Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: AJ Sykes, medical registrar, Auckland. . Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, June 2015.
Introduction Demographics Causes Clinical features Diagnosis Treatment Outcome
Sebopsoriasis is an overlap between two separate conditions: seborrhoeic dermatitis and psoriasis, in which features of both conditions co-exist. Sebopsoriasis can be thought of as a transitional condition between seborrhoeic dermatitis and psoriasis and has features of both conditions. The term is commonly used to describe a psoriasiform rash in a seborrhoeic distribution when the clinical features do not allow a precise diagnosis. Often it becomes clearer which condition the patient has with time and response to treatment
Sebopsoriasis can be seen across all age groups but is most common in childhood/adolescence and then increases in patients older than 50 years of age. The overall incidence is not known, as clear case definition is difficult.
Men are affected more often than women.
Like seborrhoeic dermatitis and psoriasis, the pathogenesis of sebopsoriasis is not fully understood.
Although the following factors are not present in the majority of patients with sebopsoriasis, they tend to be associated with more severe disease than in other patients without these risk factors:
Sebopsoriasis is characterised by:
Sebopsoriasis can also affect skin folds (intertrigo).
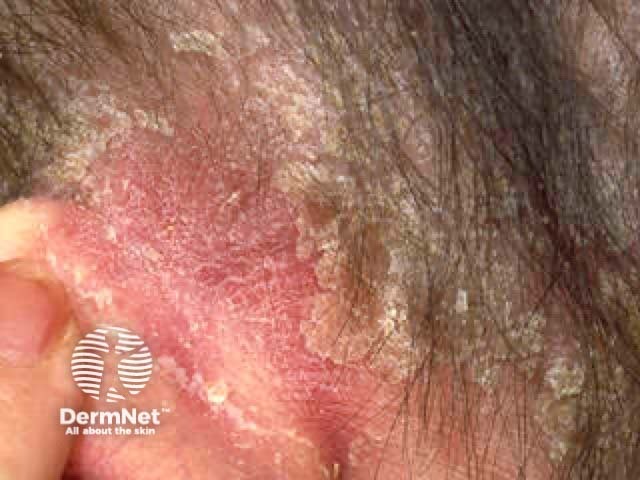
Sebopsoriasis affecting the retroauricular skin
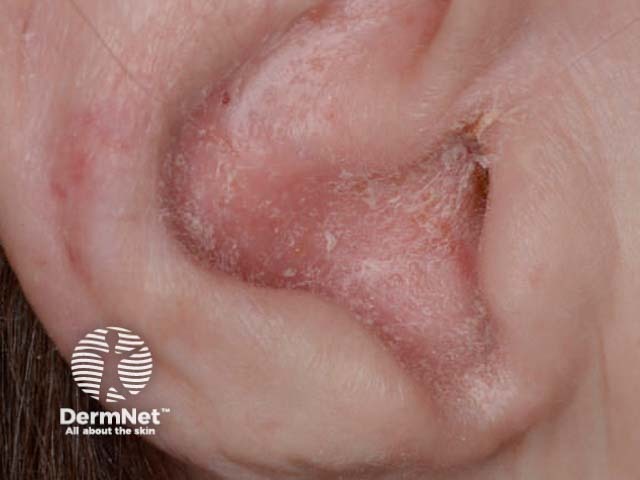
Sebopsoriasis of ear
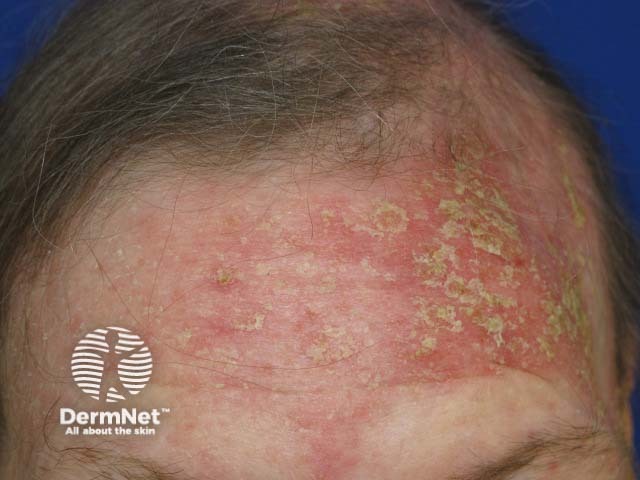
Sebopsoriasis of forehead
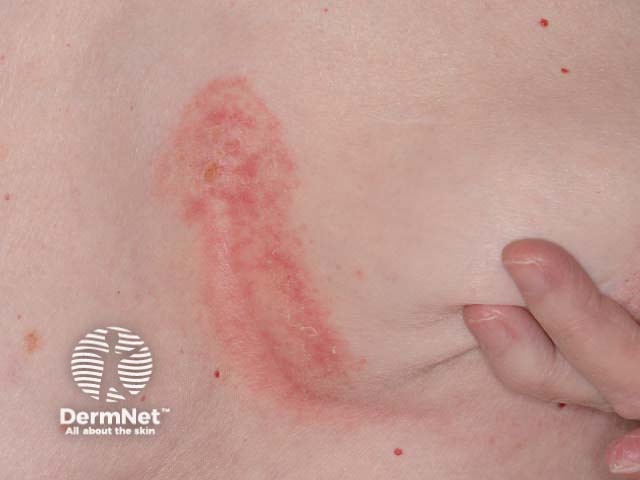
Sebopsoriasis of chest
Sebopsoriasis is diagnosed by its clinical appearance following a detailed history and examination. A skin scraping for mycology may reveal Malassezia, but this is not diagnostic, as the yeast is a normal component of skin flora (the microbiome).
Skin biopsy is rarely performed in sebopsoriasis. It shows histopathological features intermediate between psoriasis and seborrhoeic dermatitis.
The treatment for sebopsoriasis has overlap between the treatment for seborrhoeic dermatitis and that of psoriasis. Sometimes the response to treatment can help to determine if the patient is principally suffering from seborrhoeic dermatitis or psoriasis.
Topical calcineurin inhibitors Topical pimecrolimus cream or tacrolimus ointment may be helpful, especially if long term treatment is required and/or if there is concern about or presence of topical corticosteroid-induced side effects, for example, thin skin, easy bruising (purpura) or stretch marks.
There have been no long term studies looking at the outcomes of patients with sebopsoriasis. It is a chronic disorder that relapses and remits from time to time and may evolve into more typical psoriasis.