Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Infections Diagnosis and testing
Author: Natasha Lee BSc (Hons), Visiting Medical Student, University of Leeds; Chief Editor: Hon A/Prof Amanda Oakley, Hamilton, New Zealand. August 2014.
Introduction
Introduction - viral skin swab
How it works
Viral cell cultures
Blood tests
Polymerase chain reaction (PCR)
Enzyme-linked immunosorbent assay (ELISA)
Electron microscopy
Resistance testing
Various tests are carried out in a laboratory to establish or confirm the diagnosis of a viral skin infection. Although a thorough history and examination of the patient are vital, laboratory tests can help the clinician to make a diagnosis.
A viral skin swab is a sterile implement lightly rubbed against a visible skin lesion or vesicle. The swab is then sent to the laboratory in a viral transport medium for further viral cell culture and virus identification.
A viral swab from an external skin lesion or mucosal surface can detect:
In addition, a viral swab from oral skin mucosa can detect:
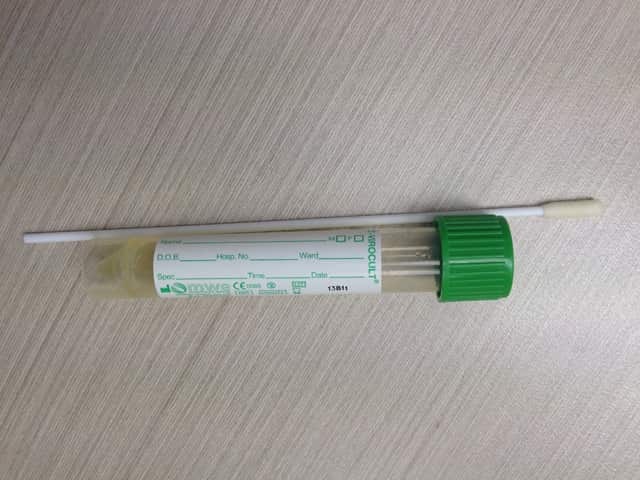
Viral skin swab
Viral cell culture places samples into suitable cell cultures that the virus being tested can infect. When the cells show particular changes the culture is positive. Viral cell culture can identify HSV, VZV, morbillivirus (cause of measles) and other viruses.
Blood tests for the investigation of viral infections include:
PCR involves isolating and amplifying lengths of DNA and then detecting known genetic sequences of microorganisms. Skin swabs can be used to identify:
ELISA can test for specific organisms either by detecting the antigen during a current infection or more commonly, antiviral antibody. The detection of the antibody confirms contact with the virus at some time but it is not necessarily the reason for a current infection.
Most commonly detected viral antibodies are to:
A skin biopsy may be useful in the diagnosis of viral infection. A viral cytopathic effect may be observed on histopathology or Tzanck smear, or specific features characteristic of the particular infection may be present.
Electron microscopy involves directing a beam of electrons at a sample producing an image. It can provide much higher resolution images than a standard light microscope. It is rarely used in practice. However it can be useful to identify atypical and rare viral infections in the immunosuppressed patients presenting with unusual skin lesions.
Resistance testing in viruses is done to aid the clinician as to what antiviral medications may or may not be effective for infection. As viruses have the potential to mutate rapidly, much faster than bacteria or fungi, this presents a therapeutic challenge for the clinician, as treatment with antiviral medications may start to fail. The most noteworthy is HIV antiretroviral (ARV) resistance, which confers a great deal of risk to the patient if the medications stop working.
Sequence analysis is performed most commonly at the genomic level, which looks directly at the HIV genome to see to which antiretroviral drugs that strain of HIV is already resistant and therefore which drugs will not work. Less commonly, this analysis is performed at the phenotypic level, where the patient's HIV virus is subjected to antiretroviral medication in the laboratory to see how well it responds.