What are the common terminology criteria for adverse events?
The common terminology criteria for adverse events (CTCAE) describes a grading system for adverse event reporting associated with cancer therapy.
Tell me more about the common terminology criteria for adverse events
The CTCAE were developed in 1982 by the US National Cancer Institute (NCI) to collect standardised treatment-related data about adverse events to help evaluate new cancer therapies.
- The current version (5.0) of the publication about the criteria was published in 2017. Version 6.0 is under development at the time of writing.
- Its development has been assisted by various regulatory agencies, international clinical trial groups, representatives from the pharmaceutical industry, and researchers.
- The criteria are grouped by anatomical and physiological systems using the system organ class from the Medical Dictionary for Regulatory Activities (MedDRA) hierarchy.
Who uses the common terminology criteria for adverse events and why?
The CTCAE are widely used by oncologists, other internal medicine specialists, and researchers involved in cancer therapy clinical trials.
- This provides an objective framework to assess toxicity, by assigning grades, to ensure consistent reporting in clinical records and trials and enable comparison between drugs.
- An important function is to provide guidance and homogeneity in criteria for drug dose reductions and discontinuations for skin toxicity.
In oncology, there are a host of new active therapies including targeted agents and immunotherapy which cause skin toxicity. Dose delays and reductions, or in the case of immunotherapy, high-dose steroids to ‘turn off’ the immune response, may influence the effectiveness of the oncology agent. The CTCAE provides a framework to ensure dose changes are done according to international recommendations.
Dermatological adverse events in the common terminology criteria for adverse events
Cutaneous adverse events are found in three sections of the CTCAE:
- Most are listed under ‘Skin and subcutaneous tissue disorders’
- Folliculitis and skin infections/cellulitis are listed under ‘Infections and infestations’
- Radiation dermatitis is listed in ‘Injury, poisoning and procedural complications’.
What is the grading system for the common terminology criteria for adverse events?
The CTCAE are classified as Grades 1 to 5:
- Grade 1: mild symptoms
- Grade 2: moderate symptoms limiting important activities of daily living, such as shopping, housecleaning, managing finances, food preparation, using a phone and managing transport such as driving or catching a bus.
- Grade 3: severe or limiting symptoms preventing self-care such as dressing and undressing, eating, walking around, getting in and out of bed, using the toilet and showering
- Grade 4: life-threatening symptoms
- Grade 5: death.
Body surface area (BSA) has been incorporated into grading dermatological adverse events:
- Grade 1: involves <10% BSA
- Grade 2: involves 10–30% BSA
- Grade 3: involves >30% BSA.
Not all grades are appropriate for a particular adverse event, for example:
- Alopecia and telangiectasia have grades 1 and 2
- Stevens-Johnson syndrome/toxic epidermal necrolysis is classified as Grade 3 if <10% BSA is affected and Grade 4 if >10% BSA is affected.
Some examples of cutaneous adverse events from CTCAE are listed below.
A single dash (-) indicates a definition is not available.
Alopecia
- Grade 1: hair loss of <50% of the individual’s normal hair that is not obvious from a distance but is seen on close inspection; a different hairstyle may be required to cover the hair loss but the patient does not require a wig or hairpiece for camouflage.
- Grade 2: hair loss of ≤50% of the individual’s normal hair that is readily apparent to others; a wig or hairpiece is necessary if the patient desires to camouflage the hair loss completely; having a psychosocial impact.
- Grade 3 to 5: -
Oral mucositis
- Grade 1: asymptomatic or mild mucositis; intervention not indicated.
- Grade 2: moderate pain or ulcer that does not interfere with oral intake; modified diet indicated.
- Grade 3: severe pain; interfering with oral intake.
- Grade 4: life-threatening consequences; urgent intervention indicated.
- Grade 5: death.
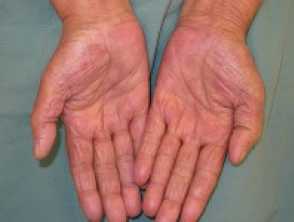
Hand-foot syndrome
- Grade 1: minimal skin changes or dermatitis without pain (eg, erythema, oedema, hyperkeratosis).
- Grade 2: skin changes with pain (eg, peeling, blistering, bleeding, fissuring, oedema, or hyperkeratosis); limiting instrumental ADL.
- Grade 3: severe skin changes (eg, peeling, blisters, bleeding, fissures, oedema, or hyperkeratosis) with pain; limiting self-care.
- Grade 4–5: -
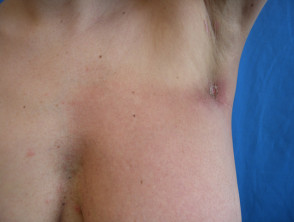
Maculopapular rash
- Grade 1: macules/papules covering <10% BSA with or without symptoms (eg, pruritus, burning, tightness).
- Grade 2: macules/papules covering 10–30% BSA with or without symptoms (eg, pruritus, burning, tightness); limiting ADL; rash covering >30% BSA with or without mild symptoms.
- Grade 3: macules/papules covering >30% BSA with moderate or severe symptoms; limiting self-care.
- Grade 4–5: -
Urticaria
- Grade 1: urticarial lesions covering <10% BSA; topical intervention indicated.
- Grade 2: urticarial lesions covering 10 - 30% BSA; oral intervention indicated.
- Grade 3: urticarial lesions covering >30% BSA; IV intervention indicated.
- Grade 4–5: -
Radiation dermatitis
- Grade 1: faint erythema or dry desquamation.
- Grade 2: moderate to brisk erythema; patchy moist desquamation, mostly confined to skin folds and creases; moderate oedema.
- Grade 3: moist desquamation in areas other than skin folds and creases; bleeding induced by minor trauma or abrasion.
- Grade 4: life-threatening consequences; skin necrosis or ulceration of full-thickness dermis; spontaneous bleeding from the involved site; skin graft indicated.
- Grade 5: death.