Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2009.
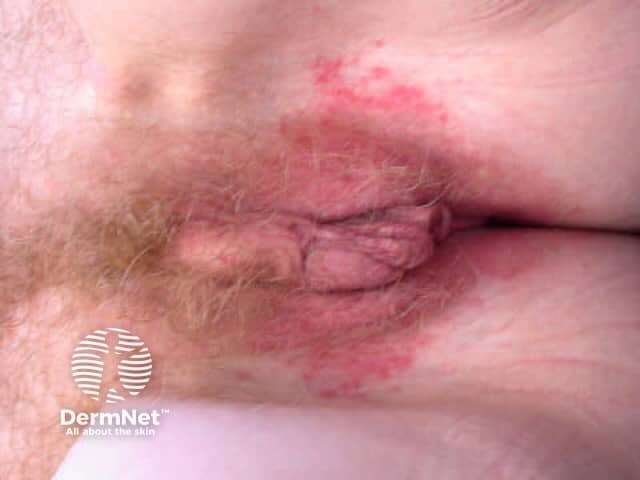
Perioral dermatitis is a common transient, recurrent or persistent rash affecting the muzzle area, hence its name. However, it often also affects skin adjacent to the eyes or nose, and sometimes around the anus or vagina, where it is more appropriately named “periorificial dermatitis”.
It appears more common in those with fair-skin and is particularly prevalent in women in their 20’s and 30’s.
Perioral and periorificial dermatitis are characterized by clusters of small papules and surrounding erythema. The surface may be scaly, and occasionally vesicles or tiny pustules develop. Typically, in contrast to contact dermatitis, 5-10mm skin adjacent to the vermilion of the lips is unaffected and may appear as a “white” ring. Symptoms vary from none to itch and burning discomfort depending on the severity and extent of the eruption.
Scaly papules Papules and erythema Papules and pustules Papules on the glabella Genital lesions 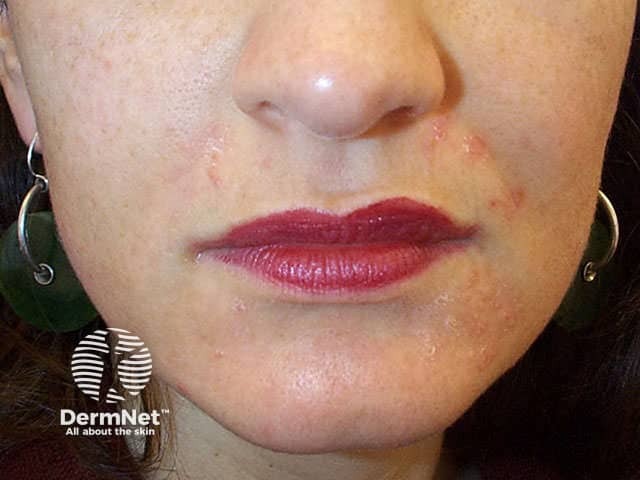
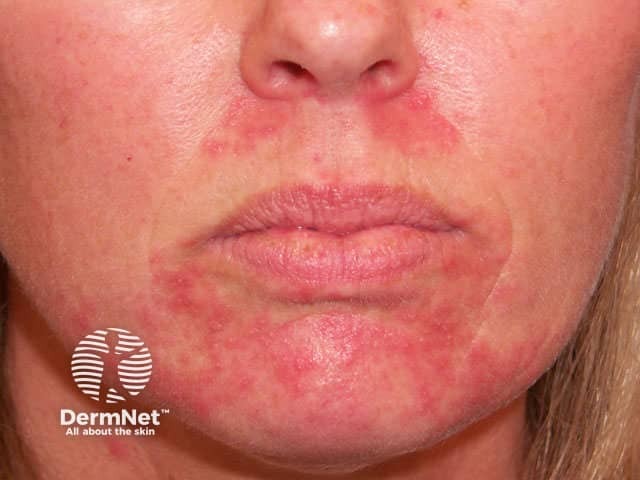
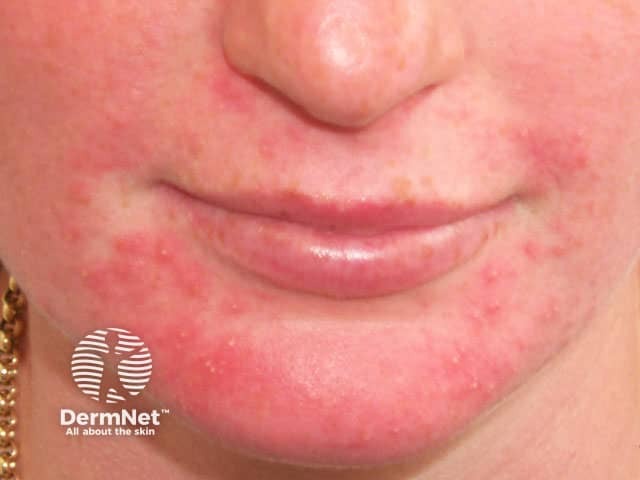
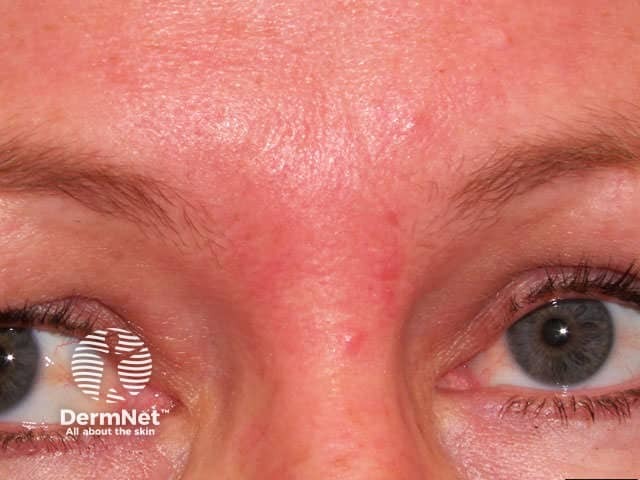
Unlike acne vulgaris, there are no comedones, cysts, or nodules. The areas affected are distinct from rosacea, which tends to occur a decade or so later and is accompanied by flushing and telangiectasia. However, longstanding perioral dermatitis is sometimes associated with telangiectasia, especially when due to topical steroids.
Perioral dermatitis may be precipitated by:
The cause is unknown – theories include proliferation of commensal fusobacteria or Malassezia yeasts, and hypersensitivity reactions perhaps to sodium lauryl sulphate or an emollient ingredient.
The description “dermatitis” can be misleading – it is not an eczematous dermatitis. Topical steroids make it look better for a day or two, but result in more extensive and more inflamed papules. The most severe cases have always applied topical steroids for weeks or months, and flare severely when these are discontinued.
Find out why topical steroids may cause or aggravate perioral dermatitis.
Information for patients
See the DermNet bookstore