Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Claire Felmingham, Resident Medical Officer, Rapid Creek, Australia; A/Prof Rosemary Nixon, Occupational Dermatology Research and Education Centre, Skin and Cancer Foundation Inc., Melbourne, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. October 2018.
Introduction Causes Normal skin barrier function Skin barrier function and atopic dermatitis treatment
Atopic dermatitis is a chronic, itchy skin condition that is associated with dry skin. It typically begins in infancy or childhood and is often associated with other atopic conditions, such as asthma and allergic rhinoconjunctivitis (hay fever) [1].

Atopic eczema
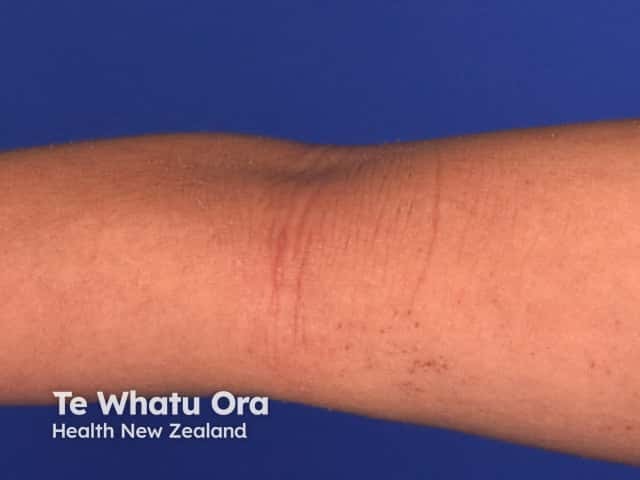
Atopic eczema
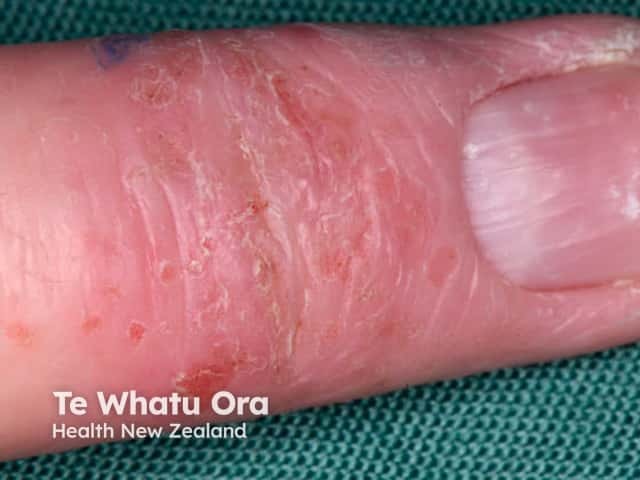
Atopic hand eczema
The causes of atopic dermatitis are incompletely understood. The underlying cause of atopic dermatitis is thought to be a result of a weakened skin barrier and a predisposition towards allergic inflammation [2]. Environmental triggers provoke an allergic reaction, which exacerbates the symptoms of atopic dermatitis.
The immunological disturbance arises from T lymphocytes, specifically T helper (Th) type 2 (Th2) cells in the acute phase, and Th1, Th17, and Th22 cells in chronic lesions. Th2 cells produce interleukin (IL)-4 and -13 (IL-13), which upregulate the production of immunoglobulin E (IgE) [3].
One theory of the pathogenesis of atopic dermatitis is the 'inside-outside theory', where the primary issue is thought to be with the immune system, and the skin barrier becomes dysfunctional secondary to the IgE sensitisation [4].
Another theory is the 'outside-inside theory', where the original defect is thought to be in the skin barrier, leading to increased allergen exposure and subsequent IgE sensitisation [4].
The skin barrier provides protection from external threats such as pathogens, chemicals, irritants, and allergens, which might cause an immune response if permitted to pass through to the deeper epidermal or dermal layers of the skin [see Structure of normal skin].
The skin barrier also protects the body from epidermal water loss, and skin barrier function can be measured by the rate of transepidermal water loss. Increased transepidermal water loss corresponds with increased skin permeability. Skin barrier function can sometimes also be measured by surface pH, the permeability of tracer compounds, and stratum corneum cohesion and hydration [2]. [see Skin barrier function]
The stratum corneum is the uppermost layer of the epidermis. The stratum corneum is comprised of a highly organised intercellular lipid matrix, and corneocytes (flattened cells without nuclei that are filled with keratin filaments); this is often referred to as the ‘brick and mortar’ of the skin, with corneocytes representing the bricks and the lipids representing the mortar [2].
There is altered stratum corneum homeostasis in both the lesional and non-lesional skin of patients with atopic dermatitis. This leads to increased water loss and the increased penetration of allergens [1].
In atopic dermatitis, the structure and composition of both the corneocytes and the intercellular lipid matrix of the stratum corneum can be affected in the following ways:
FLG is important for the structural integrity of the stratum corneum. FLG aggregates keratin filaments inside corneocytes and then helps to form a cornified cell envelope surrounding the corneocytes. The degradation products of FLG further contribute to the water-holding capacity and acidic pH of the stratum corneum. Maintaining the acidic pH is important to regulate the enzyme activity that leads to desquamation, lipid synthesis, and inflammation [2,5].
A loss-of-function mutation in the FLG gene is the strongest genetic risk factor for atopic dermatitis. FLG mutations are associated with an earlier onset of atopic dermatitis, greater disease severity, and persistence of disease. Approximately 50% of moderate to severe atopic dermatitis cases can be attributed to FLG mutations [5].
The activity of the serine proteases, such as kallikrein (KLK) 5 and seven is regulated by the pH of the stratum corneum. KLK5 and KLK7 cleave the extracellular corneodesmosomal proteins that link the corneocytes together. Their increased activity leads to decreased corneocyte adhesion and desquamation [6].
Normal skin pH is acidic and restricts the activity of these proteases, which are more active in alkaline environments. In atopic dermatitis, the pH of the skin is elevated, and subsequently so is the serine protease activity [7].
The stratum corneum lipid matrix is composed of three types of lipids — cholesterol, free fatty acids, and ceramides. These form a highly ordered structure of densely packed lipid layers. This intercellular lipid matrix is the main pathway for substances travelling across the skin barrier [2].
In atopic dermatitis, there is a reduction in total lipids, significant deficits of certain types of lipids, and changes in lipid composition. In combination, this leads to the impaired skin barrier function and increased permeability of the stratum corneum [2].
A defect in the skin barrier can facilitate the transport of allergens or haptens (molecules that only elicit an allergic reaction when bound to a protein) into the skin, inducing the release of proinflammatory cytokines causing inflammation of the skin [2].
At the same time, the Th2 cytokines IL-4 and IL-13, and the Th2 cytokine IL-22 downregulate the expression of FLG, causing further damage to the skin barrier [2,8].
The cutaneous microbiome is the pathogenic and commensal bacteria, fungi, and viruses that are resident on our skin and help maintain epidermal homeostasis [1].
More than 90% of patients with atopic dermatitis have skin colonized with Staphylococcus aureus [1].
When the stratum corneum is structurally competent, with an acidic pH, and a well-organised lipid matrix, it prevents colonisation with pathogens such as S. aureus, a bacterium that can detrimentally affect the barrier function. S. aureus surface proteins reduce free fatty acid production in the epidermis, leading to increased skin permeability. In patients with atopic dermatitis, S. aureus exotoxins with super-antigenic properties stimulate the production of IgE and cause pruritus. Subsequent excoriations create further defects in the skin barrier [4].
The understanding that skin barrier dysfunction drives disease activity in atopic dermatitis has resulted in increased interest and emphasis on treatments that improve barrier function.
Moisturisers are the main treatment for atopic dermatitis. Moisturisers that improve barrier function (barrier cream) have been shown to reduce relapse rates in atopic dermatitis with regular use [9].
Restoring skin barrier function may proactively prevent atopic dermatitis from developing or progressing, as has been shown in randomised control trials of neonates at risk of atopic dermatitis treated with a daily moisturiser [10,11].
Moisturiser ingredients that are helpful in atopic dermatitis include [2,12]:
Bathing with water can remove irritants, allergens, and squama (scales) in atopic dermatitis, allowing for repair of the skin barrier. The application of moisturiser soon after bathing is recommended. Non-soap cleansers, which are low in pH and hypoallergenic, are recommended as soap substitutes, as they cause less disruption to the stratum corneum structure and acid mantle [12]. Use of the 'soak and smear' technique (soaking the affected area in water before smearing it in the ointment) increases the effectiveness of topical medicines. The application of topical corticosteroids to wet skin, immediately after bathing, traps water in the stratum corneum and increases the amount of medication delivered by 10–100 times [13].
Bleach baths have proven helpful in decreasing clinical severity of atopic dermatitis, as a result of their antibacterial, antifungal and anti-inflammatory properties [14]. While sodium hypochlorite (bleach) is typically alkaline (pH 11–13), it produces hypochlorous acid (pH 2–7.5) when dissolved in water [15]. It is possible that this acidity helps maintain normal skin barrier function, in addition to acting as an antiseptic.
Other treatments sometimes required in atopic dermatitis include other topical anti-inflammatory treatments, such as:
In cases of severe atopic dermatitis, recommended treatments include: