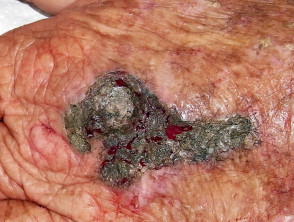
What is topical silver therapy?
Topical silver therapy is the use of silver in topical preparations applied to the skin, and wound dressings containing or coated with silver.
The most commonly used topical silver preparations are:
- Silver sulfadiazine cream (SSD)
- Silver nitrate (AgNO3)
Nanocrystalline silver dressings have been designed for sustained release of silver, reducing the need for frequent re-application of silver preparations or dressings. Silver dressings include:
- Polymeric films and meshes (eg Arglaes®)
- Nanocrystalline (eg Acticoat®)
- Hydrofibres (eg Aquacel® Ag)
- Foams (eg Avance®, Contreet® Ag)
- Hydrocolloids (eg SSD/hydrocolloid, Contreet® Ag)
- Activated charcoal (eg. Actisorb® Ag)
- Alginates and CMC (eg Silvercel®)
Topical silver therapy
How does topical silver therapy work?
Silver, in its ion form Ag+, has a broad-spectrum antimicrobial/antiseptic effect. It is thought to bind to bacterial cell walls and/or interfere with cell division and DNA replication.
What skin conditions respond to topical silver therapy?
Topical silver therapy can be used on acute thermal burns, other contaminated or infected wounds and chronic ulcers to prevent or treat infections and promote wound healing.
How effective is topical silver therapy?
Silver has been used to prevent transmission of infection dating back to 4000 BC. To date, silver dressings and preparations have not been found to be superior in efficacy or cost compared to topical non-silver therapy.
Preventing wound infections
In thermal burns, nanocrystalline dressings may be superior to topical silver preparations in reducing the incidence of infections, cost and pain. But silver sulfadiazine cream may increase the risk of infection, delay wound healing and be more painful when applied.
In chronic ulcers, silver dressings may help reduce the size of the ulcer short term and reduce the burden of bacterial overgrowth.
Treating wound infections
To date, there is no evidence that silver dressings reduce the time of healing or reduce the need for systemic antibiotics in contaminated or infected wounds.
Side effects of topical silver therapy
Side effects of topical silver therapy include:
- General adverse effects of dressings (maceration, irritant or allergic contact dermatitis)
- Rarely, acute haemolytic anaemia or transient leukopenia (silver sulfadiazine)
- Rarely, electrolyte imbalance (silver nitrate)
Contact dermatitis to silver dressing
Toxicity of topical silver therapy
- Argyria
- Cytotoxicity to host cells (fibroblasts and keratinocytes)
How to use topical silver therapy
- Refer to ‘synthetic wound dressings’ for a guided choice in dressing suitable for the wound and patient.
- Avoid using topical silver therapy on wounds with partial thickness thermal burns or donor sites to reduce the risk of toxicity in epithelialising wounds.