Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Amy Stanway, Department of Dermatology, Waikato (Feb 2004); Updated: Dr Aysha Rashid, Medical Registrar, Auckland; Associate Professor Paul Jarrett, Dermatologist, Middlemore Hospital and Department of Medicine, The University of Auckland, New Zealand (Aug 2021)
Infective complications of atopic dermatitis
Contact dermatitis and atopic dermatitis
Complications in skin colour
Other complications
Skin infection is very common in atopic dermatitis due to an inherently abnormal skin barrier, cutaneous and systemic immune system abnormalities, and scratching the itch. Cutaneous colonisation by Staphylococcus aureus forms a bacterial biofilm and worsens the dermatitis by promoting the Th2 allergic inflammatory response. Infants are particularly at risk of severe skin infections.

Impetiginised atopic eczema in teenager with skin of colour

Infection eczema

Infected eczema

Molluscum contagiosum

Molluscum contagiosum
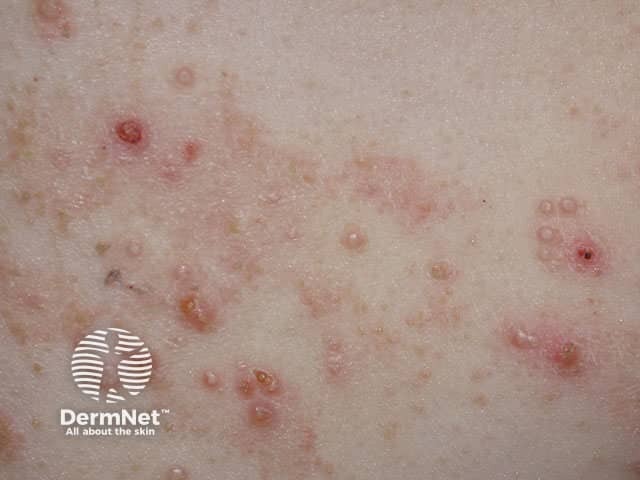
Molluscum contagiosum
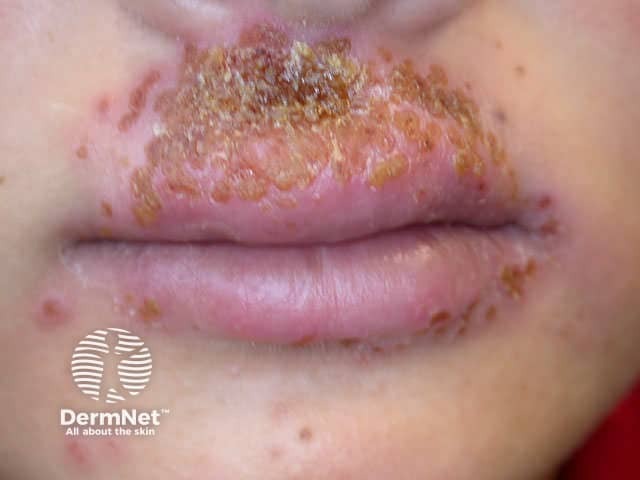
Eczema herpeticum

Eczema herpeticum

Eczema herpeticum

Tinea faciei
Contact dermatitis should be considered in the atopic patient with an otherwise unexplained dermatitis flare, particularly if in a patterned distribution.
Irritant contact dermatitis is particularly common with atopic dermatitis due to the abnormal skin barrier function. Atopic hand dermatitis and occupational skin disease are frequent manifestations.
The frequent use of multiple topical treatments for atopic dermatitis increases the risk of allergic contact dermatitis due to exposure to potential allergens. Aeroallergens also commonly aggravate other manifestations of atopy such as hay fever and asthma.

Contact dermatitis to ethylenediamine

Airborne contact dermatitis eyelid

Atopic hand dermatitis

Atopic dermatitis with dyspigmentation in young child with skin of colour

Papular atopic dermatitis with post-inflammatory hypopigmentation in teenager with skin of colour

Atopic dermatitis with dyspigmentation in child with skin of colour
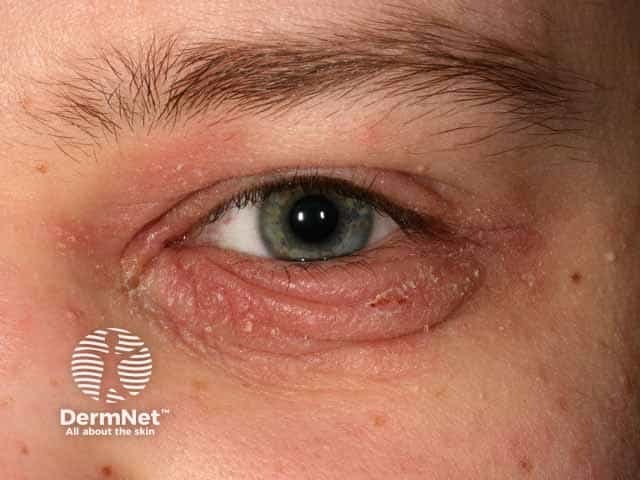
Blepharitis associated with atopic dermatitis
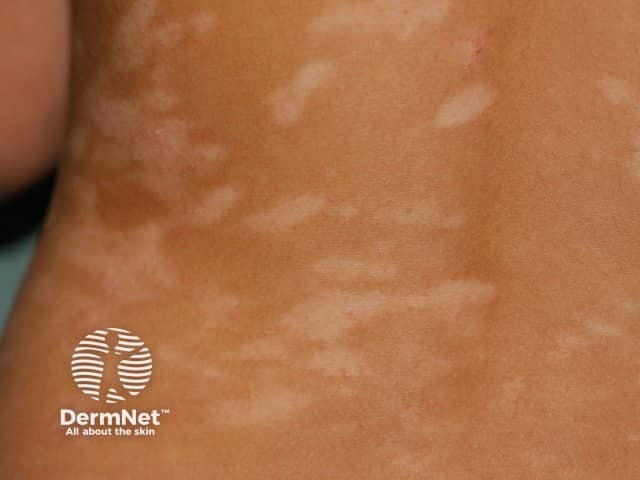
Postinflammatory hypopigmentation

Atopic hand dermatitis