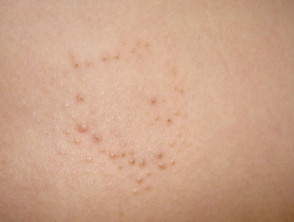
What is phrynoderma?
Phrynoderma is a form of follicular hyperkeratosis associated with nutritional deficiency.
Follicular hyperkeratosis
Who gets phrynoderma?
Phrynoderma is most often reported in children living in poverty in Africa and Asia.
A dietary history may reveal:
- Prolonged history of poor dietary intake in the past 1–2 years
- Lack of vegetables, fruit and fat in the diet.
Phrynoderma is rare in developed countries, when it is most often associated with:
- Intestinal malabsorption
- Anorexia nervosa
- Fad diets
- Previous bariatric surgery or small bowel bypass surgery
- A history of alcoholism.
Phrynoderma is associated with other chronic illnesses, such as pancreatic insufficiency, inflammatory bowel disease, and gallbladder disease [1–3].
What causes phrynoderma?
Phrynoderma is associated with nutritional deficiency, particularly [1,4]:
- Vitamin A deficiency (commonly)
- Severe malnutrition
- Vitamin E and B deficiency
- Essential fatty acid deficiency.
What are the clinical features of phrynoderma?
Phrynoderma is a form of asymptomatic or mildly symptomatic follicular hyperkeratosis, where follicular papules of various sizes with central keratotic plugs that block the follicle openings develop on the skin [1]. New patches may be hypopigmented [3,4].
Patches initially arise on the back of the elbows and the front of the knees, and can spread to involve the extremities, upper forearms and thighs.
Occasionally patches will also appear on the abdomen, back and buttocks. The face is rarely affected, and hands and feet are spared [1].
Other symptoms of vitamin A deficiency can be present, such as:
- Night blindness
- Inability to see in bright light.
Features of severe vitamin A deficiency can include [2]:
- Xerophthalmia (dryness of the conjunctiva and cornea of the eye with inflammation and ridge formation)
- Bitot spots (grey-white patches on the conjunctivae)
- Keratomalacia (drying and clouding of the cornea) that can lead to blindness
- Delayed growth
- Intellectual disability.
What are the complications of phrynoderma?
Phrynoderma may result in persistent hyperpigmentation or scarring.
How is phrynoderma diagnosed?
In the right context, phrynoderma may be suspected by its characteristic clinical features. If a skin biopsy is performed, histological features may include:
- Enlarged hair follicles containing keratin plugs
- Lamellated hyperkeratosis next to the hair follicles
- Atrophy of the sebaceous glands
- Keratinising metaplasia of epithelial surfaces
- Squamous metaplasia of eccrine and sebaceous glands, in severe disease [1,2].
The level of vitamin A in the blood of patients with phrynoderma may be either low (< 30 μg/100 mL) or normal. These vitamin A levels may not reflect a clinically apparent deficiency, as stores may last up to a year in adults [1]. Severe malnutrition is also associated with reduced albumin levels.
The diagnosis of phrynoderma is supported if the signs resolve with better nutrition [4].
What is the differential diagnosis of phrynoderma?
Several other conditions are characterised by follicular hyperkeratosis. These conditions include:
- Keratosis pilaris (small horny plugs blocking the hair follicles on the outer arms and thighs of healthy individuals)
- Darier disease (scaly papules affecting the hands and seborrhoeic areas, including the forehead, scalp, nasolabial folds [the laugh lines], ears and chest).
- Lichen spinulosus (an acute eruption of grouped keratotic papules)
- Keratosis circumscripta (a follicular form of ichthyosis).
What is the treatment for phrynoderma?
Patients with phrynoderma can be assessed by a nutritionist, dietician, ophthalmologist, dermatologist, gastroenterologist and/or a general physician.
Nutritional management may include:
- Vitamin A replacement (50,000–150,000 U/day for 1–4 months [1])
- Vitamin A-rich foods (eg, liver, carrot, spinach, egg yolk)
- Supplemental linoleic acid using safflower or linseed oil (2 tbsp, twice daily)
- Other supplementation according to the results of dietary assessment.
Topical keratolytic agents can be applied to the scaly plaques for symptomatic relief. These agents can include:
- Salicylic acid ointment
- Tretinoin gel or cream
- Urea cream.
What is the outcome of phrynoderma?
Skin lesions can take 1–4 months to resolve with restoration of nutrition. Topical keratolytic medicines can provide temporary relief [3,4].
Vitamin A deficiency can cause ocular disturbance, but this generally resolves within days of starting therapy, unless scarring has occurred. If left untreated, there can be permanent scarring of the conjunctiva and cornea [3,4].