What happens to my biopsy sample?
Once your skin biopsy sample reaches the lab, it goes through a complex series of steps so a report can be created for your doctor.
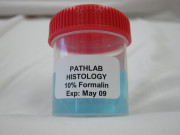
| Formal saline to fix specimen | Wax block to harden specimen | Microtome to cut thin sections | Picking up sections |
|---|---|---|---|
 |
 |
 |
 |
| The sample arrives in a specimen pot filled with formal saline, where it remains for 24 hours to preserve the tissue. | The sample is carefully sliced into small pieces before fixation. This is a process in which the tissue is dehydrated overnight. The fixed tissue is then placed in a hot-wax block, cooled to solidify the wax. | Using a microtome, it is carefully cut into very thin wafers (‘sections’), which are about 5 microns thick. | The sections are floated on a warm water bath. They are picked up onto glass slides, dried, and put through a series of stains to produce the tissue slides that can be interpreted under the microscope. |
As you can tell, this process is very labour intensive, which is why a pathology report can take a number of days to produce.
Once the slides are ready for your pathologist to look at under the microscope, there is still a lot of work to be done. Making the correct diagnosis can sometimes require special stains, which can take a further day or more to produce. The pathologist may also like to discuss cases with their colleagues or a melanoma specialist if there is any doubt about the diagnosis.
The pathology report
Once the tissue has been studied, a report is typed up and sent to your doctor. This is usually sent rapidly using a secure electronic process.
What is a synoptic report?
Although some pathologists simply describe a melanoma in their own words, synoptic reports are more common. These are standardised to include a list of melanoma features and whether they are present. For example:
- Specimen type
- Procedure eg excision or re-excision
- Site and side of the body where lesion located
- Melanoma subtype
- Excision margin (lateral and deep)
- Size of the tumour
- In situ or invasive tumour
- Maximum Breslow thickness
- Presence of ulceration
- Presence of mitoses (dividing cells)
- Invasion of blood and lymph vessels
- Invasion of nerve bundles
- Signs of regression
- Pre-existing melanocytic naevus (mole)
- Tumour pathological stage (T score)
- Free text area for comments
Clinicians find synoptic reporting very helpful when planning further treatment for patients with melanoma.
What is staging?
Once your pathologist has decided that the specimen is a melanoma, it needs to be carefully re-examined to determine features that would class it as a good or bad type of melanoma.
There are three features of melanoma that are important for pathological staging:
- Breslow depth
- Ulceration
- The number of mitoses
These make up the T score of staging. The pathology report, clinical examination of your lymph nodes, and the results of other investigations are used to describe the final clinical stage.
What is Breslow depth?
The Breslow depth is the most important feature of a melanoma for determining outcome. The Breslow depth is a measurement made from the granular layer of the epidermis, the top layer of the skin, to the deepest part of the melanoma, and is measured in millimetres.
As a melanoma becomes thicker, the outcome for that melanoma becomes worse. Staging is divided into groups based on measurements of Breslow thickness less than 1 mm, 2–4 mm and more than 4 mm.