Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Dr Nayab Shah, Royal Perth Hospital, Australia. Copy edited by Gus Mitchell. July 2022
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Periorificial dermatitis (POD) is a relatively common chronic inflammatory skin eruption. It preferentially targets cutaneous orifices as implied in its name ie, around the eyes, nostrils, mouth, and occasionally the genitals.
Periorificial dermatitis may be limited to a single orifice, where it is more appropriately termed:
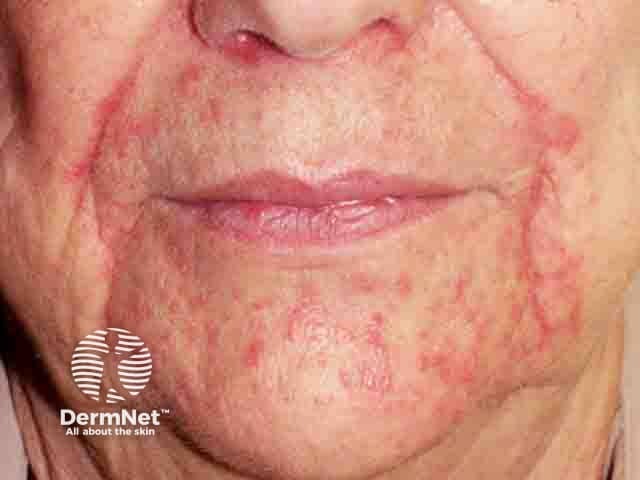
Perioral erythematous papules sparing the immediate perivermillion skin in perioral dermatitis
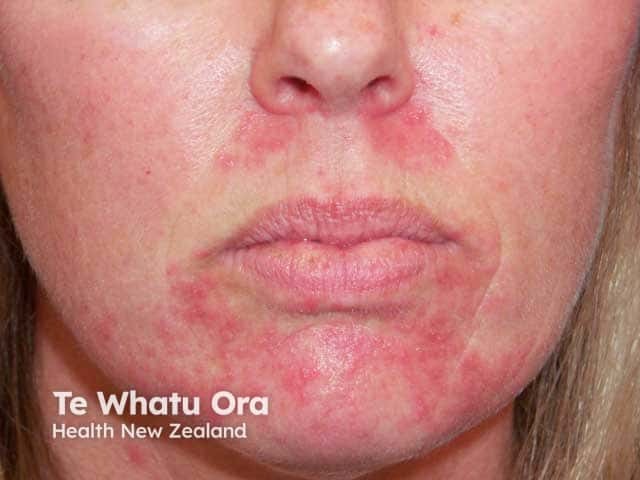
Perioral and nasolabial fold papules sparing the perivermillion skin in perioral dermatitis
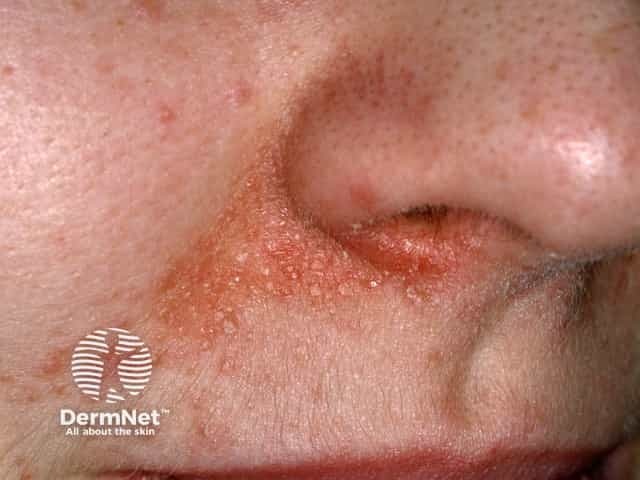
Perioral dermatitis
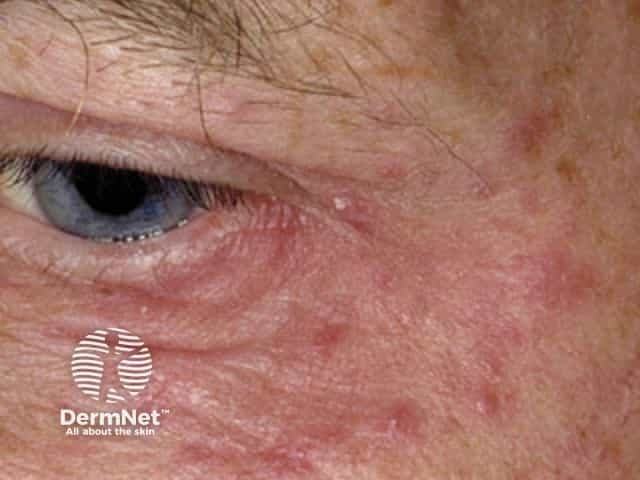
Periocular dermatitis
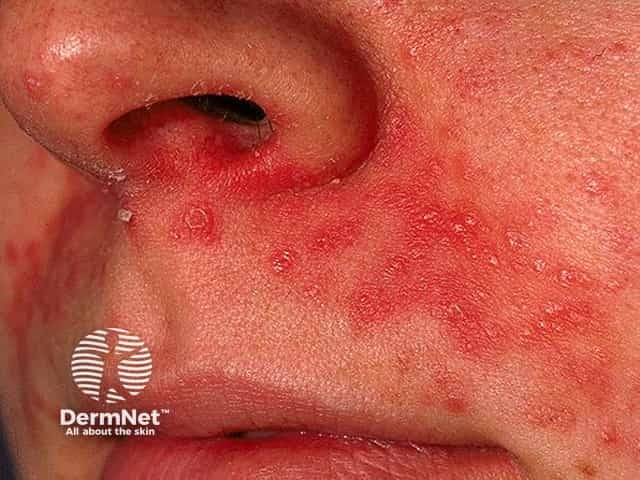
Perioral dermatitis
Periorificial dermatitis is slightly more common in lighter-skinned females and usually affects young to middle-aged women (20–45 years). However, it is also seen in young children, often between 7 months to 13 years old.
The exact incidence and prevalence remain unknown.
The exact cause is not understood. A suggested mechanism proposes epidermal dysfunction as the primary disturbance, resulting in:
Physical factors including UV light, heat, and wind seem to worsen periorificial dermatitis.
Cutaneous features of periorificial dermatitis include:
Pain is rare, although skin sensitivity is common and patients are otherwise systemically well.
Whilst usually limited to the affected orifice, more severe POD may extend to the chin, cheeks, lateral lower eyelids, upper eyelids, forehead, and glabella. The immediate peri-vermillion skin is often spared, only rarely is it affected in severe cases.
Topical steroids can obscure the primary rash and may also result in steroid-induced cutaneous side effects.
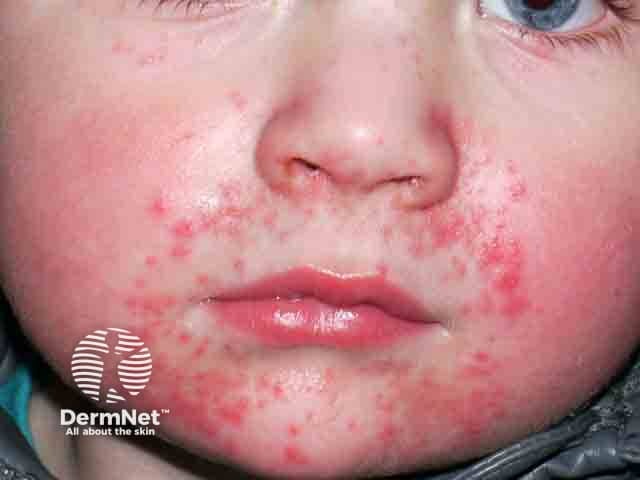
Perioral dermatitis due to the use of a steroid nebuliser mask
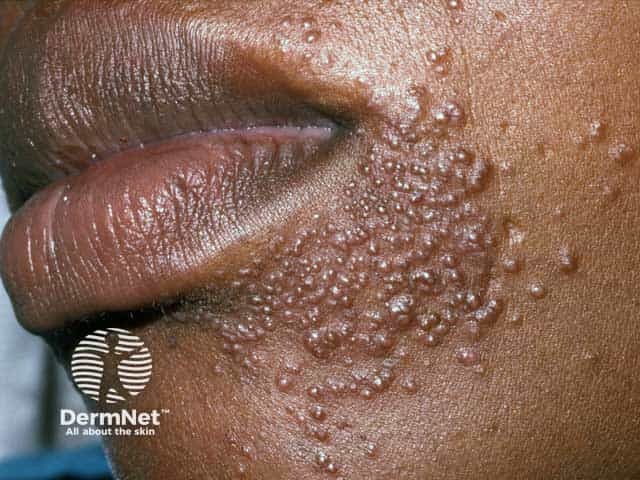
Papules and pustules (an unusual feature) in perioral dermatitis
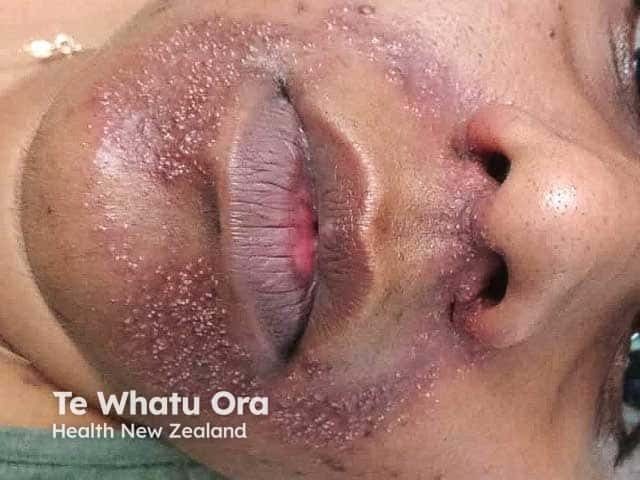
Florid perioral dermatitis due to potent topical steroid use
This is a severe subtype of POD. Eruptions are denser and larger with red-brown papules. The affected skin shows lupoid infiltrates, with a characteristic apple-jelly colour on diascopy. This subtype can result in permanent scarring.
CGPD is a rare variant often seen in children with dark-coloured skin. It was previously termed FACE (Facial Afro-Caribbean Childhood Eruption). However, it has since been renamed as it has been observed in children with light-colour skin and those not of Afro-Caribbean heritage.
Patients present with skin-coloured, red or yellow-brown monomorphic, dome-shaped papules. There is typically a lack of pustules and vesicles in CGPD, and erythema and scaling are less prominent than in classic POD. Additionally, the histological features between CGPD and POD are different.
Extra-orificial skin can also be affected with an eruption on the neck, chest, and extremities, in addition to conjunctivitis and blepharitis.
POD is a clinical diagnosis. Other investigations that may be used are:
CGPD characteristically shows perifollicular and upper dermal tissue containing noncaseating granulomas surrounded by lymphocytes and often giant cells. Again, epidermal spongiosis may be present.
Differential diagnosis depends on the site(s) involved.
Periorificial dermatitis is a benign self-limiting condition with no systemic consequences. However, it may be cosmetically unacceptable to the patient, resulting in significant disease burden and psychological distress. Periorificial dermatitis usually responds well to treatments.
The POD Severity Index (PODSI) has been used in literature to help quantify disease severity and response to treatment.
The zero-therapy approach should be utilised in all POD patients and may result in complete resolution of mild cases. Advise patients to:
Medically necessary nasal, inhaled, and oral steroids should be continued but will increase recovery time. Rinsing the face and mouth after using nasal or inhaled agents may help.
Topical and/or systemic treatments are available; duration is usually 4–8 weeks but may require an extension. Recurrence can occur if treatment is too short.
Topical treatments are often not tolerated due to associated facial sensitivity; if they are, they may be rotated every 6–8 weeks if the patient fails to respond.
Other topical therapies have limited evidence supporting efficacy and safety. These include:
Sub-antimicrobial doses may be effective for some patients. In cases resistant to systemic therapy, a combination of oral and topical therapy may be considered.
Periorificial dermatitis, including CGPD, often runs a chronic variable course that may last months to years without treatment. Usually, there is no scarring or disturbance to skin pigmentation except in severe and lupoid cases.
With treatment, most patients recover well. If POD recurs when antibiotics are discontinued, or in the future, the same treatment can be used again.