Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Sonam Vadera, Medical Student, University College London, United Kingdom. DermNet New Zealand Editor in Chief: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy Editor: Gus Mitchell. September 2017.
Introduction - bleeding
Introduction - bruising
Demographics
Causes
Symptoms
Tests
Medical care
Treatment
Outcome
Prevention
Bleeding, also called haemorrhage, is the term used to describe blood escaping from the blood vessels. Bleeding from the skin occurs if there is an injury to the skin surface, and it may sometimes occur spontaneously. Smaller areas of bleeding are known as petechiae (each spot is < 2 mm) and purpura (2 mm to 1 cm).
Subungual haemorrhage, or bleeding under a nail plate, results in painful or unnoticed purplish-black discolouration. The discolouration may persist for months as the nail carries the blood with it as it grows out.
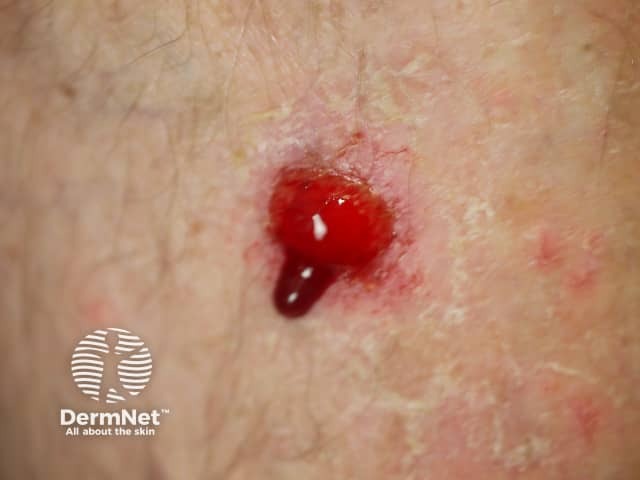
Bleeding basal cell carcinoma
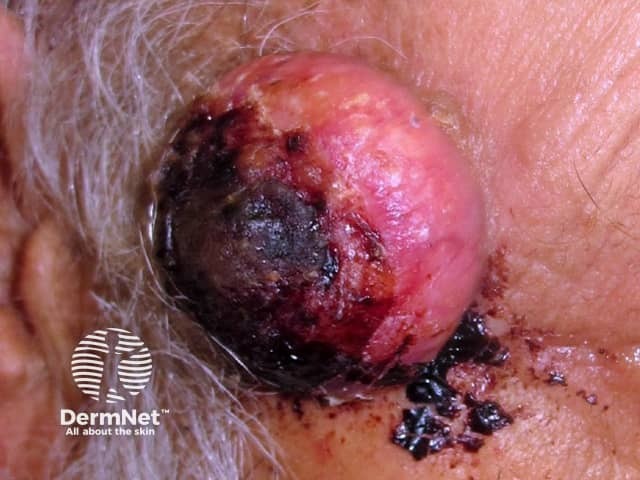
Crusted squamous cell carcinoma

Subungual haematoma
A bruise, also known as ecchymosis or a contusion, occurs when small blood vessels (capillaries) under the skin bleed, while the overlying skin remains intact. The injury causes blood to leak and collect near the skin surface, causing bluish-black skin discolouration.
Deeper bruising results in a haematoma — a collection of blood that lies within body tissues or cavities.
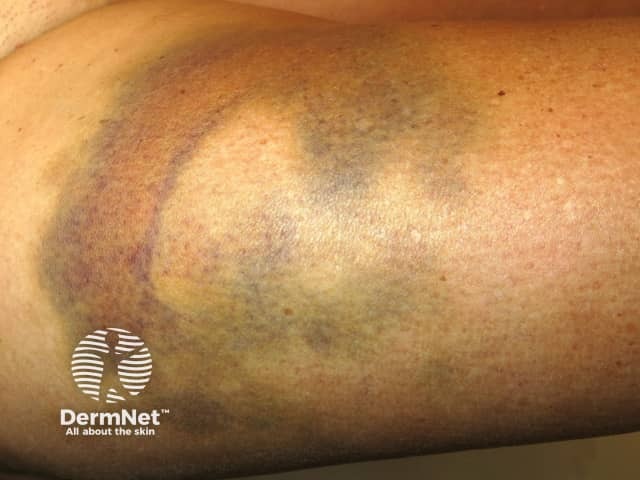
Traumatic bruise
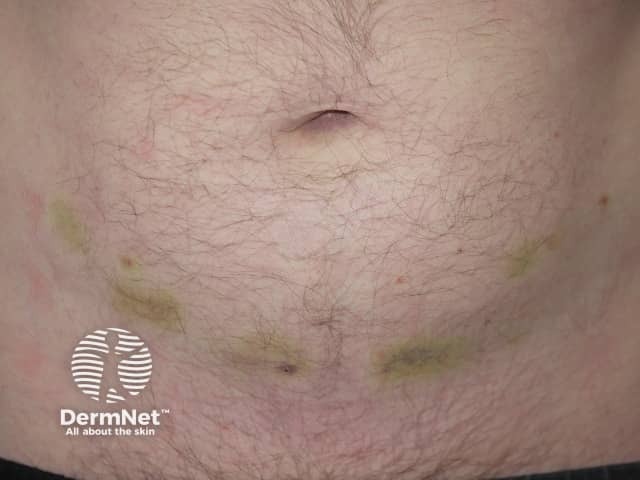
Bruising at the site of heparin injections
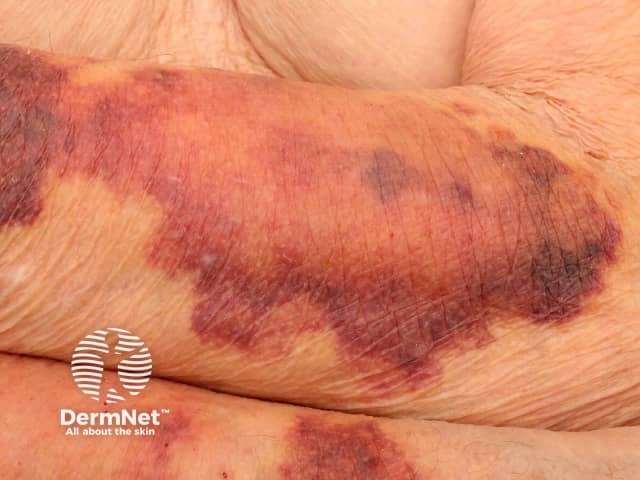
Ecchymoses associated with skin atrophy
Anyone can bleed from a cut or develop a bruise after an injury. The severity of bleeding depends on the impact of an injury. Repeated bleeding from a skin lesion with minimal provocation can be a sign of skin cancer, most often basal cell carcinoma.
Occasional bruises are normal and do not warrant medical attention. Bleeding and bruises are more common in certain individuals, such as:
Bruising occurs more readily in certain sites where blood accumulates easily, such as when a relatively minor bump results in a black eye.
After an injury, the body immediately attempts to stop any blood loss.
Defects in any of these three responses can lead to spontaneous or excessive bleeding and bruising.
Platelets can be dysfunctional or decreased in number. This can be due to conditions, such as:
Blood vessel defects, where the vessels are twisted or enlarged, include:
A clotting factor deficiency may be due to drugs that affect clotting factors (eg, warfarin, heparin, rivaroxaban and apixaban). These are often prescribed for atrial fibrillation or a recent blood clot in veins or lungs. A clotting factor deficiency can also be a result of a medical condition, such as:
The use of systemic or topical steroids can also increase the likelihood of bruising.
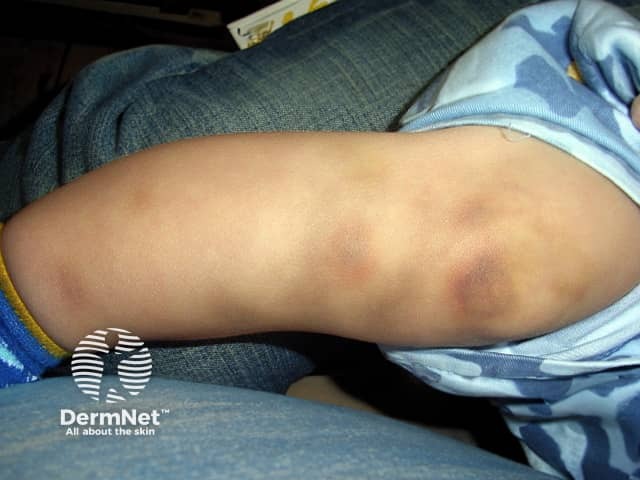
Bruises due to haemophilia
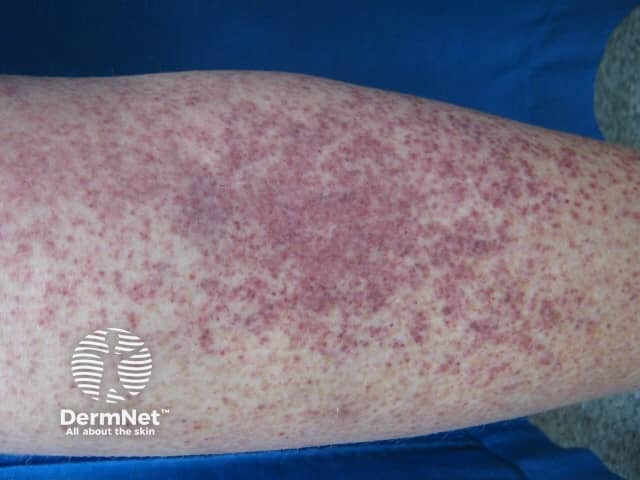
Petechiae due to thrombocytopaenia
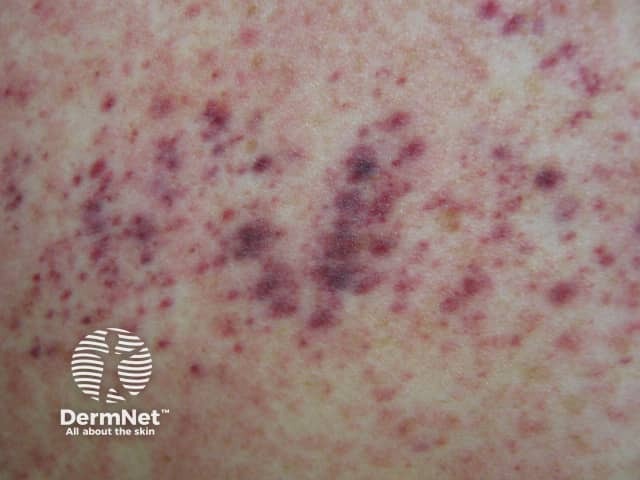
Petechiae due to thrombocytopaenia
Larger blood vessels, such as arteries, lead to more profuse and prolonged bleeding than smaller ones, such as capillaries. Once bleeding has stopped, a blackish crust or scab forms while the wound heals underneath.
Typically, a bruise first appears as a reddish patch, which develops over a few hours into a blue, black or purple discolouration. It may feel tender immediately after bruising, and the area may be swollen. Over a few days, the colour fades to a yellowish-green, as the leaked blood breaks down.
Usually, tests are not required for bruises. However, if a broken bone is suspected, an X-ray may be required.
If bruises are occurring for no reason or extremely frequently, blood tests may be required to confirm a platelet defect and determine if there is an underlying medical problem.
Urgent medical care is required if the bruising is associated with swelling and extreme pain, as it could indicate a fracture in the underlying bone.
A medical assessment is also indicated for:
There is no particular medical treatment for bruises. However, there are some techniques that can be used at home to reduce swelling and speed up the process of healing.
Non-steroidal anti-inflammatory drugs, such as aspirin and ibuprofen, are not recommended, as they may worsen the bleeding leading to the bruise.
Bruises usually take around two weeks to disappear. They may take longer to disappear from the lower legs.