haemangiomas are are at particular risk of profuse bleeding and secondary bacterial infection.
Periorbital infantile haemangiomas: Nasal lesions greater than 1 cm can affect the visual axis, potentially causing amblyopia. Optic nerve compression may occur in orbital lesions. Astigmatism may result from direct pressure from a growing haemangioma. Other complications of periorbital infantile haemangiomas can include conjunctival involvement, ptosis, proptosis, and strabismus.
Periauricular infantile haemangiomas: Lesions around the ear can obstruct the external auditory canal causing hearing impairment and otitis externa.
Peri-nasal or columella infantile haemangiomas: Significant complications of infantile haemangiomas on or around the nose include: the Cyrano nose deformity with scarring, fibrofatty infiltration, and disfigurement; nasal obstruction; alteration of the nasal valve; ulcerative destruction of the columella and part of the nasal septum.
Peri-oral or lip infantile haemangiomas: Infantile haemangiomas around the mouth and lower lip can cause mechanical feeding difficulties, ulceration, and disfigurement.
Beard or cervicofacial infantile haemangiomas: Infantile haemangiomas involving the preauricular region, chin, anterior neck, and lower lip can be associated with a deep glottic extension causing airway obstruction, stridor, hoarseness, or aspiration. Two-thirds of beard lesions have an associated airway haemangioma, and one third of airway haemangiomas have an associated cutaneous lesion. Bilateral skin lesions of these skin sites carry an increased high risk of airway involvement.
Infantile haemangiomas of other special areas: Flexural perineal infantile haemangiomas are particularly prone to ulceration and infection. Scalp lesions greater than 2 cm carry a high risk of profuse bleeding and scarring. Breast lesions in girls can potentially alter structural development and cosmesis.
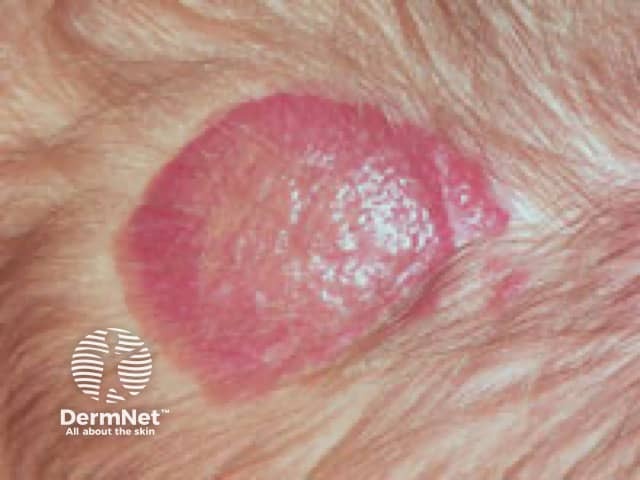
Infantile haemangioma, scalp
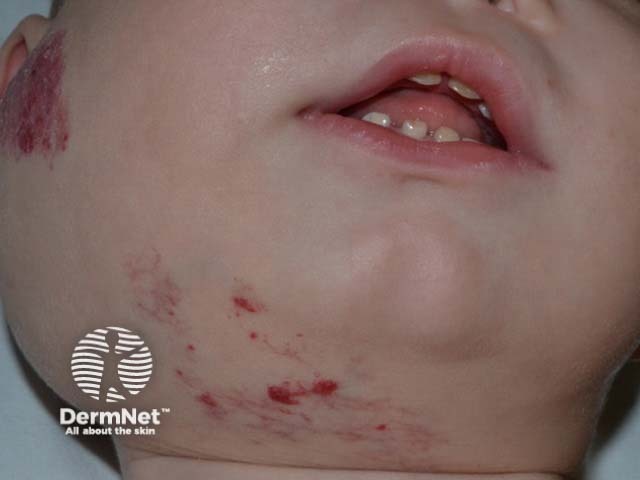
Cervicofacial infantile haemangioma
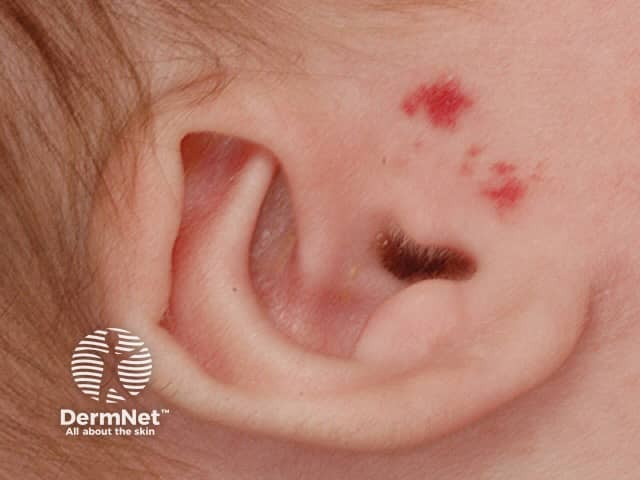
Preauricular infantile haemangioma
Infantile haemangiomas can develop in the liver, gastrointestinal tract, parotid gland, and brain. Most are asymptomatic, but life-threatening complications can occur.
Parotid infantile haemangioma: is the most common salivary gland tumour of childhood presenting with or without superficial skin involvement. It has a rapid initial growth followed by a prolonged gradual growth beyond nine months of age. Ultrasonography helps with the diagnosis and MRI defines the size, extent, and relationship of the tumour to adjacent structures.
Parotid infantile haemangioma can cause:
Infantile hepatic haemangioma: is the most common benign hepatic vascular tumour. It can be focal, multifocal, or diffuse. Most focal and multifocal infantile hepatic haemangiomas are asymptomatic in children, but diffuse infantile hepatic haemangioma can present with:
Five or more cutaneous lesions may indicate the presence of infantile hepatic haemangioma.
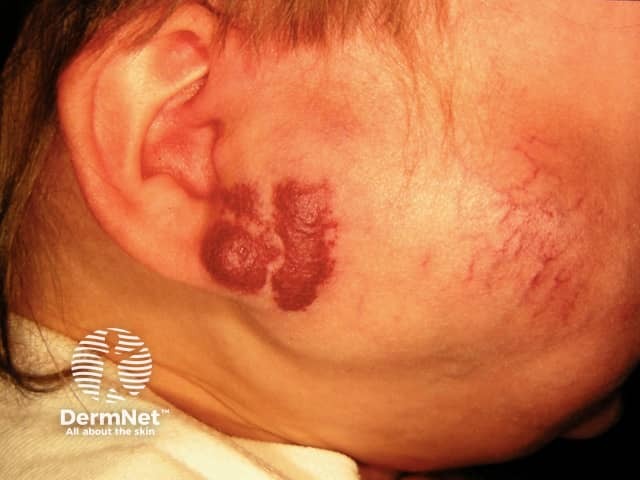
Vascular malformation
Segmental plaque-like cutaneous infantile haemangiomas may be associated with neurological abnormalities and congenital anomalies of the heart, great arteries, and cerebral vessels, as seen in PHACE(S), SACRAL, LUMBAR and PELVIS syndromes.
A collaborative treatment plan discussing risks and benefits with informed family consent promotes a good physician-patient relationship. Monitoring photo-documentation (front and side-on views) may be sufficient for small lesions with low complication risks. Emergency management may be required for life-threatening presentations and urgent intervention is indicated for some complicated infantile haemangiomas.
Haemangiomas that are cosmetically sensitive or otherwise high-risk require the following treatments.
Most infantile haemangiomas involute well, and over half of children have normal skin at the site of the lesion. Residual changes may include scar, redundant skin, anetoderma, fibrofatty residuum, telangiectases, or dyspigmentation.
The risk of slow involution and scarring is increased for infantile haemangiomas involving the tip of nose, lip, and parotid gland.
Segmental infantile haemangiomas have high rates of complications due to local, visceral, and associated anomalies.