What are topical medications?
Topical medications include any balm, cream, gel, oil, lotion, patch, ointment, or any other product with a medicinal ingredient that is applied to the skin.
A topical medication is made up of an active ingredient and base which may contain preservatives and fragrances. Many topical formulations are available over-the-counter and include products such as antibacterial and antifungal preparations, anti-inflammatory and pain-relief preparations, and cleansing and moisturising agents.
How does allergy to a topical medication present?
An allergy to a topical medication can produce a range of reactions.
- Contact urticaria results in a local burning sensation, tingling, itching may occur within minutes to about 1 hour after contact with the skin.
- Swelling and redness (weal and flare) may be seen.
- Rash usually resolves by itself within 24 hours of onset.
- Anaphylaxis causes difficulty breathing, nausea, vomiting, acute urticaria and angioedema
- Rarely occurs but can be fatal.
- Irritant contact dermatitis accounts for 80% of all cases of contact dermatitis.
- It can occur in anyone but people with a history of atopic dermatitis are more prone to irritant dermatitis.
- It usually begins as patches of itchy, scaly skin or red rash, but can develop into blisters that ooze.
- For strong irritants, a reaction may occur within minutes or hours of exposure.
- For weaker irritants, it may take days or weeks of continued exposure before symptoms appear.
- In allergic contact dermatitis, a reaction only occurs when a person’s immune system is sensitised to the allergen (the person is allergic to a specific ingredient).
- A rash usually develops more than 12 hours after contact with the allergen and usually peaks about 48 hours after exposure.
- Symptoms include redness, swelling, intense itching and hive-like breakouts.
- A photosensitivity rash is caused by the interaction of sunlight with an ingredient in the product.
Some people may suffer from one or more reactions. In particular, atopic individuals (patients with atopic eczema, asthma and/or rhinitis) are more prone to irritant contact dermatitis, which in turn increases their likelihood of allergic contact dermatitis as their skin barrier function is weakened and more sensitised to the allergen.
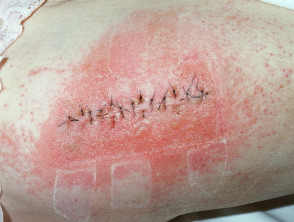
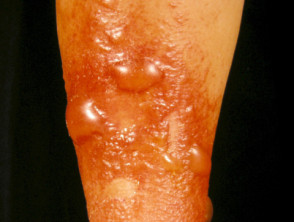
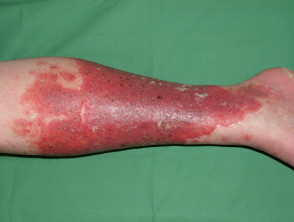
Contact dermatitis caused by topical medication
What are the allergens in topical medications?
Allergens found in topical medications may be the active drug ingredient or a component of the vehicle or base that carries the drug.
Drug allergens found in topical formulations that may cause allergic skin reactions include:
- Neomycin — antibiotic that is used widely in topical creams, ointments, lotions, eye preparations and eardrops. These prescription and non-prescription preparations are used to treat a variety of skin, eye and external ear disorders. Other topical antibiotics may also cause contact allergy, including bacitracin.
- Corticosteroids — anti-inflammatory agents used in the treatment of many conditions and diseases. There are many different types of topical corticosteroids with varying potencies and actions. They are also commonly found in combination preparations with antibacterials and antifungal agents.
- Benzocaine — widely used local anaesthetic often used topically. Doctors and dentists use benzocaine preparations, especially on mucosal surfaces such as the mouth, to prepare or 'numb' a site for injection. Local anaesthetics such as benzocaine are also found in some haemorrhoidal preparations
- Salicylate — is a chemical found naturally in plants and is the main ingredient of the pain-relieving tablet, aspirin. It is used in muscle pain creams.
- Non-steroidal anti-inflammatory drugs — these are used in topical gels and creams to treat muscle and joint pain.
The groups of allergens found in the base of topical medications that most frequently cause allergy are fragrances and preservatives.
Am I allergic to a topical medication?
Allergy to a topical medication is diagnosed by performing special allergy tests, called patch tests. Diagnosis may involve testing against the active drug ingredient or a component of the base. See individual contact allergens for patch testing recommendations.
It appears that allergy to topical medications is more common in older patients. A study of all patients patch tested at a Sheffield hospital over 9 years confirmed that contact allergy to topical medicaments is more common in those aged more than 70 years compared with the younger age groups.
Some patients with pre-existing skin conditions may be more at risk of developing allergic reactions to topically applied medications.
- Individuals with venous eczema are at high risk for developing an allergy to agents applied to the affected area. Topical neomycin is an important cause of allergic contact dermatitis in these patients because it is used frequently despite the lack of documentation of its efficacy in the treatment of stasis ulcers.
- Patients with otitis externa are often allergic to topical neomycin and topical corticosteroids.
What is the treatment for allergy to a topical medication?
Contact dermatitis should clear rapidly once the offending allergen is removed. In cases where the allergen is not a topical corticosteroid, over-the-counter mild topical steroids, such as hydrocortisone 0.5–2.5%, may be used to help control itching, swelling, and redness. In more severe cases, a prescription steroid cream may be required, as well as antibiotic medication if the skin becomes blistered and infected (impetiginised).
Care needs to be taken when prescribing a topical medication to older patients with eczema, especially for preparations that contain perfumes, lanolins (wool alcohols), and local anaesthetics as these are the allergens most commonly associated with allergic skin reactions in this group of patients.