Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Wound infection is defined by the US Centre for Disease Control and Prevention (CDC) as surgical site infection (SSI). This is further defined as:
Although this definition of wound infection is restricted to those arising from a surgical incision, a broader and more general definition would be an infection of a wound caused by physical injury of the skin as a result of penetrating trauma from plants, animals, guns, knives or other objects. Wounds break the continuity of the skin and allow organisms to gain access to tissues and cause infection.
Infections arising in surgical wounds are one of the most common hospital-acquired infections and are an important cause of morbidity and mortality. Hence, the focus of this article is on the recognition and management of surgical wound infections.
A surgical wound/site infection is defined by the following criteria. Infection must occur within 30 days of the surgical operation, and at least one of the following must occur:
Other signs of wound infection include:
Surgical site infections do not include a stitch abscess, episiotomy infection, newborn circumcision scar, or infected thermal burn wound.
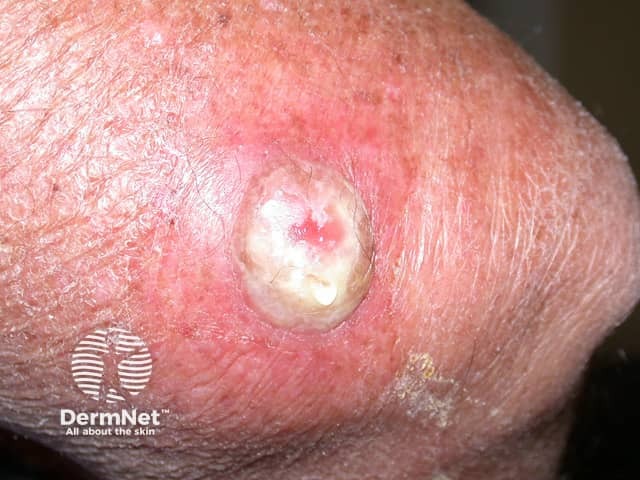
After cryotherapy
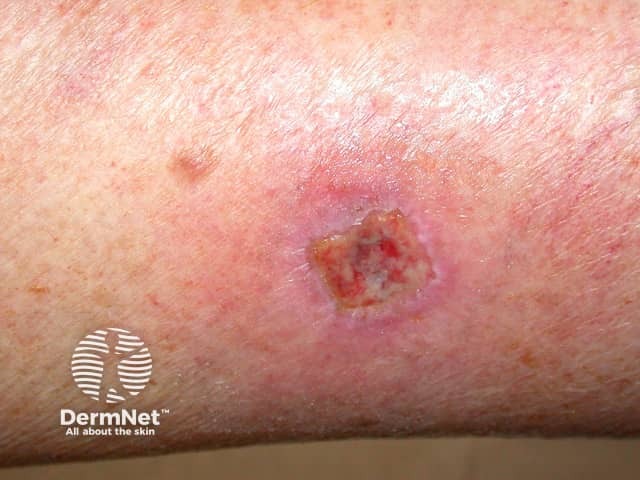
After curettage

After excision
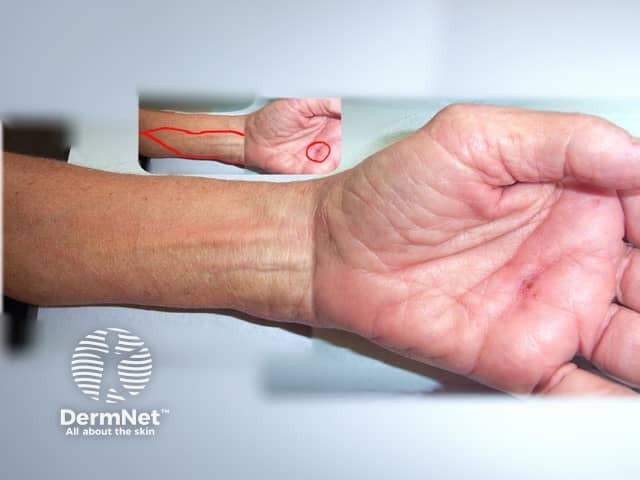
Lymphangitis following accidental wound. Image supplied by Dr T Evans.
Wound infections are caused by the deposition and multiplication of microorganisms in the surgical site of a susceptible host. There are a number of ways microorganisms can get into wounds.
The most common causative organisms associated with wound infections include Staphylococcus aureus/MRSA, Streptococcus pyogenes, Enterococci and Pseudomonas aeruginosa.
General patient characteristics
Wound characteristics
Operative characteristics
The risk of wound infection varies with the type of surgery. Certain types of surgery carry a higher risk of contamination than others and have led to the following classification of surgical wounds.
Clean wound, for example, hernia repair
Clean-contaminated wound, for example, an appendicectomy
Contaminated wound, for example, colectomy due to obstruction
Dirty wound
The goal of wound infection management is to prevent or minimise the risk of infection. The following factors or methods external to the patient are used to prevent infection.
Techniques applied to the patient to prevent wound infections include:
Antiseptic wound cleansers are adequate for clean wounds or lightly contaminated wounds. Antibiotic prophylaxis may be indicated for clean-contaminated wounds and is usually recommended for contaminated wounds. Antibiotics for dirty wounds are part of the treatment because the infection is already established. When deciding on a prophylactic antibiotic consider the following:
Wound infection can complicate illness, cause anxiety, increase patient discomfort and lead to death. It is estimated that surgical wound infections result in an increased length of hospital stay by about 7–10 days. Hence the prevention and management of wound infection have a major impact on both patient health and health economics.