Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Susan Ford BSc (Hons) Occupational Health, 2012.
Introduction
Occupational rissk
Causes
Skin conditions associated with hairdressing
Workplace risk assessment
Health surveillance
Personal protective equipment
Hand care advice
Treatment
Occupational hand dermatitis in hairdressers was first described as early as 1898 and still today up to 70% of hairdressers suffer some form of skin damage during their career. Hand dermatitis in hairdressers is the second most commonly notified occupational skin disease in women.
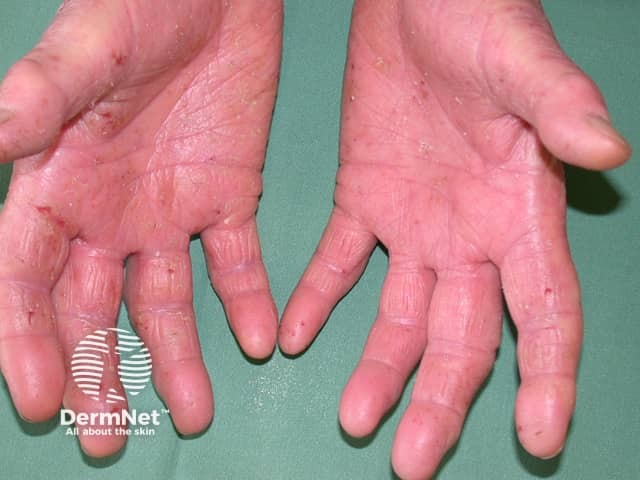
Hand dermatitis in hairdresser
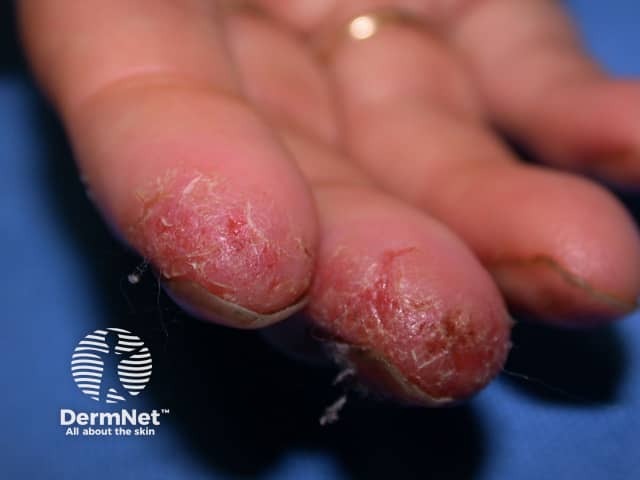
Hand dermatitis in hairdresser
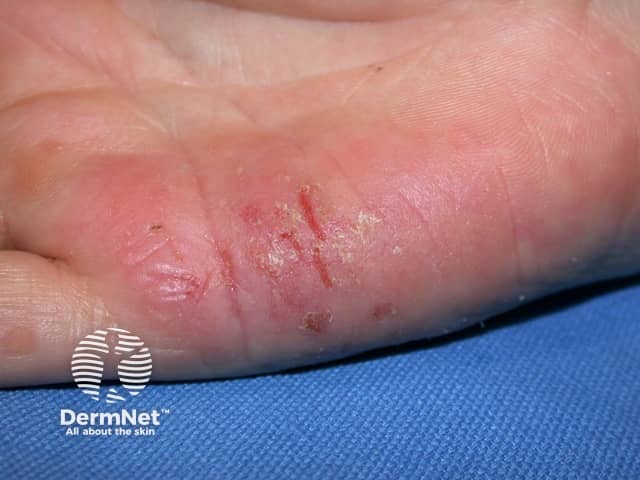
Hand dermatitis in hairdresser
Hand dermatitis in hairdressers and barbers is caused by three main factors.
Apprentices and juniors spend a lot of time at the basin, so are susceptible to occupationally related skin disease, especially if there is a history of eczema or asthma. An estimated 14–20% of students in the UK drop out of training in the first two years due to contact dermatitis.
Individuals with skin sensitivity and pre-existing atopic dermatitis at the pre-training/employment stage should consider whether hairdressing is a sensible career option. If they choose to proceed, they should take precautions throughout their career to reduce or avoid skin exposure to contact irritants and allergens.

Chemicals in a hairdressing salon

Shampooing in a salon

Applying colour in a salon
The outermost layer of the skin (the horny cell layer of the epidermis) acts as a barrier to prevent infection and to prevent potential allergens from penetrating the skin. Its pH is slightly acidic which can help to neutralise the degreasing agents that are in soaps, which are alkaline. Excessive use of soaps and some detergents can destroy the acidity and de-fat the surface skin and therefore the protection it offers.
If the moisture content is too high (overhydrated skin) or too low (dry skin), the skin barrier may also be less effective. Natural moisturising factors are diluted and may be washed out of the skin.
Irritant contact dermatitis occurs when physical or chemical damage to the barrier layer of the skin exceeds the skin’s ability to repair the damage. Examples include:
The features of irritant contact dermatitis are varied.
Allergic contact dermatitis is an immunological response to an allergen. Only people who are allergic to a specific agent (the allergen) will show symptoms. The appearance can be exactly the same as irritant contact dermatitis. There are some specific features of allergic contact dermatitis.
Nickel allergy is the most common form of allergic contact dermatitis in hairdressers and others.
The wearing of jewellery whilst at work should be discouraged, and any tools (eg, scissors) should be nickel-free.
Common examples of allergic contact dermatitis in hairdressers include:
Rubber gloves may also result in contact urticaria, which is due to rubber latex allergy.
Bacterial infection (impetigo, boils and folliculitis) is usually caused by Staphylococcus aureus and or Streptococcus pyogenes.
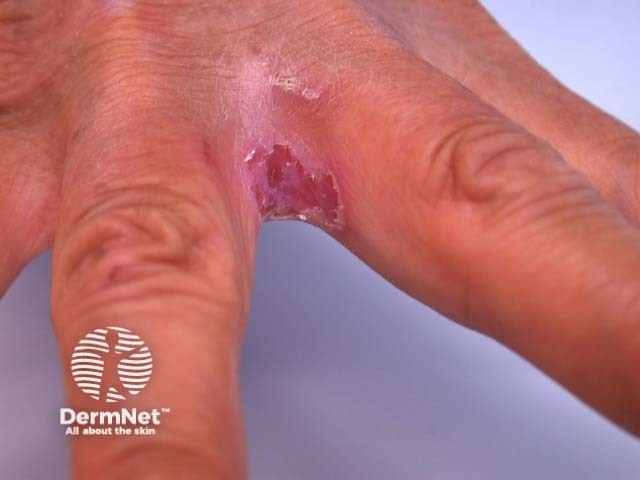
Hand dermatitis and wet work also predispose to yeast infection, usually presenting as chronic paronychia infected by Candida albicans or as intertrigo between the fingers (also called erosio interdigitalis blastomycetica).
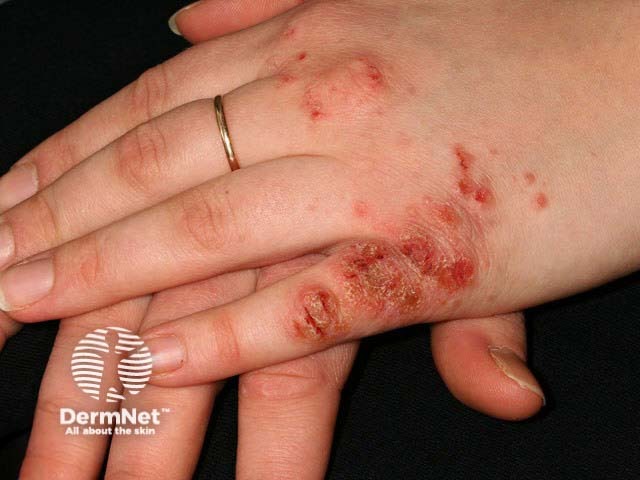
Infected hand dermatitis
Candida intertrigo
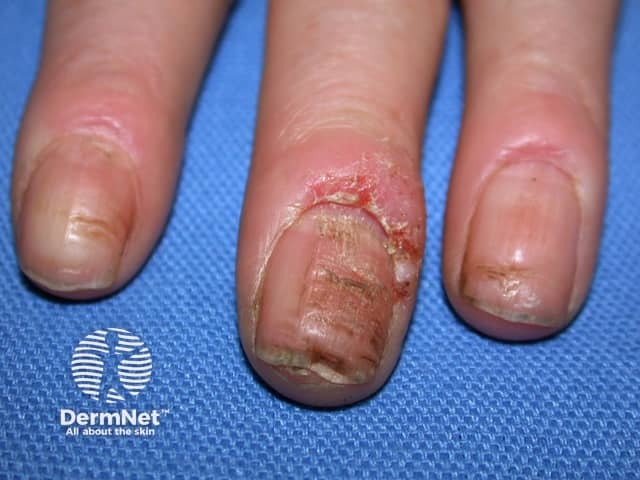
Paronychia
The shafts of a client’s hair can be as sharp as a needle and may penetrate the skin on the hands or under the fingernails, and occasionally other exposed sites. The foreign-body splinters may result in irritation, pain or infection.
Interdigital pilonidal sinuses ('pilus' meaning hair and 'nidal' meaning nest) are less common. They are typically found in the clefts between the fingers of hairdressers and barbers, where the skin is thin and moist. If the sinuses become infected, a pilonidal abscess may form.
Mechanical injuries may be caused by:
Scissor and razor wounds often affect the web between the index and middle fingers of the non-dominant hand (the comb hand). The risk can be reduced by holding the hair with the index and second fingers of the hand pressed together, one on top of the other. This closes the gap between the fingers.
Straightening irons and hair dryers cause thermal burns to the fingers and wrist of the non-dominant hand and repeated burn trauma over time can lead to scarring.
Workplace risk assessments identify ‘hazards’ (anything that has the potential to cause harm) and ‘risk’ (the likelihood of an event occurring). The aim should be to reduce these, as ill-health can adversely affect the quality of life, the ability to work in a chosen industry, insurance costs and litigation claims. A generic risk assessment in any hairdressing salon should include a specific section on skin exposure and should cover:
Results of the risk assessment must be recorded and kept.
Health surveillance should be carried out when a workplace hazard is minimised rather than eliminated Staff should be encouraged to report any signs of skin problems and all reasonable steps should be taken to resolve the problem and prevent recurrences. This may involve a referral for medical advice.
Follow the manufacturer’s recommendations for the personal protective equipment (PPE) needed for hands and eyes during mixing, application and washing out of hairdressing chemicals. Large manufacturers of hairdressing chemicals often provide technical advisors who attend salons on a regular basis to offer training and advice about their products, as well as telephone helplines.
Gloves can be inconvenient to use due to the lack of sensation/dexterity required to cut hair, apply foils and so forth. They are not popular with clients as they snag and pull on the hair. Prolonged glove wearing can result in irritant dermatitis, or contact allergy to glove constituents may develop.
Gloves protect the individual from contact with irritants and allergens.
To maximise the benefits and minimise the disadvantages of gloves they should be:
It is inevitable that hairdressing clients will be directly exposed to the same irritants and allergens as the hairdresser or barber. Prior to any exposure of a chemical product, a discussion should take place between the hairdresser and client covering the following.
If the client has had skin problems or has reacted to hair products in the past, it is advisable to patch test the chemical prior to use. Most Material Safety Data Sheets for products used on the hair or skin recommend that a patch test be performed 48 hours in advance of application. Repeated contact allergic reactions, especially to paraphenylenediamine in hair dye, can be very serious and prolonged.
In-salon patch tests involve mixing a small amount of the chemical and applying it to a small area of cleaned skin, typically the inner aspect of the forearm or behind the ear, and covering it with an adhesive dressing.
If any sign of inflammation is present after 24 to 48 hours, the treatment should not proceed. The client should be advised to seek the advice of their medical practitioner. They may be referred to a dermatologist for formal patch tests.
Always ensure advice on the MSDS is followed and only ever use recommended concentrations.
If a hairdresser or barber has developed hand dermatitis, management may include: