Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Background
Occurrence
Prevalence
Reactions
Diagnosis
Treatment
Moths and butterflies, and their larvae, caterpillars, belong to the order Lepidoptera. Although there are an estimated 125,000 to 150,000 different species in this order, very few are capable of causing adverse reactions in humans. Caterpillars are responsible for the vast majority of adverse reactions. Adult moths are less commonly implicated, and adult butterflies do not appear to be responsible for any adverse reactions in humans.

Bamboo caterpillars, which caused a rash on a gardener

Bamboo caterpillars, which caused a rash on a gardener
In most cases, adverse reactions to caterpillars and moths are mild and resolve spontaneously. Reactions from contact with caterpillars or moths can be classified based on the predominant symptoms.
Reactions to caterpillars and moths |
||
|---|---|---|
Type of reaction |
Clinical features |
|
Localised stinging reaction |
|
|
Papular urticaria and dermatitis |
Usually caused by hairs from caterpillars or moths. |
|
Urticarial weals |
|
|
Widespread haemorrhage (bleeding) |
|
|
Biting moths |
|
|
Ophthalmia nodosa |
|
|
Oral exposure |
|
|
Dendrolimiasis and pararamose |
|
|
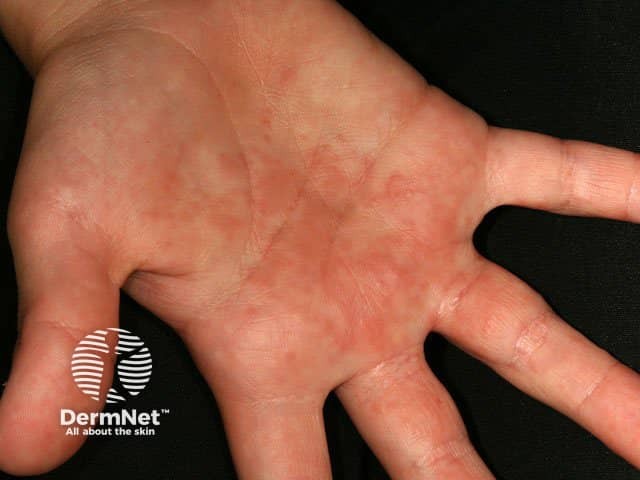
Hand irritation from contact with caterpillars
A diagnosis of a reaction to a caterpillar or moth is very difficult to make. The clinical features are non-specific and mimic those of many other insect bites, allergic reactions, and dermatological conditions. Features which may make the diagnosis more likely include:
Laboratory tests are generally not helpful.
General first aid measures include:
There is no specific treatment for most caterpillar and moth reactions (the only exception is the widespread haemorrhagic illness due to Lonomia caterpillars, for which there is an antivenom).