What is elephantiasis nostras verrucosa?
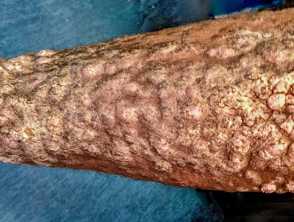
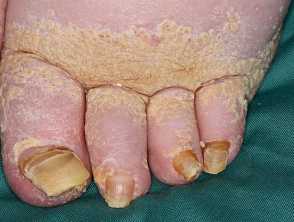
Elephantiasis nostras verrucosa (ENV) is a rare and severe form of chronic lymphoedema. It leads to cutaneous changes including scarring, non-pitting oedema, hyperkeratosis, cobblestone-like papules, and indurated plaques on gravity-dependent body parts.
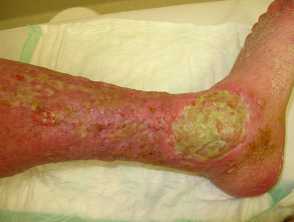
ENV predominantly affects the lower legs in a symmetrical fashion. Other sites that may be affected include the proximal thighs, abdomen, amputation stumps, and scrotum.
It is also known as lymphostatic verrucosis, elephantiasis crurum papillaris et verrucosa, ‘mossy leg’, lymphangitis recurrens elephantogenica, and lymphostatic papillomatosis cutis. ‘Nostras’ is a term used to describe the non-filiarial form of elephantiasis.
Who gets elephantiasis nostra verrucosa?
Elephantiasis nostras verrucosa is rare and can occur in males and females of all races.
It is associated with obesity and recurrent soft tissue infections. Other risk factors include malignancy, congestive heart failure, chronic venous insufficiency, previous trauma, hypothyroidism, and radiation.
What causes elephantiasis nostra verrucosa?
Elephantiasis nostras verrucosa is caused by chronic lymphostasis, which results in protein accumulation within the interstitial fluid, inducing fibroblast proliferation. This is thought to cause progressive fibrosis of the lymphatic drainage system, leading to obstruction. As the condition progresses, ulcers may develop, leading to recurrent secondary infection.
Conditions which cause impaired lymphatic drainage and can lead to ENV include:
- Obesity
- Congestive heart failure
- Deep vein thrombosis
- Hypothyroidism
- Lipodermatosclerosis
- Diabetes
- Infections (cellulitis and filariasis)
- Malignancies (such as lymphoma)
- Prior surgery or trauma
- Radiation therapy
- Milroy’s disease (congenital lymphoedema).
What are the clinical features of elephantiasis nostras verrucosa?
- Non-pitting oedema (positive Kaposi-Stemmer sign)
- Grossly enlarged and disfigured appendages
- Hyperkeratosis of the epidermis
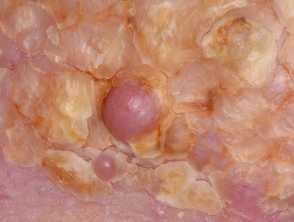
- Papillomatous lesions and verrucous growths (‘cobblestone’ appearance)
- ‘Woody’ or ‘mossy’ textured skin
- Overlying ulcerations and crusts.
How do clinical features vary in differing types of skin?
Striking white bright plaques and depigmentation have been reported in Fitzpatrick skin type VI. This is speculated to result from impaired melanogenesis due to chronic inflammation associated with lymphoedema.
What are the complications of elephantiasis nostra verrucosa?
- Lymphorrhoea (lymph leakage from the skin)
- Chronic skin infections
- Ulceration
- Poor wound healing
- If untreated, can lead to scarring or limb disfigurement
- Cellulitis +/- septicaemia
- Squamous cell carcinoma.
How is elephantiasis nostra verrucosa diagnosed?
Diagnosis is often made clinically, excluding other causes of lymphoedema on history and examination.
Patients often reveal a long history of oedema prior to the onset of fibrosis, hyperkeratosis, papules, and verrucous lesions. Recent travel, time course, and onset may differentiate from other causes such as filariasis.
Kaposi-Stemmer sign (an inability to pinch the skin overlying the base of the second toe) is indicative of lymphoedema.
Investigations
- Bloods: full blood count, Giemsa-stained blood smear, and/or specific antigen testing may help rule out filariasis.
- Biopsy may prove useful in excluding secondary malignancy but is often not necessary for diagnosis. Histology of ENV commonly shows acanthosis, papillomatosis, loss of adnexal structures, and progressive fibrosis.
- Imaging studies such as CT, MRI, lymphoscintigraphy, and lymphangiography may prove useful in determining the degree and cause of lymphoedema.
What is the differential diagnosis for elephantiasis nostras verrucosa?
- Filarial lymphoedema
- Lipodermatosclerosis
- Chromoblastomycosis
- Familial lipoedema
- Papillomatosis cutis carcinoides
- Papillomatosis cutis lymphostatica
- Lymphangiosarcoma (Stewart-Treves syndrome)
- Podoconiosis
- Mycetoma
- Lipoedema
- Pretibial myxoedema
- Venous stasis dermatitis
- Deep vein thrombosis
- Cellulitis
- Lymphoedema due to leprosy
- Endemic Kaposi sarcoma
What is the treatment for elephantiasis nostras verrucosa?
Elephantiasis nostras verrucosa is difficult to treat with no known cure. The underlying cause should be treated to prevent further complications. Treatment of ENV can be conservative, medical, or surgical, depending on the severity and deformity.
Conservative treatment
- Compression stockings or compression pneumatic devices.
- Toe caps.
- Lymphatic massage.
- General skin care measures (eg, soap-free wash, daily emollients and moisturisers, and prompt treatment of cuts/grazes).
- Weight loss for overweight patients.
- Good control of blood sugar levels in diabetic patients.
Medical treatment
Consider:
- Systemic or topical retinoids
- Keratolytics (eg, urea, lactic acid, salicylic acid)
- Deodorant powders to manage malodour
- Antibiotics — widely used in treating ENV, however, there is a lack of evidence for their efficacy in chronic infections
- Antimicrobial preparations such as triclosan, acetic acid, and bleach baths — may prove useful in the prevention of secondary infections.
Surgical treatment
Surgical treatment may be indicated when fibrosis or nodules occur. Techniques of shaving, excision, and electrocauterisation can be used, however, the risk of scarring, infection, and non-healing ulcers should be considered.
Several case reports have found that ablative carbon dioxide laser is well tolerated and provides cosmetic and symptomatic benefits to ENV patients.
How do you prevent elephantiasis nostras verrucosa?
Prevention of ENV relies on early management of lymphoedema through proper local hygiene, regular moisturiser, compression, lymphatic massage, weight loss, and exercise.
What is the outcome for elephantiasis nostras verrucosa?
Elephantiasis nostras verrucosa can result in progressive deformity of the limbs and reduced quality of life when the condition becomes debilitating.
Patients with ENV are at increased risk of malignancies such as squamous cell carcinoma, and angiosarcomas (Stewart-Treves syndrome), and should therefore be followed up to monitor for further complications.