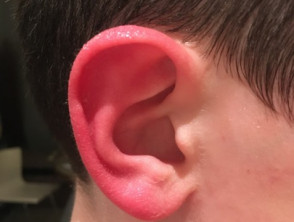
What is red ear syndrome?
Red ear syndrome (RES) is an uncommon disorder that presents with intermittent attacks of pain and reddening of one or both ears.
Who gets red ear syndrome?
Red ear syndrome affects all age groups with a median age of onset of 44 years (range 4–92 years). In children there is a male predominance of 2:1 in reported cases, compared to a slight female predominance in adults (1.25:1). Studies in children and adolescents presenting with migraines to a neuropsychiatry clinic found 20–25% had red ear syndrome on specific questioning, suggesting it is more common than the 100+ reported cases would indicate.
Red ear syndrome can be classified as either primary and secondary.
- Primary RES is more common in male children, and is often associated with migraines. It usually involves both ears. A subgroup of primary red ear syndrome may be a form of erythromelalgia.
- Secondary RES is more common in female adults, and is associated with cervical spinal nerve or temporomandibular joint dysfunction. It usually affects just one ear.
What causes red ear syndrome?
The pathogenesis of red ear syndrome is unknown and it is likely to be different in the two groups.
There are two theories as to how the syndrome can arise.
- Central theory: primary red ear syndrome is thought to be a trigeminal autonomic cephalalgia due to dysregulation in the brainstem.
- Peripheral theory: suggests secondary red ear syndrome is due to dysfunction or irritation in cervical spinal nerves (predominantly the C3 root).
What are the clinical features of red ear syndrome?
Red ear syndrome is characterised by paroxysmal episodes of pain and redness of one or both external ears. Redness can sometimes extend over the adjacent cheek. Unilateral ear involvement occurs in approximately 2/3 of cases, with the left ear more commonly involved than the right. Nearly one third report episodes are always bilateral. The pain is usually described as an annoying burning discomfort, but can be moderate to severe. Sometimes there is associated swelling of the ear with a feeling of fullness, and other symptoms such as redness or watering of the eye.
The frequency of episodes is variable, ranging from multiple episodes every day through to intermittent attacks that may occur in clusters every month or two. Daily episodes are reported by the majority.
The duration of an episode may last only seconds up to 4 hours, but typically lasts 30–60 minutes.
Episodes can be spontaneous or triggered. Triggers are more common with secondary red ear syndrome and include heat, touching or rubbing of the ear, hair brushing, teeth cleaning or grinding, or chewing. When associated with migraines, ear symptoms typically begin at the same time as the headache and resolve as the headache settles. However, the ear(s) may not redden with every migraine event.
Ear reddening can also occur as part of erythromelalgia, usually at the same time as the more typical hand and foot symptoms.
Primary erythromelalgia-type red ear syndrome in a child
What are the associations with red ear syndrome?
- Migraine
- Upper cervical spine pathology
- Temporomandibular joint dysfunction
- Erythromelalgia
- Palmoplantar erythrodysaesthesia (hand-foot syndrome)
How is red ear syndrome diagnosed?
Diagnostic criteria for red ear syndrome have been proposed:
A. Episodes of external ear pain lasting up to 4 hours
B. The ear pain has at least two of the following characteristics:
i. Burning quality
ii. Unilateral location
iii. Mild to moderate severity
iv. Triggered by cutaneous or thermal stimulation of the ear
C. The ear pain is accompanied by ipsilateral redness of the external ear
D. Attacks occur with a frequency of ≥1 per day, although cases with lower frequency may occur
E. At least 20 attacks fulfilling criteria A–D
F. Not attributed to another disorder.
Recommended investigations of red ear syndrome include:
- MRI of cervical spine and brain
- Orthodontic assessment of the temporomandibular joints.
What is the differential diagnosis for red ear syndrome?
- Relapsing polychondritis
- Contact dermatitis
- Cellulitis or perichondritis due to Staph aureus or Pseudomonas aeruginosa
- Chilblains
What is the treatment for red ear syndrome?
General measures
- Avoiding triggers
- Prevention/treatment of the headache
- Cooling the ear(s) during an acute attack.
Specific measures
Case reports have described many treatments such as indomethacin without consistent results. Gabapentin seems to be the most widely used treatment.
Red ear syndrome is usually refractory to treatment.
What is the outcome for red ear syndrome?
Red ear syndrome is usually a chronic condition. In some cases, the frequency of episodes may gradually decline with time.