Infective complications of atopic dermatitis
Skin infection is very common in atopic dermatitis due to an inherently abnormal skin barrier, cutaneous and systemic immune system abnormalities, and scratching the itch. Cutaneous colonisation by Staphylococcus aureus forms a bacterial biofilm and worsens the dermatitis by promoting the Th2 allergic inflammatory response. Infants are particularly at risk of severe skin infections.
Bacterial skin infections in atopic dermatitis
- Staphylococcal skin infection
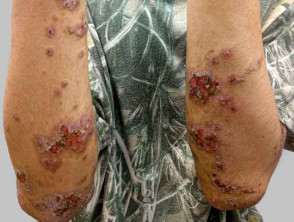
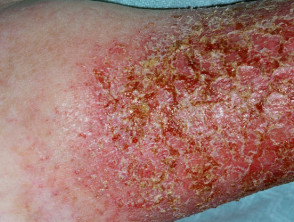
- Staph aureus causes impetiginisation of atopic dermatitis
- Streptococcal skin infection
- Strep pyogenes may cause impetigo, pustules, or punched out erosions with a scalloped border
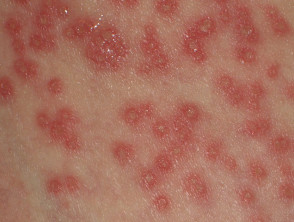
Bacterial infection and atopic dermatitis
Viral skin infections in atopic dermatitis
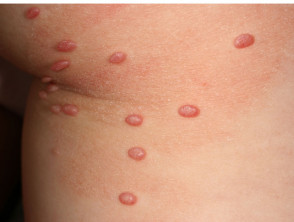
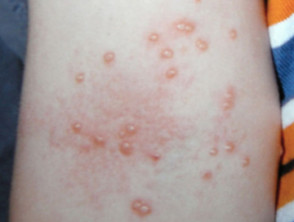
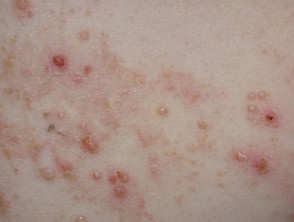
- Molluscum contagiosum
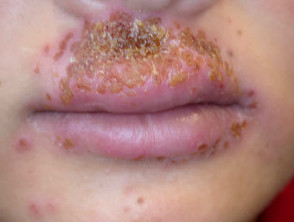
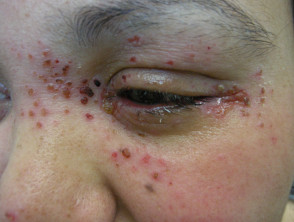
- Eczema herpeticum
- Eczema coxsackium
- Eczema vaccinatum
- Rare complication of smallpox vaccination
- Vesicular, pustular, or nodular rash after contact with vaccinia virus
Molluscum contagiosum infection and atopic dermatitis
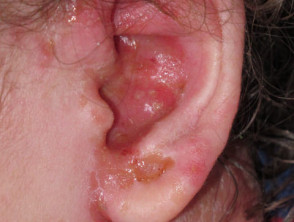
Eczema herpeticum
Fungal skin infections in atopic dermatitis
- Dermatophyte
- Trichophyton rubrum and Epidermophyton skin infection of the head and neck [see Tinea capitis, Tinea faciei]
- Yeast
- Malassezia furfur [see Skin conditions associated with Malassezia]
Fungal infection and atopic dermatitis
Complications of skin infections in atopic dermatitis
- Cutaneous abscess
- Septicaema/septic shock
- Osteomyelitis
- Septic arthritis/bursitis
- Bacterial endocarditis
- Herpes virus encephalitis
Contact dermatitis and atopic dermatitis
Contact dermatitis should be considered in the atopic patient with an otherwise unexplained dermatitis flare, particularly if in a patterned distribution.
Irritant contact dermatitis and atopic dermatitis
Irritant contact dermatitis is particularly common with atopic dermatitis due to the abnormal skin barrier function. Atopic hand dermatitis and occupational skin disease are frequent manifestations.
Allergic contact dermatitis and atopic dermatitis
The frequent use of multiple topical treatments for atopic dermatitis increases the risk of allergic contact dermatitis due to exposure to potential allergens. Aeroallergens also commonly aggravate other manifestations of atopy such as hay fever and asthma.
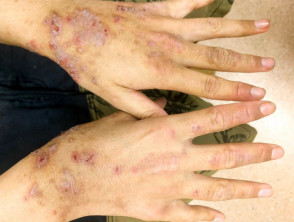
Contact dermatitis and atopic dermatitis
Complications of atopic dermatitis in skin of colour
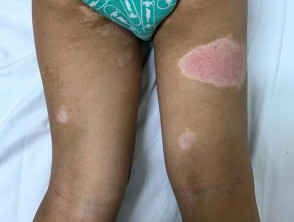
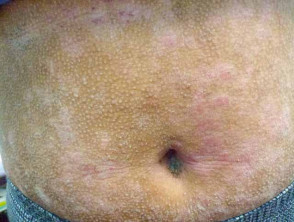
- Postinflammatory hyperpigmentation
- Postinflammatory hypopigmentation and leukoderma
- Vitamin D deficiency due to covering involved skin especially if extensive
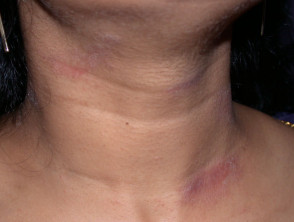
Dyspigmentation due to atopic dermatitis in skin of colour
Other complications of atopic dermatitis
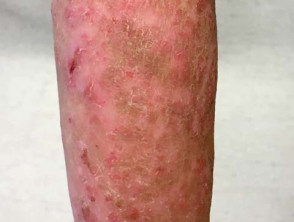
- Erythroderma and its complications in atopic dermatitis
- Psychological effects of atopic dermatitis
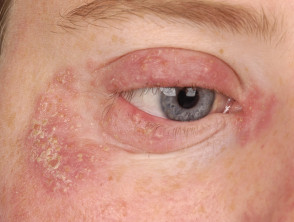
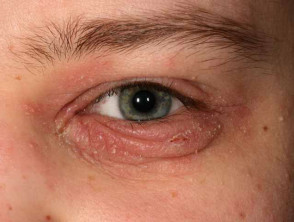
- Ophthalmological complications of atopic dermatitis
- Vernal keratoconjunctivitis in children
- Blepharitis, infectious keratitis, keratoconus
- Atopic keratoconjunctivitis in adults
- Corneal scarring, loss of vision
- Herpes keratoconjunctivitis in eczema herpeticum
- Cataracts
- Bilateral with characteristic appearance on eye examination
- Associated with severe atopic dermatitis
- Onset around age 15–25 years
- Vernal keratoconjunctivitis in children
- Growth
- Severe dermatitis may slow the growth rate of children
- Growth retardation can be due to the dermatitis itself and/or treatment such as systemic corticosteroids
- Dietary restrictions may affect growth and, in extreme cases, cause protein-energy malnutrition
Other complications of atopic dermatitis