What are marine stings?
Marine stings include venomous or contact stings from any marine creature.
The main culprits causing contact stings are jellyfish and jellylike animals, fire coral, sponges, hydroids, and sea anemones; while penetrating injuries are caused by sea urchins, cone shells, and venomous fish. Venomous fish include stingrays, stonefish and zebrafish, lionfish and scorpionfish, and catfish.
Who gets marine stings?
Marine wounds and stings occur amongst fishermen, swimmers, scuba divers, surfers, and aquaculture workers.
Jellyfish are most prevalent in calm warm seawater, sandy beaches, and harbours during the summer months, although they are also seen in other circumstances. Sea anemones, fire coral, sea urchins, sponges, and venomous fish are also commonly found in shallow coastal waters, as well as reefs.
What causes marine stings and wounds?
Jellyfish stings
Jellyfish cause the majority of marine stings.
- Bluebottles (Physalia species) are the most common cause of jellyfish stings worldwide.
- Chironex fleckeri (the Pacific box jellyfish or sea wasp, with long tentacles) and Carukia barnesi (the Irukandji jellyfish) are typically found in northern Australian and Indo-Pacific waters and are the most venomous.
- Physalia physalis (also known as the Portuguese man o’ war) is found in the southern Atlantic, while Physalia utriculus is common in the Pacific and on the east coast of Australia and New Zealand.
- Pelagia noctiluca (Mauve stinger) is a widespread offshore species that can also wash ashore in large numbers.
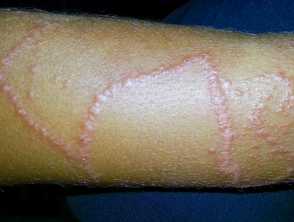
Jellyfish stings occur when their tentacles contact human skin. Nematocysts (cells that line the jellyfish tentacles) fire poison-filled darts as they touch the skin. The severity of the sting depends on the amount of tentacle contact and the type of venom.
Other marine stings
Corals, sea anemones, and hydroids also use nematocysts to sting, typically producing intense and sustained local skin reactions, characterised by burning pain.
Venomous fish, stingrays, and sea urchins all have venomous spines in their dorsum, ventral surface, or tail which can inject venom as they penetrate human skin. The venom typically stings more than the penetrating wound and effects are typically local, although very painful.
Sponges use structural elements in their skeleton called spicules to form small perforations from which chemicals or toxins can be extruded into human skin. Irritant or allergic contact reactions typically result (‘sponge dermatitis’).
When picked up or handled, blue-ringed octopus and cone shells envenomate via a bite (sometimes painless) and a dart-like apparatus respectively, delivering tetrodotoxin and conotoxins (nerve channel toxins).
Other marine injuries
Cuts and scratches among fishermen, swimmers, and surfers often fail to heal, which may relate to repeated exposure to seawater and foreign material such as sand in the wound.
What are the clinical features of marine stings and wounds?
Clinical features of marine stings include:
- Pain, paraesthesia, erythema, itch, swelling, or bleeding on or near the affected area on immediate contact
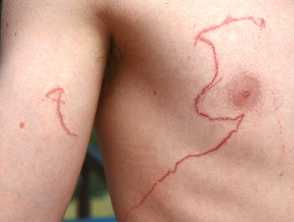
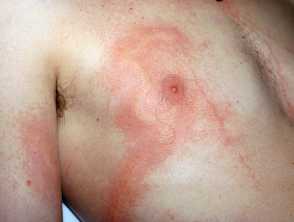
- Brown/purple beaded, linear, or whip-like patterned welts (jellyfish)
- C. fleckeri produces immediate brownish or purplish wheals 8–10 mm wide with cross striations, followed by vesiculation and areas of necrosis
- Bluebottle stings produce chains of oval wheals surrounded by erythema that persist for about 24 hours.
- ‘Caterpillar’ track mark or ‘goose pimples’ (Irukandji)
- Blisters (may form within minutes)
- Sweating (Irukandji)
- Nausea or vomiting, diarrhoea
- Muscle pain and cramps (especially Irukandji)
- Progressive muscle paralysis and respiratory failure (sea snake, blue-ringed octopus, cone shells)
- Rarely: weakness, faintness, dizziness, or difficulty breathing (box and Irukandji jellyfish).
Irukandji leaves a small erythematous area or scarcely any skin marks, a diagnostic clue in itself. Irukandji syndrome may be delayed (20–30 mins) with severe generalised cramping pain and systemic effects (tachycardia, agitation, hypertension, and pulmonary oedema) and is potentially lethal.
Stonefish produce a single severely painful foot puncture with rapid surrounding oedema, in a tropical coral reef setting and typically no sighting of what caused the injury. Sea urchin and stingray injuries also typically involve the foot or ankle.
Other marine injuries (eg, cuts and scratches) are most often located on the feet, ankles, and back of the hands. They are often slow to heal and may be called ‘sea ulcers’. Peripheral callus formation may occur, similar to diabetic foot ulcer (even in non-diabetics).
How do clinical features vary in differing types of skin?
Darker Fitzpatrick skin types may be more prone to keloid and hypertrophic scarring following injury.
What are the complications of marine stings?
Potential complications of marine stings include:
- Anaphylaxis
- Delayed skin reactions
- Wound infections — secondary infection risk in penetrating wounds:
- Staphylococcus aureus is the most common source of wound infection and results in impetiginisation and cellulitis
- Vibrio vulnificus infection is peculiar to marine injuries and may cause rapidly progressive cellulitis and death
- Mycobacterium marinum is an atypical mycobacterium found in tropical waters, and can cause chronic infected ulcers or plaques.
- Localised neuropathy
- Keloids
- Granulomas
- Hyperpigmentation
- Fat atrophy
- Muscle contractures
- Irukandji syndrome, which mimics excessive catecholamine release
- Skin necrosis (Irukandji)
- Compartment syndrome (all jellyfish)
- Digital ischaemia (all jellyfish)
- Retained foreign bodies (venomous fish or sea urchins)
- Synovitis/tenosynovitis (sea urchins)
- Arthropathy and bursitis (sea urchins)
- Osteomyelitis (sea urchins)
- Death (can sometimes occur with stings from box or Irukandji jellyfish, deep penetrating stingray spines to thoraco-abdominal cavities, sea snakes, blue-ringed octopus, or cone shells).
- Box jellyfish fatalities are more common in children.
How are marine stings diagnosed?
Diagnosis of marine stings relies on the sighting of the creature, historical clues, and clinical features. Enquire if the animal (or pieces of it) was obtained, or if photographs were taken. All significant jellyfish and spiny fish envenomations produce immediate and severe pain.
Dermoscopy may be used to identify the type of jellyfish sting with a peculiar finding of ‘serpentine ulceration’ with brown dots indicative of a P. noctiluca sting.
A definitive diagnosis of the jellyfish type can be made using sticky tape or a skin scraping to identify the characteristic nematocysts in the keratin layer. Skin scrapings are placed in a formalin solution (1–4%) and then examined under a microscope at x40 objective.
What is the differential diagnosis for marine stings?
- Marine bites (eg, blue-ringed octopus)
- Trauma
- Sea bather’s eruption
- Seaweed dermatitis
- Swimmer’s itch
What is the treatment for marine stings and wounds?
General measures
- Resuscitation for patients who are unconscious or have cardiovascular collapse (usually caused by box or Irukandji jellyfish, or cone shells).
- Analgesia (ice packs, simple analgesics) and local pressure for bleeding.
- Topical corticosteroid creams and/or antihistamines may be used for itch and burning discomfort.
- To prevent infection: early wound irrigation, debridement, and the removal of any foreign body with the exception of stingray wounds. Any thoracic, cervical, or vascular penetrating wound from venomous fish requires urgent medical attention.
- Prophylactic antibiotics remain controversial but are suggested for large penetrating wounds and those with significant comorbidities or who are immunocompromised.
Toxicology advice can be obtained from local poison advisories (eg, the Australian Poisons Information Centre). Antivenoms exist for box jellyfish, stonefish, and sea snake envenomation.
Specific measures
Major box jellyfish (Chironex fleckeri)
- Apply vinegar (5% acetic acid) immediately and liberally for at least 30 seconds to inactivate nematocysts.
- Remove any tentacles using your fingertips or gloves after inactivation.
- Consider antivenom in patients with potential cardiovascular collapse not responsive to standard advanced life support, uncontrolled pain or potential severe scarring.
- Cardiac monitoring is advised.
- Urine and alcohol can exacerbate injury and are not recommended.
- Ice packs may be used for pain, along with oral or parenteral analgesia.
Irukandji box jellyfish (Carukia barnesi)
- Apply vinegar (5% acetic acid) immediately for at least 30 seconds.
- Remove any tentacles using your fingertips or gloves.
- If vinegar is not available, wash the area with seawater.
- Hospital admission may be required for titrated analgesia, antiemetics, benzodiazepines and management of hypertension.
- Cardiac monitoring is advised.
- The use of magnesium in Irukandji syndrome is anecdotal and remains unproven.
Bluebottle and other jellyfish (Physalia spp)
- Wash the sting site with seawater (not vinegar).
- Remove any tentacles if present.
- Immerse in hot water (42–45ºC) for 30–90 minutes or until pain resolves. A hot shower may be used and repeated for 20-minute intervals for up to 2 hours for widespread stings.
- Jellyfish sting inhibitors in sunscreen lotions have been shown to lessen symptoms.
Venomous fish and stingrays
- Carefully remove visible spines unless it is a stingray wound.
- Wash the wound site and immerse in hot water (42–45ºC) for 30–90 minutes or until pain resolves.
- Debridement is often needed: surgical consultation is recommended for spines embedded near joints, tendons, or neurovascular structures, and deep truncal wounds.
- X-ray the wound to exclude retained spiny material.
- Consider stonefish antivenom for stonefish stings with severe pain or systemic effects.
- Tetanus prophylaxis should be considered.
- Review wound for up to a week for secondary infection and need for antibiotics (Vibrio spp in salt water and Aeromonas spp in fresh water).
Sea urchins
- Treatment is aimed at removing as many visible spines as possible.
- Wash the wound site and immerse in hot water (42–45ºC) for 30–90 minutes or until pain resolves (typically not severely painful).
- Vinegar or weak acids can be used to dissolve small spine fragments, mainly composed of calcium carbonate (some island cultures use lime juice).
- Most spines come out by themselves within a few weeks.
- X-ray or ultrasound can be used to identify retained spines.
- Tetanus prophylaxis should be considered.
Corals and sea anemones
- Remove visible debris.
- Wash the wound site and immerse in hot water (42–45ºC) for 30–90 minutes or until pain resolves.
- Vinegar may also be used in coral stings.
- Topical steroids may be used.
- Tetanus prophylaxis is recommended.
Cone shells and blue-ringed octopus
- Monitor airway and pulse and provide CPR if necessary. Generalised paralysis may necessitate mechanical ventilation.
- Immobilise affected area in a dependent position (hanging down).
- Compression bandaging (remove only in hospital).
- Wash the wound site and immerse in hot water (42–45ºC) for 30–90 minutes or until pain resolves.
- Tetanus prophylaxis is advised.
Sponges
- Remove spicules using adhesive tape.
- Clean the wound thoroughly.
- Topical corticosteroids
- Tetanus prophylaxis should be considered.
Sea ulcers
- Sea ulcers should be kept scrupulously clean, dry, and protected from further injury.
How do you prevent marine stings?
- Swim in areas patrolled by lifeguards.
- Pay attention to signs warning of danger from hazardous marine life.
- Avoid touching unfamiliar sea creatures without gloves (including dried sponges).
- Wear protective footwear on submerged rocks or reefs.
- Remain cautious in murky water.
- A full-body lycra ‘stinger suit’ can prevent some jellyfish stings.
What is the outcome for marine stings?
Most marine stings are minor and do not require any medical intervention. Some bites and stings can result in serious tissue damage, penetrating injury, and systemic toxicity.
Death from a marine sting is rare and is largely due to cardiac arrhythmias caused from the toxins released by the box jellyfish, Irukandji jellyfish, or a major stingray trauma. Rare deaths have occurred from sea snake, cone shell, and blue-ringed octopus envenomation, which may cause paralysis and respiratory failure.
Marine stings rarely cause permanent scarring. Hyperpigmentation or hypopigmentation can remain for up to two months. Consider tetanus prophylaxis and treatment of secondary infection.