What is an allergy?
Allergy is an abnormal response of the body to a foreign body, known as an antigen. It involves the immune system recognising this antigen and mounting one of four types of response, which are detailed below.
Allergy is also known as a ‘hypersensitivity reaction’ or a ‘hypersensitivity response’.
This article uses the terms allergy and hypersensitivity interchangeably. An allergy refers to the clinical syndrome while hypersensitivity is a descriptive term for the immunological process.
How is an allergy different to intolerance?
Intolerance refers to an individual’s ability to handle different types of food or drink. Food intolerance is not a true allergy, in that there is no clearly defined immune response and the symptoms that often develop only affect the digestive tract. An intolerance is normally found in the context of a deficiency in certain enzymes that break down the components of food. The absence of these enzymes thus results in abnormal byproducts that produce the symptoms of intolerance.
In contrast, a true allergy tends to affect multiple organ systems within the body and tends to have a poorer outcome.
- A true food allergy means that the individual is required to avoid that food for life or risk the consequences.
- Food intolerance means the individual can eat small amounts of food without obvious consequences while eating larger amounts may lead to stomach cramps, nausea, or diarrhoea.
A good example of the difference between an allergy and food intolerance can be made by comparing coeliac disease, an allergy, with lactose intolerance.
- Patients with coeliac disease have an allergy to gluten, the main component found in wheat, rye, barley and often contaminates oat products. In coeliac disease, the ingestion of gluten results in a specific immune response against the gluten, leading to inflammation and the destruction of the lining of the small intestine. This leads to the malabsorption of important vitamins and minerals, which if left untreated can be life-threatening.
- Lactose intolerance is due to a deficiency in the enzyme (lactase) that breaks down lactose, a type of sugar commonly found in dairy products. The absence of this enzyme results in abnormal levels of lactose in the bowel, which leads to the feeling of bloating, diarrhoea, cramps, and nausea. While uncomfortable, the continued ingestion of lactose is not life-threatening.
Type I hypersensitivity reaction
Type I hypersensitivity reaction is the most widely known type of allergic reaction and includes anaphylaxis; this is where the body reacts to a stimulus, or allergen, leading to swelling of the airways, and cardiovascular and other organ system effects. True anaphylaxis is uncommon.
Anaphylaxis occurs when a specific type of antibody, immunoglobulin E (IgE), recognises a foreign antigen and attaches itself to it. By attaching to the antigen, the IgE activates a chain of reactions that result in the widespread release of chemicals, including histamine.
Type I hypersensitivity reactions include:
- Food allergies, such as peanuts and shellfish
- Pollen-food allergy syndrome
- Bee sting reactions
- Penicillin allergy
- Latex allergy.
The symptoms of a type I hypersensitivity reaction include:
- Urticaria (also known as hives; note that most cases of urticaria are not due to a hypersensitivity reaction)
- Hay fever
- Asthma
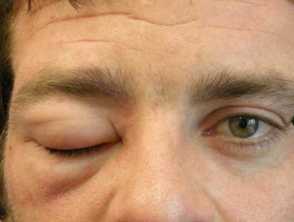
- Angioedema — swelling of the face; typically around the eyes and mouth
- Anaphylaxis — this is at the end of the reaction and includes:
- Airway swelling (laryngeal oedema)
- Hypotension and resultant shock
- Diarrhoea and other organ dysfunction.
Type I hypersensitivity reactions
Diagnosis of type I hypersensitivity reactions
The diagnosis of type I hypersensitivity reactions is largely based on the patient’s clinical history of typical symptoms and signs following exposure to a particular allergen. Tests can aid in confirming the diagnosis.
- A full blood count may show eosinophilia.
- The serum tryptase level is elevated in most cases of anaphylactic reaction when measured within the first 1–2 hours after the event.
- A radioallergosorbent test (RAST) can be used to identify the causative allergen. This assay detects specific IgE antibodies against a range of common allergens.
- RAST has now largely been replaced by fluoroenzyme assays (eg, the ImmunoCAP assay), which are more sensitive at detecting allergen-specific IgE.
- Skin prick testing is widely used to test for type I hypersensitivity reaction. A small number of common allergens or patient-specific allergens are inoculated directly under the skin. The skin reaction is then compared against a control area to see if a positive (ie, allergic) reaction occurs. Prick testing should not be used to test for an allergen that has caused anaphylaxis or when severe pre-existing skin disease would obscure the result.
- Atopy patch tests are used to determine whether type 1 allergens might be contributing to atopic dermatitis (which is ordinarily not considered due to a specific allergy).
Treatment of type I hypersensitivity reactions
Anaphylaxis is a medical emergency requiring prompt recognition and treatment. Treatment of type I hypersensitivity reactions include:
- Adrenaline intramuscularly to reverse the airway swelling and cardiovascular effects
- Systemic glucocorticoids to lessen the inflammatory reaction while the body clears the allergen
- Antihistamines to prevent the action of widespread histamine release
- Avoidance of the allergen in future.
People with known anaphylaxis to common environmental triggers (eg, bee venom or peanuts) may carry a pre-loaded adrenaline syringe or an adrenaline pen (eg, an EpiPen) that allows the rapid and easy injection of adrenaline into the thigh muscle in an emergency.
- Antihistamines are often enough to control mild symptoms (eg, urticaria).
- Topical steroid nasal sprays can be used to control hay fever.
Desensitisation
Desensitisation can be performed by an allergy specialist (an immunologist with interest in allergy) within the hospital environment. It involves gradually exposing the patient to increasing doses of the allergen (eg, an antibiotic) in an attempt to desensitise the patient’s immune response.
Type II hypersensitivity reaction
Type II hypersensitivity reactions, or autoimmune reactions, are due to the abnormal binding of antibodies to normal host targets. Autoimmune diseases involve immunoglobulin G (IgG) and M (IgM) antibodies that activate the complement cascade. This causes inflammation and damage to tissues.
The complement cascade forms part of the innate immune system that fights infection. The innate immune system always responds in the same way to a foreign stimulus and does not change or adapt over time. When exposed to a foreign protein, the complement cascade activates the adaptive immune system to form antibodies. Over time, the antibodies remember the foreign protein and clear foreign invaders (eg, bacteria and viruses) and damaged cells. It is a self-amplifying cascade of enzyme activation: downstream enzymes act to further increase the level of activation of the upstream enzymes, thereby increasing the response.
Cutaneous examples of type II hypersensitivity reactions include:
Diagnosis of type II hypersensitivity reactions
The diagnosis of a type II hypersensitivity reaction is confirmed by detecting causative antibodies. Direct immunofluorescence is used in skin biopsies of the skin adjacent to blisters to detect bullous pemphigoid and pemphigus vulgaris.
-
- In bullous pemphigoid, antibodies target the interface between the dermis and epidermis, resulting in the loss of adhesion of the epidermis to the dermis.
- In pemphigus vulgaris, the antibodies target proteins anchoring adjacent cells in the epidermis to each other, resulting in the loss of adhesion between the epidermal cells.
Type II hypersensitivity
Treatment of type II hypersensitivity reactions
Currently, immunosuppression is the mainstay of treatment to prevent the action of abnormal antibodies.
- Systemic glucocorticoids in high dose are often used to suppress the disease when it first presents or when it flares. Long-term glucocorticoids have significant side effects and therefore the dose is usually tapered over time.
- Cyclophosphamide and ciclosporin are glucocorticoid-sparing agents that can be used long term to achieve immunosuppression. Close monitoring by a specialist is usually required.
- Intravenous immunoglobulin infusions deliver human-derived antibodies to target abnormal antibodies to neutralise them and prevent them from reaching their target site of action.
- Plasmapheresis is a process whereby the patient’s blood is passed through a machine that filter outs the antibodies before the ‘cleaned’ blood is returned to the patient.
A note on type V hypersensitivity reactions
Type V hypersensitivity is a relatively newly described reaction in which an antibody targets receptors on the cell surface that are normally activated by hormones. It is likely a subset of type II hypersensitivity reactions, as it involves an antibody targeting a specific structure within the body, leading to the clinical syndrome through abnormal cell signalling, either through the antibody activating a receptor or through blocking the binding of the normal hormone. No dermatological type V hypersensitivity reactions have been described.
Common non-cutaneous examples of type V hypersensitivity reaction include:
- Graves disease
- Myasthenia gravis.
Type V hypersensitivity reaction
Type III hypersensitivity reaction
Type III hypersensitivity reaction involves IgG antibodies bound to foreign antigens in the blood. These antibody–antigen complexes can precipitate and get stuck in certain locations, such as blood vessels in the skin, kidneys and joints, where they activate the complement cascade to cause local damage.
Common cutaneous examples of type III hypersensitivity reactions include:
- Henoch–Schönlein purpura
- Small-vessel vasculitis
- Systemic lupus erythematosus
- Rheumatoid arthritis
- Serum sickness.
Most commonly, immune-complex reactions cause palpable purpura, the hallmark of small-vessel vasculitis. These are visible, non-blanching haemorrhages that are raised and palpable on examination.
Type III hypersensitivity reactions
Diagnosis of type III hypersensitivity reactions
There are a large variety of diseases that can lead to type III hypersensitivity reactions. The appropriate tests are dictated by the patient’s clinical history and examination. There is no single test that can identify the cause of the hypersensitivity reaction.
Punch biopsies of the vasculitis rash typically show a leukocytoclastic reaction, in which there is superficial and mid perivascular neutrophilic infiltration with fibrinoid necrosis of the vessels and fibrin extravasation.
Treatment of type III hypersensitivity reactions
The treatment for type III hypersensitivity reactions is aimed at controlling the underlying disease. It often involves immunosuppression with systemic glucocorticoids and disease-modifying drugs, such as methotrexate, ciclosporin and cyclophosphamide.
Type IV hypersensitivity reaction
Type IV hypersensitivity or delayed hypersensitivity reaction occurs 48–72 hours after exposure to the allergen. This reaction does not involve antibodies. Instead, eosinophils, monocytes, or lymphocytes called T cells are activated by the antigen. The helper CD4+ T cells initially recognise the antigen, releasing cytokines that activate the immune system with killer CD8+ T cells to destroy the target cells on contact, and macrophages to wall off the antigen and prevent further damage.
Common examples of cutaneous type IV hypersensitivity reactions include:
- Allergic contact dermatitis — commonly to hair dye, nickel in jewellery, Toxicodendron spp. (eg, poison ivy, Rhus)
- The Mantoux test (used to detect active tuberculosis)
- Delayed drug reactions, including:
- Morbilliform drug reactions
- Drug hypersensitivity syndrome (formerly known as drug reaction with eosinophilia and systemic symptoms [DRESS])
- Erythema multiforme
- Lichenoid drug eruptions
- Steven–Johnson syndrome (SJS) / toxic epidermal necrolysis (TEN).
Type IV hypersensitivity reactions
Diagnosis of type IV hypersensitivity reactions
A thorough history and examination are required to identify the likely causative agent when considering a possible allergic contact dermatitis. Diagnosis is confirmed through patch testing (also known as a contact delayed hypersensitivity allergy test).
- Small quantities of the potential allergens are applied to the skin.
- They are left in situ for two days.
- A patch of eczema at the site of an allergen is a positive reaction.
- Atopy patch tests using type 1 allergens are sometimes used in patients with atopic dermatitis.
Treatment of type IV hypersensitivity reactions
The mainstay of treatment for type IV hypersensitivity reactions is the avoidance of contact with the causative agent. For example, people with nickel allergy should select jewellery and clothing items that do not contain the metal.
Symptomatic relief of contact dermatitis is achieved through emollients and topical steroids.
Systemic corticosteroids are prescribed for severe reactions and tapered over 2–3 weeks to prevent a recurrence of the rash.
Monoclonal antibody use for the treatment of hypersensitivity reactions
Monoclonal antibodies are antibodies generated within a laboratory setting that can be directed against the abnormal antibodies or cells in an affected individual. They can be directed against very specific molecules, allowing for specific targeting within a disease pathway. Monoclonal antibodies can be used in treating hypersensitivity reactions.
Omalizumab
Omalizumab is an anti-IgE antibody, and therefore can be used in treating type I hypersensitivity reactions. It has been shown to have benefit in patients with moderate-to-severe asthma. Its use in other allergic conditions is also being studied.
Rituximab
Rituximab is an anti-CD20 monoclonal antibody that is helpful in treating type II and III hypersensitivity reactions. Rituximab is directed against the CD20 molecule found on the surface of B cells that produce antibodies. The rituximab acts as a signal for natural killer cells within the blood to target B cells and destroy them, reducing the level of abnormal antibody production seen in type II and III hypersensitivity reactions.
Anti-complement monoclonal antibodies
Anti-complement monoclonal antibodies are antibodies directed against certain components within the complement cascade. These biologic agents are already in use for several immunological diseases and are being investigated in hypersensitivity reactions.