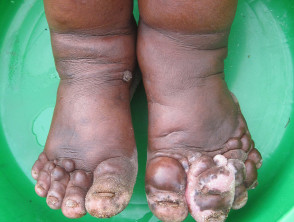
What is podoconiosis?
Podoconiosis is a form of lymphoedema that affects the lower limbs and occurs in people with long-term exposure to volcanic red clay soil.
Podoconiosis
Fasil Ayele, National Institutes of Health, via Wikimedia Commons
Who gets podoconiosis?
Podoconiosis is endemic in tropical regions of Africa, Asia and Central America.
- Podoconiosis is present in communities living at high altitude (above 1000 m) where there are volcanic red clay soils.
- Long-term exposure occurs in rural communities where genetically susceptible individuals are most likely to be exposed in the home and through their occupation.
- Symptom onset begins in the first 10–20 years of constant exposure, with a progressive increase in prevalence being seen up to 60 years of age [1].
What causes podoconiosis?
Podoconiosis is a genetically determined abnormal inflammatory reaction to mineral particles derived from volcanic deposits in red clay soils. The suggested pathogenesis is [1]:
- Absorption of soil particles through fissures in the sole of the foot
- Lymphocytic reaction to the particles
- Subsequent oedema (fluid build-up) and fibrosis
- Enlargement and stiffening of the vessels, causing valvular dysfunction
- Attachment of the dermis and subdermis to the deep fascia
- Narrowing and obliteration of the lymphatic vessels
- Destruction of the hair follicles, sweat and sebaceous glands.
No contagious or infectious organism has been identified.
What are the clinical features of podoconiosis?
Cutaneous symptoms and signs associated with podoconiosis include [1–3]:
- Lichenification and stiffness in the web space (the interdigital soft tissue extending from the base of toes to the metatarsophalangeal joints) between the first and second toes
- Dermal nodules — elevated, non-translucent lesions 0.5 cm in width and length
- Dermal ridges — elevated lesions 0.5 cm in width, longer in length than in width
- Dermal bands — unelevated palpable ridges
- Longitudinal skin markings — these are most striking between first and second toes, exaggerated by scrunching
- Serous ooze
- Mossy changes leading to a rough velvety skin surface with round or fusiform, fluid-filled or papillomatous, hyperkeratotic horny lesions in a slipper pattern around the heel and border of foot
- Pruritus and/or a burning sensation over the foot and lower limb
- Swelling of the foot and lower limb
- Increased diameter of the leg
- Block toes and splaying of the forefoot, which cause the big toes to knock together.
Lichenification of the web space can be identified for using a lymphoedema test called Stemmer sign. This involves pinching and lifting on the skin on the upper surface of the second toe; if the skin is pinched but not lifted, the test is positive
Podoconiosis is a chronic condition that is commonly complicated by acute episodes of lymphadenitis, especially when fibrotic. Acute lymphadenitis presents as:
- Fever
- Pain in the limb
- Warmth of the limb
- Tender femoral lymph nodes
- A further increase in the size of the limb.
Podoconiosis presents with ascending lymphoedema.
- Lymphoedema is commonly bilateral, but can sometimes be asymmetrical.
- Lymphoedema begins in the foot, progressing proximally up the lower limb. It usually stops before the groin.
- Swelling can take two forms: either a soft and fluid, ‘water-bag’ type or a hard and fibrotic ‘leathery’ type often associated with multiple hard skin nodules.
Podoconiosis has an early prodromal phase prior to the development of elephantiasis.
Acute attacks resolve spontaneously after a few days of rest and elevation. Subsequent episodes typically affect the same limb. Patients have an acute attack on average five times a year [1,2].
Podoconiosis staging
The following staging system was designed for use by field workers [3]. Each leg should be staged separately for the:
- Presence (M+) or absence (M-) of mossy changes
- Greatest below-knee circumference.
Stage 1: Swelling reversible overnight
The swelling is not present when the patient first gets up in the morning.
Stage 2: Below-knee swelling that is not completely reversible overnight; if present, knobs or bumps are below the knee ONLY
- Dermal knobs or bumps appear in form of nodules, ridges or bands.
- Tourniquet-like effects are observable at this stage, depending on the position of dermal ridges and nodules in relation to joints.
- Mossy changes may be apparent, but their presence depends on a range of factors, such as the use of plastic footwear.
- Nail dystrophy may develop.
- Interdigital maceration and hyperpigmentation are often present.
Stage 3: Below-knee swelling that is not completely reversible overnight; knobs or lumps present above the ankle
- Persistent swelling is seen that does not reach above the knee.
- Dermal nodules, ridges or bands appear above the ankle.
- Tourniquet-like effects are frequently observed at this stage.
- Features mentioned in Stage 2 may also be present.
Stage 4: Above-knee swelling that is not completely reversible overnight; knobs or lumps present at any location
- Persistent swelling reaches above the knee.
- Lymphangiectasia may be apparent, particularly on the thigh.
- Features mentioned in Stage 2 may also be present.
Stage 5: Joint fixation; swelling at any place in the foot or leg
- The ankle or interphalangeal joints become fixed and difficult to flex and dorsiflex.
- This joint fixation may be accompanied by adhesion of the web spaces between the toes, making the toes appear short or indistinct.
- Sensation is preserved.
- X-rays show tuft resorption (short of the ends of the toes) and loss of bone density.
What are the complications of podoconiosis?
Complications of podoconiosis include:
- Secondary bacterial infection
- Loss of work
- Social isolation.
How is podoconiosis diagnosed?
Podoconiosis is diagnosed clinically. Diagnosis is based on clinical features, a careful patient history and the exclusion of other causes of lymphadenitis.
What is the differential diagnosis for podoconiosis?
The differential diagnosis includes other causes for elephantiasis, such as:
- Lymphatic filariasis is found at lower altitudes — swelling is often first noticed in the groin and then descends. It is usually unilateral and stops above the knee
- Lymphoedema due to leprosy — sensation is lost from the heel but preserved in the toes and forefoot; trophic ulcers, thickened nerves or hand involvement may be observed
- Endemic Kaposi sarcoma
- Chronic recurrent erysipelas
- Mycetoma
- Elephantiasis nostras verrucosa (form of chronic lymphoedema).
What is the treatment for podoconiosis?
Podoconiosis treatment aims to reduce lymphoedema and to prevent relapse by reducing re-exposure to the causative soil.
Primary prevention requires avoiding prolonged contact between the skin and the soil. This includes:
- Wearing covered footwear
- Having floor coverings in homes.
Treatment after podoconiosis has occurred involves:
- Foot hygiene
- Covered footwear
- Compression bandaging
- Relocation of living and working environments
- Emollient to improve skin barrier function.
More severe disease may require [1, 2]:
- Elevation for at least 18 hours per day
- Compression bandaging.
Surgical management has been attempted. Shave excision (using a blade to remove the top layers of the skin) of hard nodules has been used with secondary intention healing (where surgical wounds are left to heal by themselves). It should be noted that surgical removal of tissue followed by skin grafting (Charles operation) is unsuccessful, as scar tissue aggravates symptoms [1].
What is the outcome for podoconiosis?
Podoconiosis results in progressive swelling and disfigurement of the limbs. Untreated patients are typically in constant pain and discomfort and may suffer from chronic infections. As a result of social stigmatism, individuals with podoconiosis are often ostracised in their communities [1, 2].