Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction
Spider species that bite
Signs and symptoms
Clinical features
Bacterial infections from spider bites
Treatment
Spiders belong to the class of mainly terrestrial arthropods known as Arachnida. Medically significant classes of arachnids include spiders, ticks/mites and scorpions. Unfortunately through myths, legends and nowadays media, spiders have gained a reputation of being dangerous and harmful, and in some people instil a psychological fear known as arachnophobia. In reality, very few are dangerous to man and media reports exaggerating the dangers of spider bites are far out of proportion to the actual threat they pose.
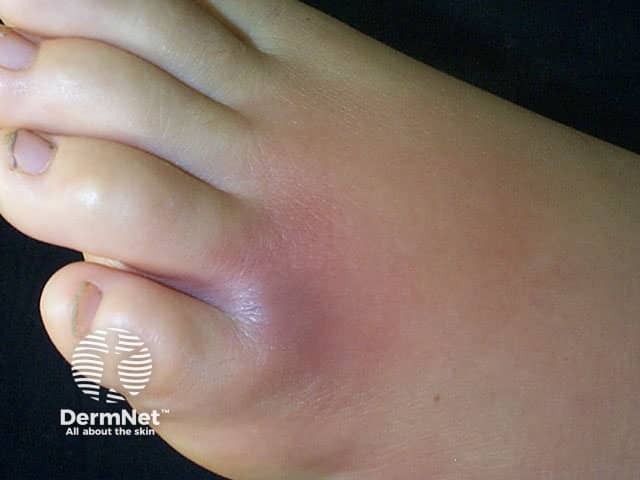
Day 1
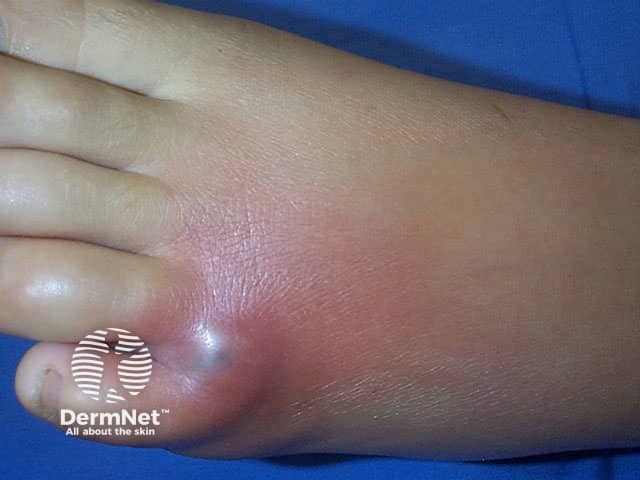
Day 2
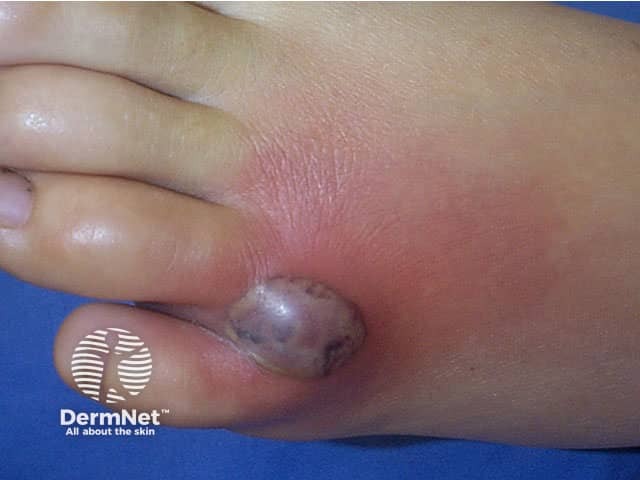
Day 3
Latrodectus spp (widow spiders) are found throughout the world and known by many different common names according to country.
Loxosceles spp is found in South America, United States, Australia, and commonly in the tropics.
Tegenaria agrestis (hobo spider) and Cheiracanthium (yellow sac spider) are found in the United States.
Phoneutria (banana spider) is found in Central and South America.
Atrax and Hadronyche (funnel-web spider) are found in Australia.
The venom produced by spider bites is generally either neurotoxic or cytotoxic. Web dwellers tend to have neurotoxic venom and non-web dwellers cytotoxic venom. Spiders of the Latrodectus genus produce neurotoxic venom, while the violin spider and yellow sac spider produce cytotoxic venom.
The signs and symptoms of a spider bite depend on many factors, these include:
The signs and symptoms from a bite from a spider with neurotoxic venom differ to those produced by a spider with cytotoxic venom. The severity of the symptoms depends on the species of the spider as the symptoms of bites from different species of Loxosceles can range from unremarkable (requiring no care), localised (usually self-healing), dermonecrotic (slow-healing ulcerated lesion requiring treatment), to systemic (vascular, renal damage and sometimes life-threatening).
Features of neurotoxic venom bite
Features of cytotoxic venom bite
The skin around the site of the bite is red and two fang marks may be visible where the skin was penetrated. In untreated cases, a rash may develop after several days. Systemic symptoms are of more diagnostic value.
The dermatological features of these spider bites depend on the severity of the bite. In self-healing wounds, the bite site gets no worse than being swollen and red. With more serious bites a “bull's eye” wound may form. This is characterised by a central red swollen blister that is separated from a peripheral bluish region by a white zone of firm swelling. If the bite turns a purplish colour within the first few hours, this usually indicates severe localised tissue death (necrosis) may occur. Over days the blister forms a scab, which hardens and falls off to leave behind an ulcerated depression. Healing can take weeks to months.
Interestingly, it appears that bites that become systemic do not also develop necrotic wounds. It is thought that in necrotic wounds the venom is localised in the tissue whereas in systemic reactions the venom is distributed quickly throughout the body without any localised effects.
Although many people attribute an episode of bacterial infection (especially cellulitis and necrotising fasciitis) to an unseen spider bite, they are falsely blamed. Documented spider bites have not led to skin these infections.
One of the most important aspects in treating spider bites it to try and identify the offending spider. The venom of spider bites is quite variable hence identification of the spider can be of value in determining the management of the condition.
General measures that should occur after a spider bite include:
Depending on the identification of the offending spider and the severity of the bite, treatment may include:
Specific treatment for bites from certain spiders include: