Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated by Dr Jessica Witherspoon, General Practice Registrar, Doctors Grand Plaza, Brisbane, QLD, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. October 2018.
Introduction
Demographics - ephelides
Causes - ephelides
Clinical features - ephelides
Introduction - lentigines
Demographics - lentigines
Causes - lentigines
Clinical features - lentigines
Diagnosis - lentigines
Differential diagnoses - lentigines
Treatment
Brown spots and freckles on sun-exposed skin are ephelides (the plural of ephelis) and lentigines (the plural of lentigo). The difference between an ephelis and a lentigo is that an ephelis fades during the winter months while a lentigo persists in the absence of ultraviolet (UV) stimulation. Ephelides and lentigines can occur in the same individuals and the risk factors for both are generally the same.
Ephelides are very common in fair-skinned people, especially in children with red hair, where the MC1R gene is thought to be the main gene involved. They are an inherited characteristic that also sometimes affects people with darker skin types.
An ephelis is brown because of the pigment melanin. Melanin is made by melanocytes and diffused into keratinocytes. Melanin production by melanocytes decreases during the winter months, and increases when the skin is exposed to the UV radiation in sunlight. The colour is due to the localised accumulation of melanin in keratinocytes. There is no increase in the number of melanocytes.
Ephelides arise on an individual's mid face and sometimes more widely from early childhood onwards. As the person ages, this type of freckle generally become less noticeable. They are more prominent in summer but fade considerably or disappear in winter. An ephelis is usually less than 3 mm in diameter.
Apart from the need for sun protection, no particular treatment is necessary.
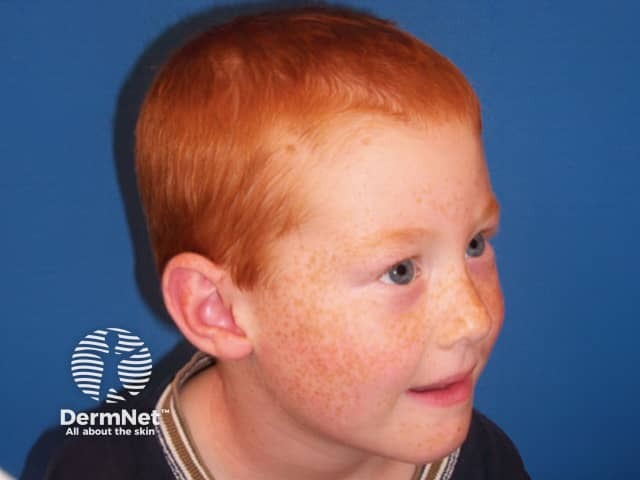
Freckles
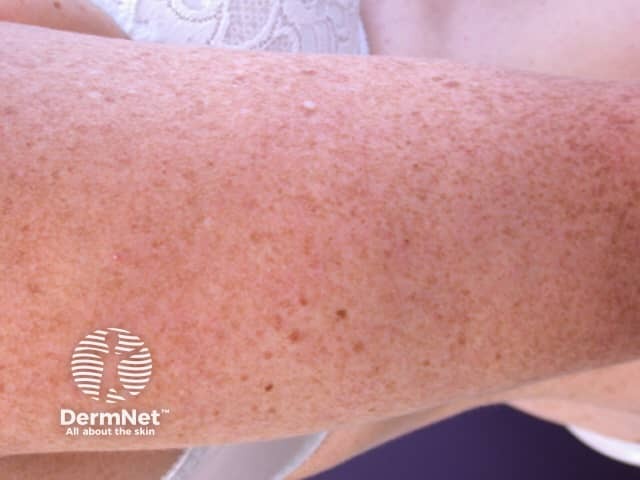
Freckles
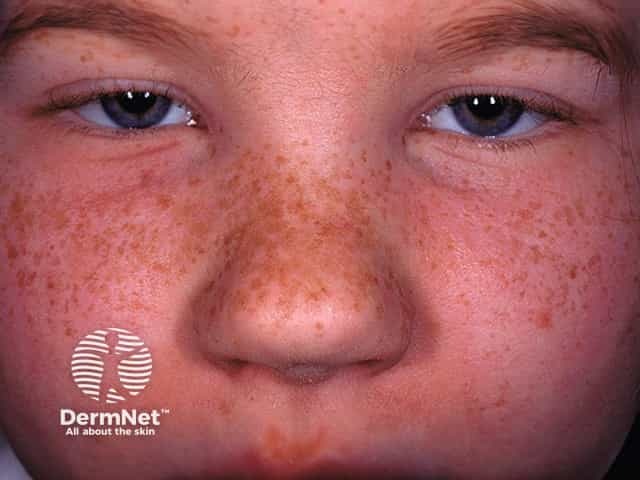
Freckles
Lentigines are brown flat lesions with a clearly defined edge. The most common type, solar lentigines, arise in middle age and result from sun damage. They are most often found on the face and hands, and they are larger and more defined than freckles. Other types of lentigo include ink spot lentigo and lentigo simplex.
Lentigines are common in people with fair skin, but they also frequently arise in sun-exposed sites in people who tan easily or who have naturally dark skin. Lentigines are common after the age of 40 years, but they may also occur in younger people.
Solar lentigines are caused by UV radiation from exposure to the sun or other forms of UV radiation such as that involved in medical treatment (eg, phototherapy) or the use of tanning booths. On biopsy, a solar lentigo has a proliferation of keratinocytes, which form rete pegs, and there may be a mild increase in the number of melanocytes.
Solar lentigines tend to persist for long periods, and they do not disappear in the winter although they may fade. They vary in size from a few millimetres to several centimetres in diameter. Colour tends to be uniform across the lesion, with a yellowish or greyish light-brown hue. The border of the lesion is sharply defined, and an irregular border may give it a scalloped shape. They may have a dry or slightly scaly surface.
One or more seborrhoeic keratoses may arise from a solar lentigo.
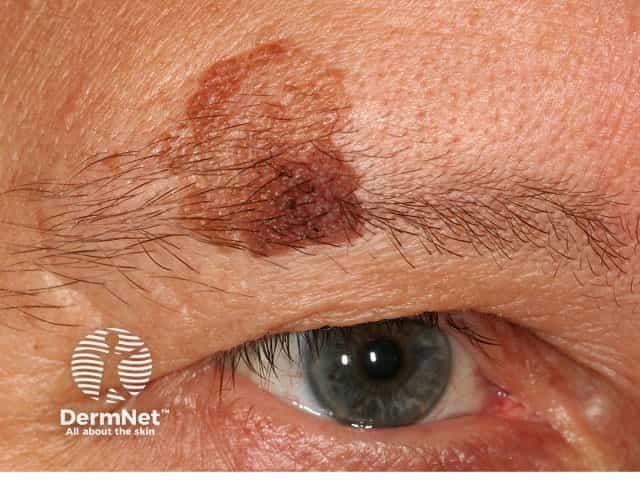
It is important to distinguish a harmless but atypical solar lentigo from an early melanoma and its subtypes, lentigo maligna and lentiginous melanoma. Lesions that are clinically, dermoscopically, or histologically atypical should be completely removed by surgical excision with pathological examination.
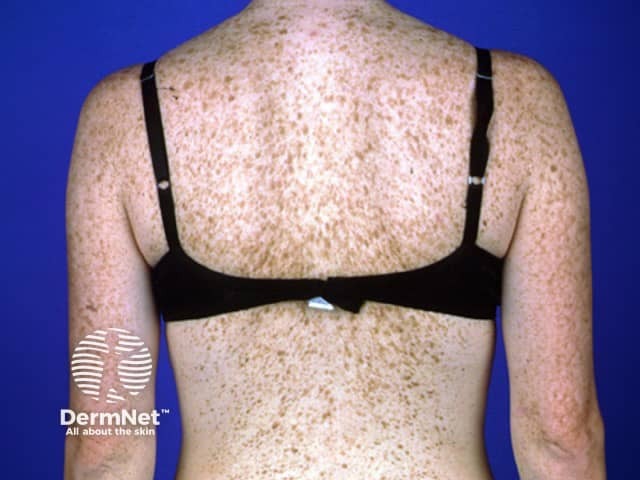
Lentigines
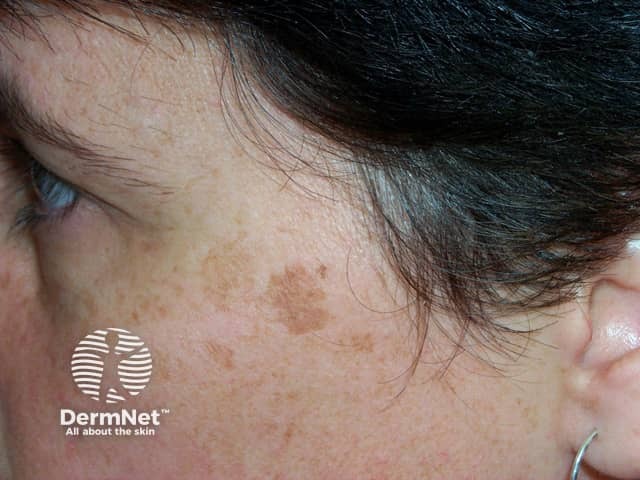
Lentigines
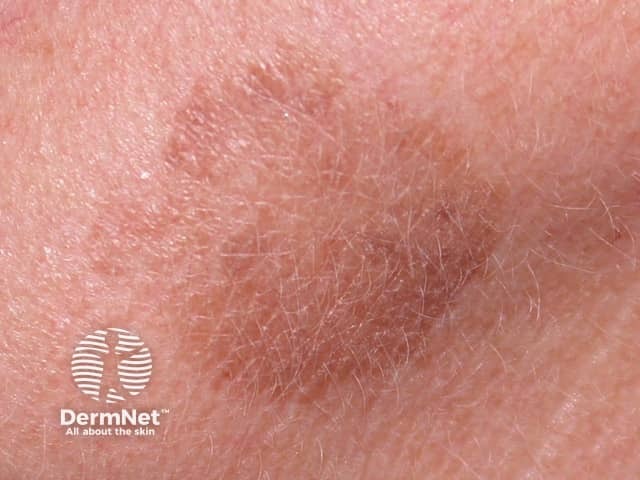
Lentigines
Most ephelides and lentigines can easily be diagnosed clinically by a health practitioner trained in examining the skin. If there is any doubt whether a brown mark may be a cancer, the lesion may be monitored (with digital dermoscopic surveillance) or excised for pathological examination.
A brown mark may also be an actinic keratosi (sun damage) or a seborrhoeic keratosis (senile wart) in which there are proliferations of keratinocytes. Actinic and seborrhoeic keratoses tend to be more scaly and thickened than solar lentigines. Facial pigmentation may also be due to melasma, a chronic pigmentation disorder.
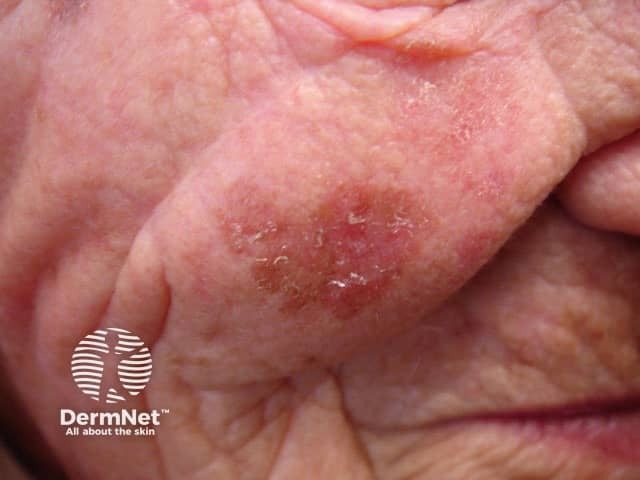
Actinic keratosis
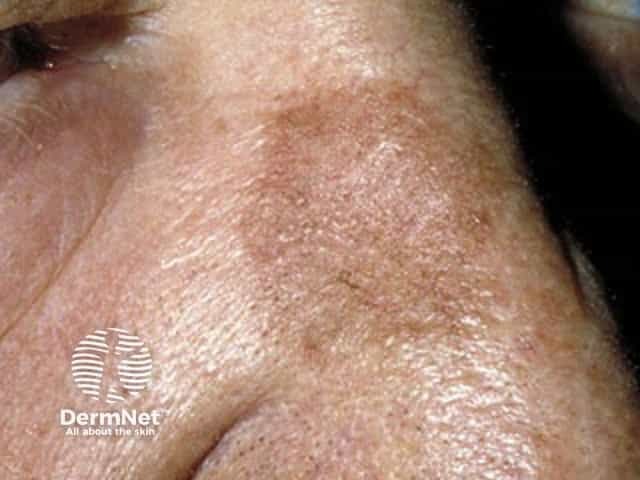
Actinic keratosis
Seborrhoeic keratosis
Not all brown marks on the skin can be prevented. Careful sun protection will reduce the number of new solar lentigines. Staying out of the sun and using sun-protective clothing is much more effective than using sunscreens alone. Sunscreens must have a high sun-protection factor (SPF 50+) and good broad-spectrum cover, and they should be applied liberally and frequently.
Brown marks may fade with careful sun protection, such as applying a broad-spectrum sunscreen daily. Regular applications of anti-ageing or fading creams may also help.
These may contain hydroquinone or antioxidants such as:
Brown marks may be removed more rapidly and effectively by chemical peels, cryotherapy, or certain pigment lasers that target melanin in the skin. Multiple treatments are often necessary.
Suitable green-light devices to remove epidermal pigment include:
Suitable red-light devices that can be used to remove epidermal pigment include:
Intense pulsed light has a similar effect. Carbon-dioxide lasers and erbium:YAG lasers lasers vaporise the surface skin thus removing the pigmented lesions. A fractional laser may also be effective. More recently, picosecond lasers have begun to be used for the removal of epidermal pigment.
The results of laser and light treatment are variable but sometimes are very impressive with minimal risk of scarring.
With superficial resurfacing techniques, there is minimal discomfort and no down time but several treatments are often necessary. Treatment occasionally makes the pigmentation worse by causing postinflammatory pigmentation. Continued careful sun protection is essential, because the pigmentation is likely to recur the next summer.
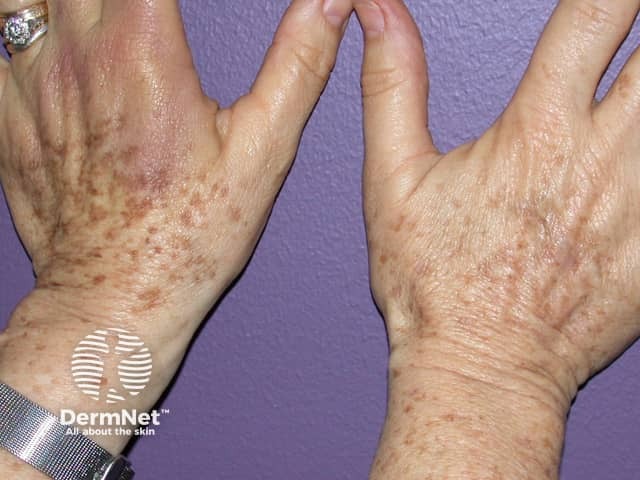
Freckles on hand before and after green laser light
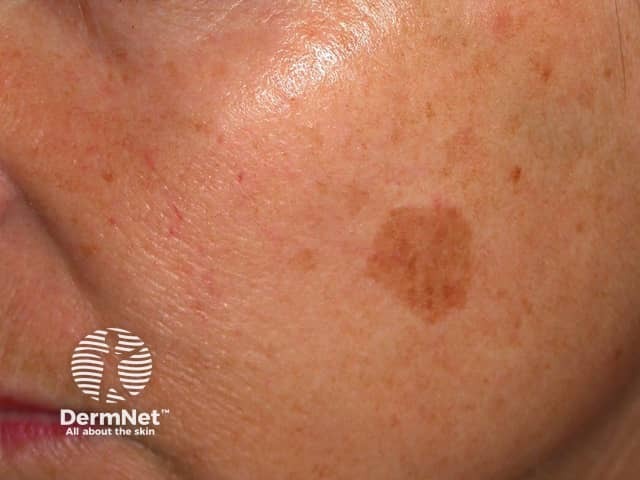
Freckle before cryotherapy
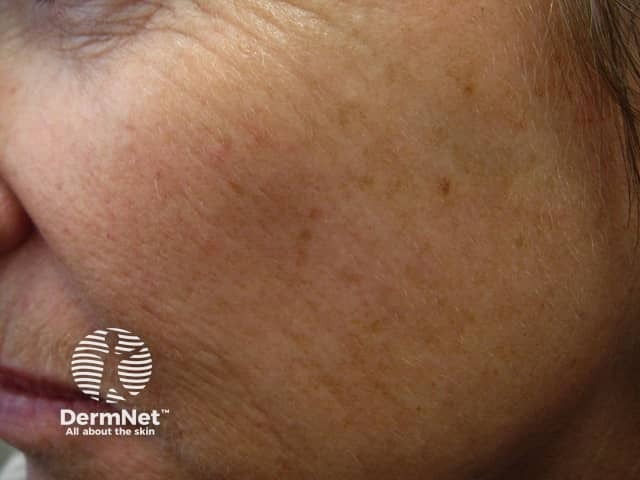
Freckle before cryotherapy