Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2005. Updated by Dr Sara de Menezes, Basic Physician Trainee, Alfred Health, Melbourne, Australia; Chief Editor, Dr Amanda Oakley, Hamilton, New Zealand, July 2016.
Introduction - anaemia Introduction - iron-deficiency anaemia Demographics Causes Clinical features Systemic symptoms Tests Treatment Side effects Outcome
Anaemia (American spelling, anemia) is a deficiency of red blood cells. It can occur either through the reduced production or an increased loss of red blood cells.
Three essential elements must be present to produce red blood cells: iron, vitamin B12 and folic acid. The most common cause of anaemia is iron deficiency, affecting more than 2 billion people worldwide.
The estimated prevalence of iron deficiency worldwide is double that of iron deficiency anaemia. Iron deficiency anaemia occurs when there is insufficient iron to create red blood cells
The main groups at risk of iron deficiency and iron-deficiency anaemia are pre-school children, adolescents, pregnant and young women, which are times of increased physiological need for iron.
In people living in developing countries, iron deficiency tends to be due to insufficient dietary iron intake or to blood loss from intestinal worm colonisation. In high-income countries, iron deficiency may result from a vegetarian diet, chronic blood loss, or malabsorption.
Diet-related iron deficiency
Blood loss
Gastrointestinal iron deficiency
Medication-related iron-deficiency
Other conditions
The signs and symptoms of an iron deficiency depend on whether the patient is anaemic, and if so, how fast the anaemia develops. In cases where anaemia develops slowly, the patient can often tolerate extremely low concentrations of red blood cells (< 100 g/L) for some weeks before developing any symptoms. The first symptoms to appear are due to low delivery of oxygen to tissues, and may include:
Skin signs of anaemia are often subtle and may include:
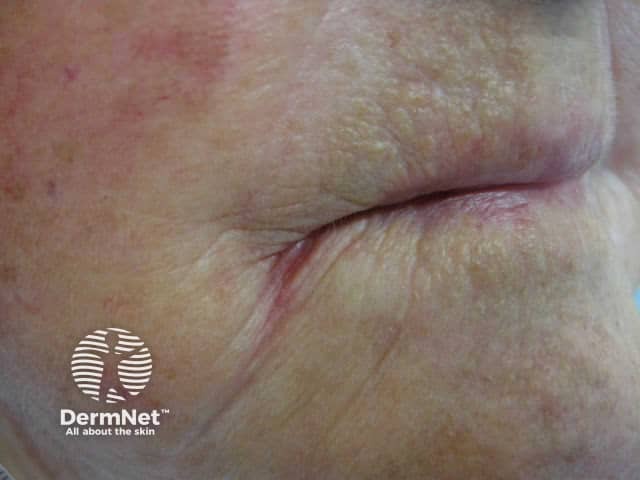
Angular cheilitis
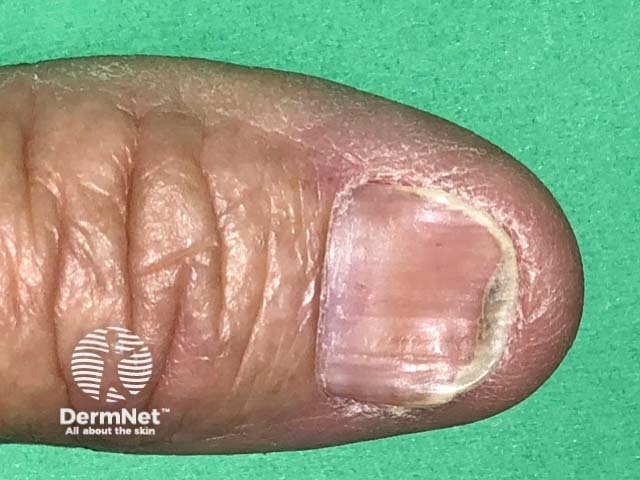
Koilonychia
Other characteristic manifestations of iron deficiency anaemia may include:
Iron deficiency may also predispose to bacterial and fungal infections such as impetigo, boils and candidiasis.
A full, or complete, blood count (FBC, CBC) is essential to detect anaemia. Iron deficiency can be present when blood count indices are normal.
If anaemia is due to iron deficiency, the cells are smaller and contain less haemoglobin resulting in lowered red blood cell count or haematocrit, mean corpuscular volume (MCV) and mean cell haemoglobin concentration (MCH). Reticulocyte haemoglobin content (Ret-Hb), which tends to be low in iron deficiency anaemia, can be used to monitor response to iron replacement. Red cell distribution width (RDW) can reveal mixed iron and vitamin B12 deficiency as this results in red cells of variable size.
Ferritin is a measure of iron stores and is the most sensitive and specific test for iron deficiency. Low levels of ferritin less than 15 μg/ml are diagnostic of iron deficiency. Levels higher than 40 μg/ml in a healthy person are considered optimal.
Normal or high levels of ferritin do not exclude iron deficiency, because ferritin acts as an acute phase reactant. Levels are higher in the presence of chronic inflammation (eg, rheumatoid arthritis) when erythrocyte sedimentation rate (ESR) or C-reactive protein (CRP) are elevated. In the context of inflammation, significantly higher cut-off values for ferritin are used (eg, 100 μg/ml) and are more predictive of iron deficiency. Ferritin is also more elevated in patients with chronic kidney disease and heart failure.
In iron deficiency:
Retest iron status after three months of iron supplementation.
Older patients sometimes have unexplained iron deficiency anaemia. If bowel investigation is negative, bone marrow examination may be considered in undifferentiated cases.
Once iron deficiency has been established, the underlying cause should be investigated and managed (correct/control GI bleeding or menstrual blood loss, eg, with the levonorgestrel-releasing intrauterine device or tranexamic acid for a woman with heavy periods). Most people with iron deficiency anaemia will need iron replacement therapy to correct the anaemia and replenish iron stores. The benefit of treating iron deficiency without anaemia is still uncertain. Specific groups of patients like those with cardiovascular disease (with heart failure or angina) should receive red blood cell transfusions which will correct both hypoxia (low oxygen) and the iron deficiency.
Red meat contains haem iron, which is readily absorbed. Non-haem iron sources may need the help of vitamin C in the form of fresh fruit or tablets.
Many manufactured foods contain iron, so it is essential to read the labels.
Calcium (in milk products) and tannin in tea, coffee and red wine, reduce the absorption of non-haem iron, so these should be taken several hours before a meal. Conversely, vitamin C (ascorbic acid) enhances the absorption of iron when they are taken together.
Iron supplementation is safe in pregnancy, infants, children and adults. It can be used in iron deficiency anaemia and anaemia of chronic disease.
Iron preparations come in the form of tablets, oral liquids and injection. Oral preparations are most commonly used.
Oral iron preparations from reputable sources include:
Enteric-coated and slow-release formulations are less well absorbed, but better tolerated. Taking iron with vitamin C (ascorbic acid) may increase its absorption and help replenish iron stores more quickly. Lower dose preparations are less effective.
In anaemic patients, once haemoglobin levels are corrected to within the normal range, iron replacement should be continued for a further three months to replenish iron stores. Aim for serum ferritin levels over 50 μg/ml.
Iron absorption is reduced in the presence of gastrointestinal disease (atrophic gastritis, infection with Helicobacter pylori, coeliac disease, inflammatory bowel disease), chronic kidney disease and inflammatory conditions.
Iron may interfere with the absorption of some medications, including:
Iron absorption is decreased by calcium, tannins (in tea and red wine) and plant phytates (in cereals). Iron should be taken at a different time of day.
Intravenous infusions are used in patients that cannot tolerate oral supplementation, or where iron losses exceed the daily amount that can be absorbed orally. Intravenous iron is also essential in the management of anaemia in patients with chronic kidney disease that are receiving dialysis and treatment with erythropoiesis-stimulating agents (agents to stimulate red blood cell production). Parenteral iron in patients with heart failure has led to improvements in physical performance, symptoms and quality of life.
The most commonly used intravenous preparation is iron polymaltose, which is infused over several hours. Other intravenous preparations include low molecular weight iron dextran, iron carboxymaltose, iron sucrose and ferric gluconate complex.
Adherence to recommended oral iron replacement therapy may be poor with some patients as iron preparations are associated with a high incidence of side effects. These include nausea, constipation, diarrhoea and black stools. To reduce this:
Intravenous iron polymaltose may cause infusion reactions such as headache, nausea and muscle pains. Severe allergic reactions including anaphylaxis have been reported. Delayed reactions include fever and joint pain. Extravasation is rare but may lead to persistent brown discolouration of affected skin.
Intramuscular injections of iron are now rarely used. They may result in long-lasting brown staining (siderosis), pain, haematoma and sterile abscesses. Improvement in iron staining has been reported following treatment with Q-switched ruby and Nd:YAG laser.
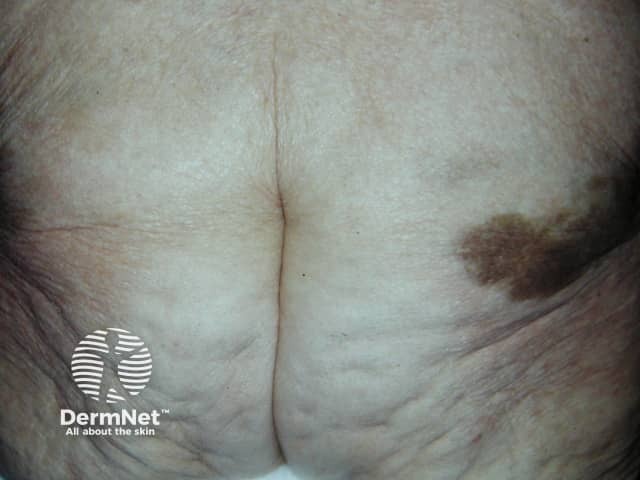
Intramuscular
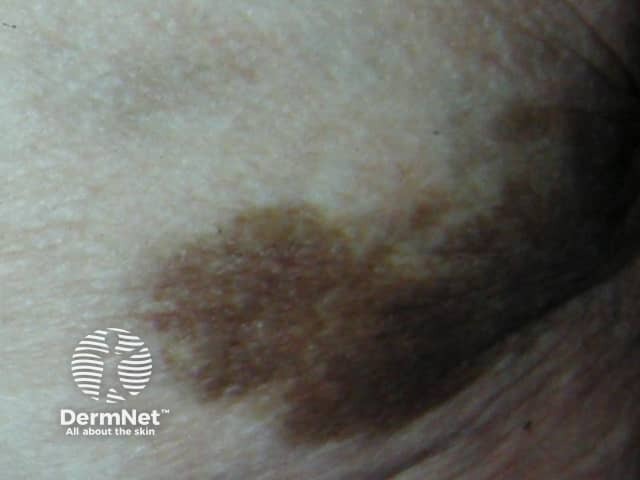
Intramuscular, close-up
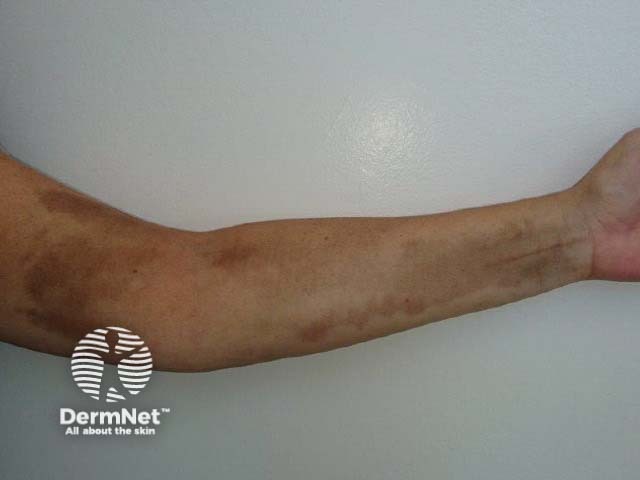
Intravenous extravasation
Most patients with uncomplicated iron deficiency anaemia should experience:
In those who do not respond to treatment, alternative diagnoses need to be considered, for example, B12 or folate deficiencies, myelodysplastic syndrome (bone marrow abnormalities) and inherited anaemias.